A Pap smear, also known as a Papanicolaou test or Pap test, is a procedure that checks for abnormal cells on the cervix.1 It is named after George Papanicolaou, M.D., who is credited for developing the Pap smear.2 The Pap smear drastically transformed how early cervical cancer can be detected in females.2 The cervix is the lower part of the uterus that opens at the top of the vagina. Pap smears play a vital role in the early detection of abnormal cells in the cervix that may become cancerous and possibly lead to cervical cancer. Pap smears can also detect other conditions, which can include infections or inflammation.1 Pap smears are necessary in order to treat any abnormalities in a timely manner and maintain female reproductive health.
Procedure
The procedure will typically take place in a doctor’s office and be performed by a doctor.3 The procedure should only take a matter of minutes to complete.3 Before the procedure, the patient may be asked to undress completely or partially.3 The patient will then lie on an exam table and place their heels on stirrups, where their legs may be supported while their knees are bent for the procedure.3
To acquire the cell sample, the doctor will use a special instrument called a speculum to hold open the vaginal walls.3 This tool (pictured below) resembles a duckbill and is used to dilate the vagina so that the cervix is easily accessible.3 When the speculum is inserted, you may feel a pressure sensation in your pelvic region.3 The doctor will then gently brush the cervix with a cotton swab to remove a few cells. The cells are removed so that they may be screened for cervical cancer or any signs that may indicate the possible onset of cervical cancer.1 This sample of cells is put on a glass slide and sent to a laboratory to be tested. The swabbing is not painful because the cervix has few nerve endings. However, discomfort levels can differ depending on factors such as the anatomy of the patient and the skill of the practitioner. Most people tend to experience a mildly uncomfortable sensation, but this is completely normal. Following the procedure, most people are able to continue their day as normal.3 Before leaving the doctor’s office, it is a good idea to inquire when the results from the Pap smear can be expected.3 Although the name ‘Pap smear’ may be daunting, the actual procedure is very quick and easy, so there is no reason to worry!
Preparation
In order to get the most accurate results, take the following into account when scheduling a Pap smear appointment:
- Do not insert anything into the vagina for 24 to 48 hours prior to the Pap smear. This includes intercourse, douches, tampons, and any vaginal inserts. Inform your doctor before the appointment if you have recently performed any of these activities.
- Try to avoid scheduling a Pap smear during your period. Menstrual fluid may interfere with the accuracy of your results.
- Inform your doctor if you might be pregnant.4
- Inform your doctor of any medications you are taking.4 If you take birth control pills, this can possibly affect your test results.4
- Empty your bladder before the procedure.4
- If you have had a previous abnormal Pap smear results, inform your doctor. If you have copies of previous abnormal test results, be sure to bring them to your appointment.
- Schedule a follow-up appointment if you receive abnormal Pap smear results.
Preparing properly for your Pap smear test will contribute to more accurate results.
Frequency
Females should begin getting routine Pap smears within three years of becoming sexually active or by the age of 21. Females between the ages of 21-65 should get Pap smears about every three years or more frequently if recommended by their healthcare practitioner.4 Alternatively, you can instead obtain the test can be done every five years if you are over the age of 30 and you also have Human papillomavirus (HPV) testing done.4 However, both the Pap smear and HPV test must come back with normal results.4 Regular Pap tests can increase the probability of catching cancerous cells early so that treatment can begin as soon as possible. It is important for females who have already undergone menopause to continue to get Pap smears because they are still at risk of developing cervical cancer. However, screening may be discontinued for females ages 65 to 70 if they have had at least three consecutive normal Pap smears and have not received abnormal results within the past 10 years.4 If you have had a total hysterectomy, or have not had cervical cancer, pelvic cancer, or an abnormal Pap smear you may also need to get an examination.4 Pap smears are not foolproof, so regular testing increases the probability of discovering cancer early.
You can get a Pap smear at the following locations:
- Your doctor’s office
- A community health clinic5
- The health department5
- Your local Planned Parenthood Health Center5
The various locations available that perform Pap smears may allow females to obtain such tests routinely and in a timely manner.

Results
Once the cell sample has made its way to the laboratory, it is checked for abnormalities. Cells go through a series of changes before becoming cancerous, and these changes can occur up to 15 years before the actual cancer develops. The cells will be checked for these changes. It usually takes about 3 weeks to obtain the results from a Pap test. A negative Pap smear means that your results are completely normal and only normal cervical cells were found during your exam.4 A positive Pap smear, however, means abnormalities or unusual cells were detected from your Pap smear.4 About 5% to 7% of Pap smears produce abnormal results. Most of the time, abnormal Pap test results do not mean that you have cervical cancer.

