Disclaimer note: While both males and females can be infertile, this article focuses on female infertility, its most common causes, and treatments. For information relating to male infertility click here.
Table of Contents
Overview of Female Infertility
Female infertility is defined as the inability to conceive or carry a pregnancy to term after 12 months of unprotected intercourse, or 6 months of unprotected intercourse if the female is over 35 years old. Typically, female infertility is linked to anatomical malfunctions or complications of the reproductive system, but can be caused by behavioral and environmental factors as well. Novel findings in the scientific community, combined with recent technological advancements, have made treating some forms of infertility possible.
According to researchers at Stanford University, infertility affects about 10 percent of females in the United States.1 Although identifying the source of infertility between partners can complicate estimates, the World Health Organization found that one in every four couples in developing countries has been affected by infertility. Furthermore, female infertility is ranked the 5th highest serious global disability among populations under the age of 60.2 It is difficult to find accurate statistics regarding infertility rates because there are numerous definitions, causes, and views of infertility. Many females do not know they are infertile until they begin trying to conceive. Even then, not becoming pregnant may be a result of other factors, such as stress.

Different Definitions
Infertility may be the result of many different factors, so it is helpful to understand the different definitions of infertility and the complications that can cause it. Listed below are a few of the main definitions used to understand infertility.
- Clinical Definition of Infertility: A disease of the reproductive system defined by the failure to achieve a clinical pregnancy after 12 months or more of regular unprotected sexual intercourse. 2
- Infertility as a Disability: Infertility generates an impairment of function, and thus access to health care falls under the United Nations Convention on the Rights of Persons with Disability preamble.2
- Primary Infertility: One form of infertility, primary infertility, is the case in which a female is unable to bear a child, either due to the inability to become pregnant or the inability to carry a pregnancy to live birth.2
- Secondary Infertility: This refers to infertility in which a female is unable to bear a child, either due to the inability to become pregnant or the inability to carry a pregnancy to live birth following either a previous pregnancy or a previous ability to carry a pregnancy to live birth.2
Knowing these definitions can help a female understand which type of infertility they may be experiencing and what the causes or treatments for it may be.

What Causes Female Infertility?
There are many different reasons why a female may be infertile. Age is a major cause of infertility because females are born with a finite number of eggs. Therefore, as a female gets older and the number and quality of their eggs decrease, they will have a harder time getting pregnant. Otherwise, primary infertility is typically due to anatomical complications or malfunctions that inhibit the ability to become pregnant. Secondary infertility is usually linked to damages of the reproductive system from invasive surgeries and infections. Although these are the most common causes of primary and secondary infertility, it is still possible for invasive surgeries to cause primary infertility and anatomical complications to cause secondary infertility.
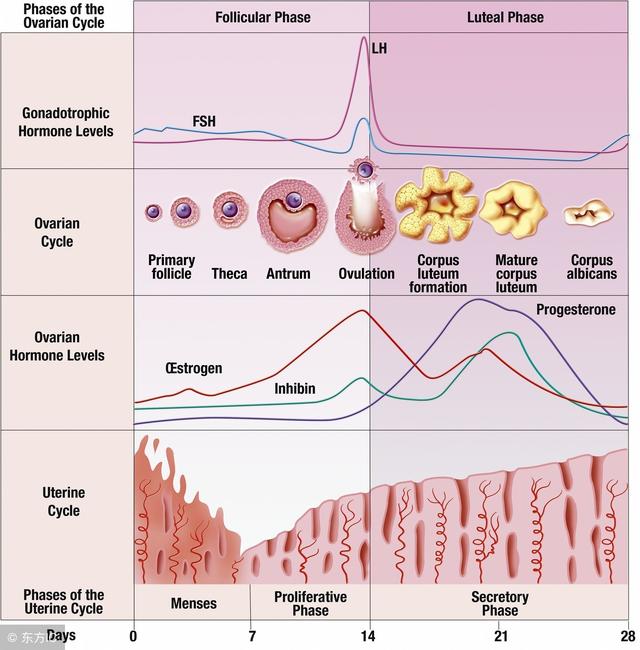
Infertility is most commonly linked to ovulatory disorders, which account for 30 percent of cases. Amongst other causes, ovulatory disorders may stem from hormonal problems, scarred ovaries, premature menopause, or follicle problems. Hormonal problems usually cause anovulation, which is key in understanding infertility. Anovulation is the lack of ovulation during a female’s menstrual cycle, so if ovulation cannot occur due to these hormonal complications, then it is impossible to become pregnant. Ovulation depends on a complex interaction of the Follicle Stimulating Hormone (FSH) and the Luteinizing Hormone (LH). FSH stimulates the ovarian follicle, which both causes the egg to grow and produces estrogen in the follicle. The rise of estrogen alerts the pituitary gland to halt FSH production and to produce more LH. Increased LH production causes the follicle to burst and release the egg from the ovary into the fallopian tube where it can be fertilized. If there is discrepancy in this chemical interaction, ovulation will be disrupted. Most commonly, these hormonal problems are linked to a malfunction of the hypothalamus, which is the part of the brain responsible for sending signals to the pituitary gland, or a malfunction of the pituitary gland itself, which produces and secretes FSH and LH. Physical damage to the ovaries may also result in failed ovulation.1 For instance, having multiple invasive surgeries for ovarian cysts can create a much higher risk of damaging the ovaries and losing the ability to ovulate.
