Bacterial Meningitis is caused by inflammation of the meninges, the protective membranes surrounding the brain and spinal cord.1 A host of different strains of bacteria can cause meningitis, and people are more susceptible to certain strains at certain ages.1 Oftentimes, people carry the contagious bacteria, but do not show symptoms. However, if the bacteria break through the immune system’s defenses and travel through the bloodstream, they can infect the brain and create harmful swelling. Bacterial meningitis is most commonly spread in community settings, like college campuses, grade schools, military camps, and corrections facilities. Infants are at an especially high risk of contraction. There are an estimated 1.2 million cases and 135,000 resulting deaths worldwide caused by bacterial meningitis. Incidents most commonly occur during the winter or early spring.
Multiple other types of meningitis exist, including non-infectious, fungal, viral, and parasitic.1 While bacterial is the second most common form of meningitis, it is by far the most dangerous, and can be fatal if left untreated. Bacterial Meningitis is a medical emergency. If you believe you or someone you know is infected, seek medical attention immediately.
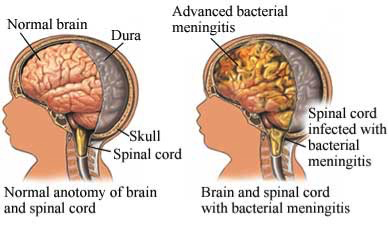
Table of Contents
Transmission
Bacterial meningitis is typically spread from person to person. Certain bacteria can spread through food, and others through stool.3 If you care for children, wash your hands regularly, and make sure your child does the same to avoid infection. Transmission commonly occurs through the mouth, nose, and throat secretions.3 It is not transmitted from sexual contact, including oral sex. Extreme caution should be exercised if you are in any kind of close proximity with an infected individual. The likelihood of contracting bacterial meningitis drastically increases if you live with someone who is infected or is a carrier.
Aside from direct contact (i.e. sneezing in someone’s face, French kissing, sharing food, etc.), secretions are typically only contagious in large droplets, since the bacteria cannot survive for more than a few moments outside the body.3 Simply having a conversation with an infected individual is no reason to be alarmed. Mothers can also contaminate babies with certain strains of contaminated bacteria during labor or birth.3 At any time, one in ten people carries the bacteria without ever developing symptoms. Though only a small number of people exposed actually get ill, any person carrying the bacteria can still be contagious until his or her body develops an immune response (a few days to a few months after infection).
Symptoms
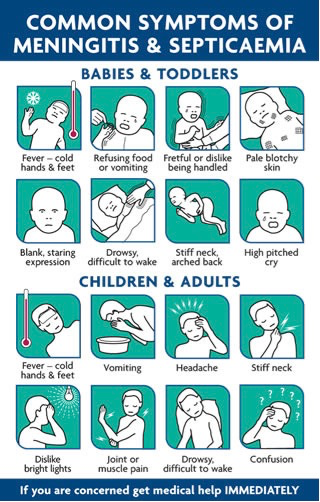
Meningitis infection is produced if the bacteria are able to cross the blood-brain barrier. This barrier normally prevents large molecules from entering the cerebrospinal fluid, allowing the brain to continue functioning optimally. Symptoms typically appear within the first 3-7 days of exposure, and can manifest suddenly, or over the span of a few days.1 Some common symptoms are listed below:
- Fever
- Nausea or vomiting
- Stiff neck
- Headache
- Increased light sensitivity
- Muscle pain
- Confusion
- In certain cases, a rash that does not fade under pressure
If bacterial meningitis goes untreated, it can result in seizures, coma, or death.1
Bacterial Meningitis and Infants
The Centers for Disease Control and Prevention recommends screening for bacterial meningitis during the third trimester of pregnancy (35 to 37 weeks). If any bacteria are found, the woman is given antibiotics to prevent infection to the newborn.
Infants are at a higher risk of contracting bacterial meningitis since their immune systems have not yet fully developed.3 Signs of infection in infants may include:
- Bulging of the soft spot on their head
- Lack of alertness
- Rapid breathing
- Excessing crying or a high pitched moan
- Stiffness or jerky movements
- Listlessness and limpness
If you believe your infant has been exposed to or is infected with bacterial meningitis, seek immediate medical attention.
Septicaemia
Blood poisoning, known as septicaemia, can also result from the bacterial infection. Septicaemia produces blood vessel leakage, interfering with the body’s ability to carry oxygen. Infants may exhibit the following symptoms:
- Pale skin
- Cold hands and feet
- Rapid breathing
In extreme situations, septicaemia can also cause the formation of blood clots. Large-scale tissue damage can lead to amputation or kidney failure. About one in five cases of meningococcal septicaemia are fatal, making it more lethal than meningitis.
Diagnosis and Treatment
Bacterial Meningitis is diagnosed using a blood sample or lumbar puncture.3 Depending on the bacteria causing the infection, a doctor will begin treatment immediately with a course of antibiotics, distributed either orally or intravenously.1 The antibiotics will reduce the spread of infection.2 Following immediate hospitalization, the patient will likely be given oxygen and resuscitation fluids. If the patient has septicaemia, these fluids will allow their blood volume to return to a normal level.2 The sooner treatment is begun, the greater the chance that it will be effective. Effective treatment can reduce the risk of death to below 15%.
Most survivors are left without long-term consequences. However, some are left with disabilities or problems after treatment. If the meningitis damages nerve cells, the person can be left with epilepsy, learning difficulties, problems with coordination or speech, or a change in behavior. If bacterial poisons damage the inner ear, the survivor can be left with deafness. Therefore, make sure the patient receives a hearing test within four weeks of treatment. These problems may disappear over time, but can be permanent in some cases. Meningococcal meningitis is less likely to produce long-term effects than the other types of bacterial meningitis. If behavioral changes are not disappearing, it may be helpful for the survivor to talk to a counselor.
Prevention
Vaccination is the most effective way to prevent infection. The primary vaccine in the U.S. is the meningococcal vaccine. All children should be vaccinated around the ages 11 to 12, and again at 16.3
There are vaccines for the three types of bacterial meningitis: Meningococcus, Pneumococcus, and Haemophilus influenzae type b (Hib). The meningococcal vaccine is recommended for college and high school students prior to entering a dorm. It is effective for three to five years, but does not protect against all strains of the bacteria. The vaccines are noninfectious, meaning that they can be administered during pregnancy or breastfeeding without harming the infant. If you have been exposed to someone with meningococcal meningitis, your doctor may recommend antibiotics in order to decrease the risk of infection and contagion.
Concluding Remarks
Bacterial meningitis is a potentially life threatening infection. If you or a loved one is diagnosed, all prescribed treatment should be followed closely, and taken very seriously. If you live in a community setting, vaccination is extremely important. Schools and college campuses in the United States even require students to be vaccinated. A vaccination is the most effective method of prevention.
References
- Nordqvist, Christian. “All about bacterial meningitis.” Medical News Today. MediLexicon, Intl., 30 Nov. 2017.
- Brouwer, M.C. “ESCMID Guideline: Diagnosis and Treatment of Acute Bacterial Meningitis.” ESCMID. Academic Medical Center, Department of Neurology, 7 April 2016.
- “Bacterial Meningitis.” Centers for Disease Control and Prevention. Nation Center for Immunization and Respiratory Diseases. 25 January 2017.
Last Updated: 10 May 2018.