If the Pap smear produces abnormal results, further tests are usually performed before a formal diagnosis is made. Testing or treatment that may follow your positive Pap smear results include a colposcopy-directed biopsy, an HPV test, a cervix cryosurgery, and/or cone biopsy.4
A colposcopy-directed biopsy includes having a colposcope, which is a binocular-like tool, magnifying the cervix.4 The colposcope does not go inside you nor touch you.6
An HPV test will check if HPV virus types are present, which may cause cancer.4 Cervix cryosurgery freezes and destroys cervical abnormal tissue.7 The doctor will insert a cryoprobe into the vagina and cover the abnormal tissue.7 Compressed nitrogen gas will then flow from the instrument so that the tissue will be frozen and destroyed.7
A cone biopsy removes a sample of abnormal cervical tissue.8 You will be asleep during the procedure, which will be done in the hospital or surgery center.8 A speculum will be inserted into your vagina and a small tissue sample, in the shape of a cone, will be removed from the cervix.8 The sample will then be screened for any indications of cancer.8 If all of the affected tissue is removed, this procedure may also be considered as a treatment for the underlying issue.8
Causes of Cervical Cancer
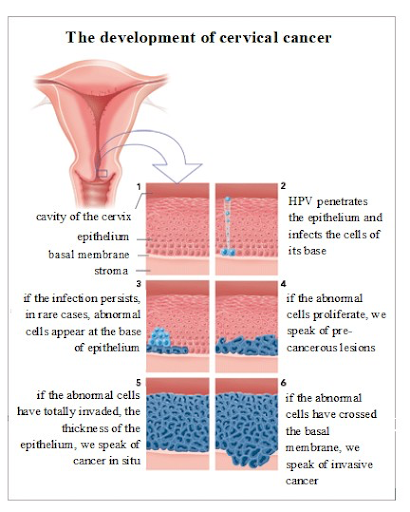
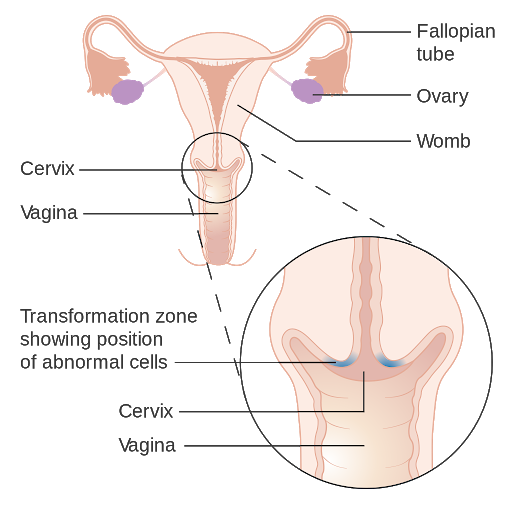
Normal cells in the cervix do not change into cancerous cells overnight.9 Instead, the normal cervical cells transform slowly into pre-cancerous cells that turn into cancer.9 A Pap smear can discover these changes and intercept the cancer development.9 Only some women with precancerous cervical cells will actually develop cancer.9 It is common for normal cervical cells to take several years to turn into cancerous cells, but it is possible for these cells to turn cancerous within a year.9 In a majority of cases, the precancerous cells will dissipate without treatment.9 However, it is still very much a possibility that these precancerous cells will develop into actual cancer.9
Most cervical cancer is caused by certain types of Human papillomavirus (HPV), which is transmitted through sexual contact with an infected person. Not all types of HPV cause cervical cancer, and many types of HPV are asymptomatic. If transmitted, the virus can cause abnormal cells to appear on the cervix. In some cases, the virus goes away on its own. However, if these cells are not discovered early they have the potential to turn into cervical cancer. Females should still be tested for cervical cancer even if they have been vaccinated against HPV since not all types of HPV that cause cervical cancer are prevented by the vaccines.10
Any female who participates in any kind of sexual activity is vulnerable to HPV. Besides getting regular screenings, consistently and correctly using condoms can greatly decrease the risk of developing cervical cancer. On the other hand, some factors that can increase the risk of cervical cancer include smoking, having an immune system weakened by HIV, chlamydia infection, a diet low in fruits and vegetables, being overweight, long-term use of oral contraceptives (birth control pills), intrauterine device, having multiple full-term pregnancies, being younger than 17 at your first full-term pregnancy, having taken Diethylstilbestrol (a hormonal drug), having a family history of cervical cancer, and economic status.11
Concluding Remarks
Pap Smears test for abnormal cells in the cervix that can lead to early detection of cervical cancer. Obtaining Pap smears in a timely manner contributes to good female reproductive health and can prevent the onset of cervical cancer with treatment. The procedure is quick and most people generally experience only mild pain. Females should begin routine testing once they reach the age of 21 or within three years of becoming sexually active. Only a small amount of Pap smears produce abnormal results and treatment is available. Using condoms, abstaining from smoking, eating a healthy diet, and maintaining a healthy weight are just some factors that can lower the risk of cervical cancer. Although the procedure may seem slightly daunting, it is imperative for females to get routinely tested in order to maintain overall general health—specifically reproductive health.
References
- “NCI Dictionary of Cancer Terms.” National Cancer Institute.
- Tan, Siang Yong, and Yvonne Tatsumura. “George Papanicolaou (1883-1962): Discoverer of the Pap Smear.” Singapore Medical Journal, Singapore Medical Association, Oct. 2015.
- “Pap Smear.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 25 July 2019.
- White, Cynthia D. “Pap Test.” MedlinePlus, U.S. National Library of Medicine.
- Planned Parenthood. “What’s a Pap Test?” Planned Parenthood.
- Planned Parenthood. “What Is a Colposcopy?: Procedure, Risks and Results.” Planned Parenthood.
- Jacobson, John D. “Cervix Cryosurgery.” MedlinePlus, U.S. National Library of Medicine.
- Jacobson, John D. “Cone Biopsy” MedlinePlus, U.S. National Library of Medicine.
- “What Is Cervical Cancer?” American Cancer Society.
- “HPV and Pap Testing.” National Cancer Institute.
- “What Are the Risk Factors for Cervical Cancer?” American Cancer Society.
Last Updated: 14 October 2019.
