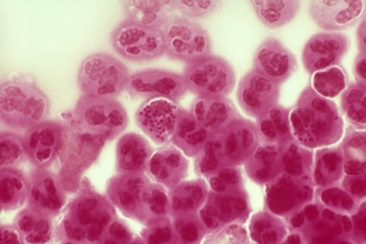
Gonorrhea, sometimes called “the clap”, is a sexually transmitted infection that can be spread to both males and females. It is a bacterial infection caused by the bacterium Neisseria gonorrhoeae, also called gonococcus.1 Gonorrhea is a very common infection in the United States and worldwide. The Centers for Disease Control and Prevention (CDC) estimates, that in the United States, about 820,000 people contract gonorrhea infections each year and the Public Health England (PHE) reports that in England the rate of the infection rose 25% between 2010 and 2011. Though the rates may be even higher since less than half of these new infections are detected.1,2 There also a more severe type of gonorrhea gaining prevalence called “super gonorrhea,” which is resistant to antibiotics. To learn more about super gonorrhea, read this article.
Table of Contents
Transmission
Gonorrhea is transmitted through any kind of unprotected penile-vaginal, oral-genital, oral-anal, and genital-anal contact with an infected individual. Therefore, any sexually active person is at risk for contracting gonorrhea. The bacteria can be spread even without penetration or ejaculation.1
Teenagers and young adults (ages 15-24) have the highest rates of gonorrhea infection and men who engage in sex with other men have reported having disproportionately higher rates of gonococcus.1 A 2015 report stated that people in Ghana, Africa who are: unable to have access to condoms, are engaging in sex at younger ages, and are less educated than others.2,3
Infants can also contract gonorrhea from an infected mother during childbirth.4
Symptoms
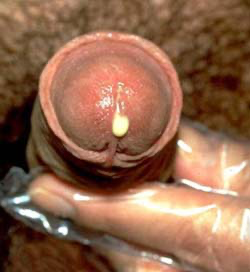
In males, symptoms will normally appear one to five days after exposure to the bacteria. It is possible for symptoms to take much longer to present themselves, and in about 10 to 15% of cases, the infection can be asymptomatic (expresses no symptoms).5 The two most common signs of gonorrhea are dysuria (burning during urination) and a cloudy, foul smelling discharge from the penis that is white, yellow, or green in color. Some males also notice tenderness or swelling in the lymph nodes of the groin. In severe cases, gonorrhea can be accompanied by epididymitis, which is characterized by pain in the testes or scrotum.1

Females are usually asymptomatic, about 80% of females who are infected do not notice any symptoms.5 When symptoms do appear, females usually experience dysuria, increased vaginal discharge (especially yellow or green in color), or vaginal bleeding. While these symptoms are typically irritating and concerning, they are often mistaken for signs of other health problems such as yeast infections, or bladder and vaginal infections.1
In both males and females, gonorrhea can also be found in the rectum and throat. Similar to genital gonorrhea, rectal and pharyngeal (oral) gonorrhea in both males and females may be asymptomatic. More specifically, 9 out of 10 throat gonorrhea will show no symptoms.1,4 Symptoms of anal gonorrhea include anal discharge, itching, soreness, bleeding, or painful bowel movements. The most common result of pharyngeal (mouth and throat) gonorrhea infection is a red, swollen, or sore throat.1
Diagnosis
If a person suspects that they may have gonorrhea, a doctor should be consulted immediately for a proper diagnosis since self-diagnosing can be dangerous. Testing for gonorrhea most often involves collecting urine samples or swabs of the cervix, vagina, urethra, rectum, or throat, and then searching for the bacterium Neisseria gonorrhoeae.1 These tests are usually low in cost and the samples can be tested for many other STIs such as syphilis and chlamydia. Test results are typically available anywhere from two to ten days after the test.6,4 For more information about getting tested, call your healthcare provider or local clinic.