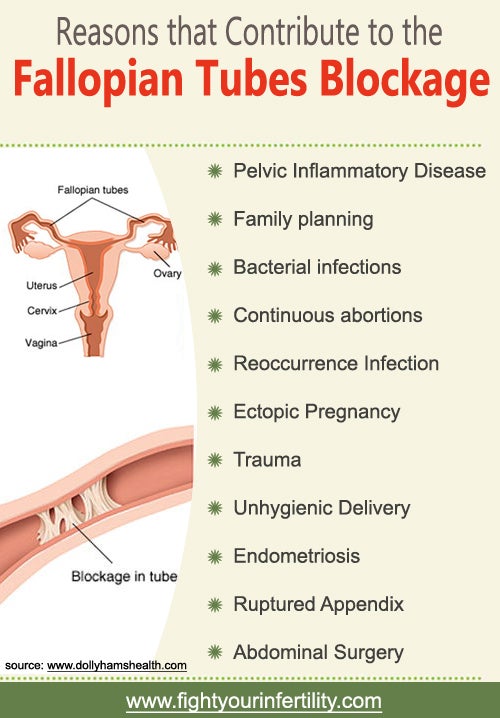
Tubal disease, which refers to poorly functioning fallopian tubes, affects approximately 25 percent of infertile females and varies widely, ranging from mild adhesions to complete tubal blockage.1 Tubal disease is typically linked to infection, abdominal disease, previous invasive surgeries, ectopic pregnancies, or congenital defects. Sexually transmitted infections (STIs) can cause inflammation of the fallopian tubes, which can lead to damage or scarring. Pelvic inflammatory disease (PID) is one specific way that the fallopian tubes can be damaged from STIs and cause infertility. Abdominal disease, such as appendicitis, also causes inflammation of the abdominal cavity that can lead to tube blockage.1 Invasive surgeries may also lead to infertility by causing tubal damage that restricts the egg from traveling through them. Ectopic pregnancy occurs when the fertilized egg implants into the fallopian tube itself rather than implanting in the uterus. Beyond infertility, the condition is also potentially life threatening. Congenital defects are another cause of infertility; in this case, the females are born with tubal abnormalities that cause problems with egg transportation and fertilization.
Endometriosis affects about 10 percent of infertile females.1 Approximately 30-40 percent of patients with the complication are infertile, which is two to three times the rate of infertility in the general population.1 Endometriosis is caused by abnormal growth of the endometrial tissue, which is the inner lining of the uterus. If the tissue spreads and grows outside of the uterus, infertility may occur depending on the severity of the abnormal growth. While the exact causes of endometriosis are unclear, retrograde menstruation is most probable. In this condition, the endometrial discharge travels backwards into the oviducts and becomes stuck in the pelvic cavity or irregular places outside the uterus.
There are also behavioral and environmental factors that can inhibit a female’s ability to get pregnant. For instance, females who are significantly overweight or underweight may have difficulty becoming pregnant.1 Therefore, diet and exercise is critical in maintaining a healthy reproductive system. Other behavioral factors include smoking, the use of alcohol and drugs, and involvement in stressful jobs or situations. Even the amount of exercise someone participates in can impact fertility. Exercising for more than 60 minutes a day can lead to an increased risk of anovulation.3 While these factors may or may not directly cause infertility, they can combine with anatomical malfunctions and decrease a female’s ability to become pregnant.