Treatment
Gonorrhea is a treatable infection; however, certain strains of the infections are adapting, which makes treatment more difficult.4,5 This more advanced version of the infection is called “super gonorrhea” or antibiotic-resistant gonorrhea and is relatively rare. More research needs to be conducted on super gonorrhea to discover new ways to treat and prevent the occurrence of the super strain. A person who has been diagnosed by a doctor will be prescribed medications to treat it and since chlamydia infections often accompany gonorrhea infections, health practitioners may use a treatment that cures both.4 A patient must continue to take the prescribed medications until the regimen is completed, even if their symptoms have cleared up. Planned Parenthood recommends to get tested again 3 months after symptoms have disappeared to make sure the infection is fully gone.4 Although treatment of gonorrhea cures the infection, there is no cure for any permanent damage that the bacteria did to the body before it was treated.1
The sexual partners of an infected person are often likely to be infected as well. Therefore it is extremely important that anyone who is diagnosed with gonorrhea notify all sexual partners that they have been with up to two months before the date of diagnosis.2
People who are being treated for gonorrhea are advised to not have sex for at least seven days after the start of the treatment.5 Being treated for gonorrhea does not prevent a person from being re-infected if they come into sexual contact with an infected partner.1
Complications
If a person with gonorrhea goes without medical treatment it is very likely that complications will occur. For this reason, it is very important to seek medical treatment and complete any prescribed medication regimens even if symptoms have gone away.4
In Males
If gonococcal infection goes untreated for two to three weeks it can affect the prostate, bladder, kidneys, and testes. Most males who do not receive successful treatment may only experience occasional flare-ups, which involve a discharge from the penis and burning during urination. However, in a small number of men, untreated gonorrhea can lead to the formation of abscesses in the prostate, resulting in fever, painful bowel movement, and difficulty urinating. In males who remain untreated for more than a month, the bacteria can move into the epididymis causing epididymitis.1
In Females

If the bacteria moves from the genitals further into a female’s reproductive tract, Pelvic Inflammatory Disease (PID) can result. PID is an infection of the female reproductive organs. The most common symptoms of PID are abdominal pain and fever. If left untreated, it can lead to internal abscesses and chronic pelvic pain.1PID can also create bands of scar tissue that connect structures like the fallopian tubes, ovaries, and uterus to each other or to the abdominal walls. Women with PID may experience extreme pain when standing, walking, or engaging in coitus. The damage done to the fallopian tubes and uterus due to pelvic inflammatory disease is usually irreversible and can be severe enough to lead to ectopic pregnancy or infertility.1
Newborn infants can contract the gonococcus infection when passing through the birth canal of a mother infected with gonorrhea. The infection usually manifests itself as an eye infection, and can lead to blindness, joint infection, or a life threatening blood infection if not treated immediately.1,4
In Both Sexes
If the gonococcus bacterial infection is left untreated, it enters the bloodstream and spreads to the rest of the body, resulting in a condition called disseminated gonococcal infection (DGI). This systemic infection produces numerous symptoms such as fever, fatigue, chills, loss of appetite, arthritic pain in the joints, and skin lesions. Arthritic pain can cause permanent joint damage if not treated quickly. DGI is very uncommon, occurring in only about 2% of adult men and women with gonorrhea. Very rarely does the gonococcus bacteria invade the heart, liver, spinal cord, and brain. Although the chances of gonorrhea escalating to these extremes are low, the resulting health conditions are life-threatening, which is why it is so important to get gonorrhea treated immediately.1
A person with untreated gonorrhea is also at an increased risk for contracting HIV.1 This is because the inflammation or lesions in the mucous membranes from the gonococcus provides a convenient site for the transmission of the HIV virus.2
Prevention
Preventative measures can be taken to lower the chances of getting gonorrhea. Condoms, when used correctly, significantly reduce the risk of spreading and contracting STIs. Since gonorrhea can also be spread through oral sex, it is recommended to wear protection such as a condom or dental dam during oral sex. 2,4 Additionally, gonorrhea and other STI’s can be spread anally so a condom should be worn if engaging in anal sex. Effective communication with all long and short-term sexual partners about getting tested regularly can be crucial in ensuring that both people involved in a sexual relationship are uninfected.1
The only way to be 100% protected from gonorrhea and other sexually transmitted infections is to abstain from all oral, vaginal, or anal sexual activity.7
Concluding Remarks
Gonorrhea is one of the most common STIs in the United States and around the world. The infection can be spread through penile vaginal sex, oral sex and anal sex so it is important to always wear some sort of protection during any sexual activity. Symptoms may include white discharge and a burning sensation, however, some people with this infection will experience no symptoms. Fortunately, most cases of gonorrhea can be easily diagnosed and treated by a doctor.
References
1.”Gonorrhea – CDC Fact Sheet.” Centers for Disease Control and Prevention. N.p., 28 Oct. 2016. Web. 28 Feb. 2017.
2. Turner, Rosemarie, et al. “Diagnosis, Treatment and Prevention of Gonorrhea.” Nursing Standard, vol. 28, no. 27, 05 Mar. 2014, pp. 37-41. EBSCOhost.
3. Duplessis, Christopher, et al. “Gonorrhea Surveillance in Ghana, Africa.” Military Medicine, vol. 180, no. 1, Jan. 2015, pp. 17-22.
4. “Gonorrhea.” Planned Parenthood. N.p., 27 Apr. 2016. Web. 28 Feb. 2017.
5.”Gonorrhea Gonococcal Infection.” Department of Health. New York State, Nov. 2006. Web. 28 Feb. 2017.
6. “Gonorrhea.” BC Centre for Disease Control. Provincial Health Services Authority, n.d. Web. 28 Feb. 2017.
7. “Gonorrhea.” Mayo Clinic. N.p., 25 Oct. 2016. Web. 28 Feb. 2017.
Last Updated: 19 March 2017.