Environmental factors can also contribute to infertility, such as frequent exposure to various toxins or chemicals in the workplace or the surrounding environment.1 These substances are called reproductive toxins because they have the ability to cause mutations, birth defects, miscarriages, sterility, and infertility. Despite the considerable controversy that exists regarding the impacts of toxins on fertility, four chemicals are now regulated based on cases that found these toxins to be the main cause of the inability to get pregnant.1 These regulated reproductive toxins are lead, radiation, ethylene oxide, and dibromochloropropane (DBCP).
Testing for Infertility
Females should check with a doctor if they have been trying to get pregnant for a year with no success, have irregular periods, painful periods, no periods, endometriosis, PID, or more than one miscarriage.4 All of these circumstances could mean possible infertility.
There are a few ways to test for infertility. A female can check her own fertility at home by checking her body temperature every morning and looking at her cervical mucus over a period of a few months. A doctor can also do an ultrasound of the female’s ovaries, blood tests to check ovulation, an x-ray of the uterus and fallopian tubes, or a minor surgery called a laparoscopy, which looks inside the abdomen.4 In the x-ray, dye is injected into the uterus, so the doctor can see how it moves in the uterus and fallopian tubes. If the dye is blocked from moving, this can be a sign of a blockage that may be causing infertility. The laparoscopy involves the doctor using a tool to look at the ovaries, uterus, and fallopian tubes. Testing for infertility can take months and be a difficult time for those involved.4 Problems with fertility can cause many emotional and relational difficulties but, depending on the cause and severity of each case, there may be many treatment options.
Treating Infertility
Advancements in modern technology and medicine have evolved to provide some females who were infertile with the ability to become pregnant. Anatomical complications can be corrected by both surgery and medicine. In some cases, if infertility is due to the behavioral factors listed above, simple changes in lifestyle can create the ability to become pregnant. If the female is indefinitely infertile and treatment is not possible, then they can seek a surrogacy or gestational carrier agreement.
Surrogacy is when a male’s sperm is combined with a surrogate female’s egg and the surrogate carries the baby, rather than the infertile female. In these situations, the infertile mother does not share DNA with her baby. A similar situation occurs when a couple uses a gestational carrier rather than a surrogate. In this case, the infertile female’s egg is combined with her partner’s sperm and the embryo is then implanted into another female who carries the baby to term. In this situation, both parents will share DNA with their child.4 Both surrogacy and gestational carrying are forms of assisted reproductive technology (ART).

Other forms of ART include in vitro fertilization (IVF) and intrauterine insemination (IUI). IVF is a procedure in which the egg and sperm are combined outside the body and then inserted back into the female. IUI, also known as artificial insemination, is a process in which sperm is injected into the female. The female sometimes takes medicine that helps with ovulation before this process. IUI is often used if a female has problems with her cervical mucus.4
ART is between 11-39 percent effective, depending on the age of the female. As females get older, the technology is less likely to lead to a live birth.4 For more information on ART, click here.
Ovulatory disorders can be treated using drugs such as Clomiphene® and Menogan/ Repronex®, which have been noted to have a 70 percent success rate.1 Tubal disease is commonly treated by surgeries using lasers and microsurgery technology with success rates (defined as the number of females who become pregnant within one year of surgery) as high as 30 percent overall, while certain procedures can be up to 65 percent successful.1 As for endometriosis, treatment relies on the severity of the condition and the symptoms. Anti-inflammatory pain relievers, such as ibuprofen, can help manage the pain, while birth control pills or other hormonal medications can control the growth of the endometrial tissue, reduce inflammation, and overall reduce the impact that endometriosis has on fertility. Surgery can also correct endometrial complications depending on the tissue’s growth and location.
Concluding Remarks
Female infertility has many different anatomical and behavioral causes. Dealing with infertility can be a long and painful journey, but medical advancements have provided ways to treat or help with the issue. Depending on the cause and severity of each case, females dealing with infertility may have options for medical treatments or ART available to them if they do want to have a child. Infertility is also not just a female issue and other factors may be involved, including problems with the male’s reproductive functions.
References
- University, Stanford. “Infertility Treatment.” Stanford Edu. Stanford Education, 2012. Web.
- World Health Organization. “Infertility.” WHO.com. World Health Organization, 2015. Web.
- Hakimi, O & Cameron, LC. “Effect of Exercise on Ovulation: A Systematic Review.” ncbi.nlm.nih.gov. US National Library of Medicine, 2017. Web.
- Office on Women’s Health. “Infertility.” Office on Women’s Health, 2018. Web.
Last Update: 09 February 2019.
