
Polycystic ovary (or ovarian) syndrome, also known as PCOS, is the most common endocrine ailment affecting people with uteruses, impacting about 8-13% of adults of reproductive age and approximately 6-18% of adolescents.1 PCOS is caused by an imbalance in an individual’s androgen hormone levels. This hormonal imbalance can cause a number of issues, including difficulty achieving pregnancy, by creating an irregular menstrual cycle.2 During ovulation, those with PCOS do not produce all the hormones necessary for their eggs to fully mature. In some cases, this causes a portion of the eggs to remain in the fluid-filled sacs in which they were produced, which leads to the formation of cysts in the ovaries. Though more often than not, these cysts remain small and are not harmful, in rare instances, a cyst may rupture or twist an ovary, resulting in severe abdominal pain as well as nausea and vomiting.3 However, the presence of cysts on the ovaries can create hormone imbalances, making PCOS the most common cause of infertility in people with uteruses.2
Table of Contents
Causes of PCOS
The causes of polycystic ovary syndrome are unknown; however, certain factors, such as genetics or insulin levels, may play roles in its formation.2 One of the most prominent characteristics of this condition is hormonal imbalance. The body overproduces androgen, the group of male sex hormones, which impedes the development of the hormones responsible for ovulation, such as estrogen and progesterone.4 PCOS destabilizes the balance of these sex hormones, resulting in irregular ovulation and menstruation. Experts have hypothesized that the following factors may have an impact on the development of PCOS.
Excess Insulin
Insulin is a hormone that enables the body to convert the sugars that one ingests throughout the day into energy. Insulin is produced in the pancreas and gives the body’s cells the ability to process and utilize sugar. If an individual is diagnosed with type 2 diabetes, their body has developed an insulin resistance, blocking them from processing insulin properly. As a result, the pancreas produces excess amounts of insulin to overcompensate for the cells’ inability to use this hormone effectively; this overproduction of insulin, in turn, allows the body to acquire the necessary amount of glucose (sugar) to one’s cell. The excess insulin levels in someone with type 2 diabetes may result in the ovaries overproducing androgen, leading to altered ovulation. 5
Low-grade Inflammation
Inflammation occurs when the body’s immune system sends inflammatory cells and cytokines to combat foreign agents or help heal an injury. This leads to a rush of blood swelling the affected area in order to fight infection.6 Research has shown that individuals with PCOS are at an increased risk of both coronary heart disease and type 2 diabetes. These conditions often result in low-grade inflammation, which may influence polycystic ovaries to produce more androgen.
Genetics and Environment
Researchers are studying the possibility that certain genes are linked to PCOS, based on the observed pattern that a person is more likely to have this condition if their parent or sibling has PCOS as well.7 Many scientists also hypothesize that the environment one grows up in plays a decisive role in whether or not a person with a uterus will develop PCOS. For instance, issues during pregnancy, such as diabetes or maternal hypertension, may result in the baby being born abnormally small. These children are predisposed to insulin resistance and obesity, exacerbating the possibility of developing PCOS later in life. Exposure to anti-epileptic and mood stabilizer medicine during pregnancy may also be linked to PCOS.8 These observations do not indicate a direct relationship between genetics or the environment and PCOS, but it is worthwhile to talk to a physician about one’s family history and mother’s habits during pregnancy when being assessed for PCOS. While an exact cause of PCOS is uncertain, each of the aforementioned factors may play a key role in the development of this condition.
Symptoms of PCOS
PCOS affects people as young as eleven years of age. Between 1 in 10 and 1 in 20 individuals with uteruses of childbearing age have PCOS, and this syndrome affects up to 5 million people in the United States.7 PCOS-like symptoms usually appear soon after a person’s first menstrual cycle. However, the syndrome may also develop later in life, commonly after a considerable weight gain. One of the main consequences of this syndrome is an excess production of androgen, which is produced only in small amounts in unaffected individuals. This hormone imbalance can affect the body in several ways.2 It is possible that one or more of the following symptoms will accompany a diagnosis of PCOS:
- Infertility, due to lack of ovulation
- Irregular, infrequent, and/or absent periods; typically less than 8 a year
- Cysts in the ovaries
- Anxiety or depression
- Weight gain (especially around the waist)
- Hirsutism (excess hair growth) on the face, chest, stomach, back, and tops of thumbs and toes
- Acne (typically most severe on the face and back) and oily skin
- Dark patches of skin (usually on neck, arms, breasts, or thighs)
- Dandruff
- Thinning hair (male-pattern baldness)
- Skin tags (excess flaps of skin in the armpits or neck area)
- Pelvic pain
No two experiences are alike. PCOS manifests differently in many people who are diagnosed, so it is possible for one to experience a combination of some or all of the aforementioned symptoms or to only encounter one of them.
How PCOS Affects the Menstrual Cycle
The hormonal imbalance that accompanies PCOS is the main cause of the irregularity or absence of menstruation. An afflicted individual’s body produces excess androgens which affect the development and release of eggs during ovulation. This process usually starts in the ovaries, where eggs are produced. They begin as small fluid-filled sacs called follicles or cysts, which build up fluid as an egg develops inside. Normally, when the egg fully matures, the follicle ruptures and releases the egg which then travels down one of the fallopian tubes into the uterus to be fertilized by sperm. However, in people with PCOS, the excess androgens disrupt this process. The affected follicles begin to grow, but never properly rupture and release the egg, so they remain as cysts.9 Their failure to release eggs results in a lack of ovulation and a decrease in the production of the hormone progesterone. Without progesterone, a person’s menstrual cycle will be irregular or absent.7
An absent or irregular period and low progesterone levels mean the thickened endometrial lining of the uterus does not shed each month, as it does during typical menstruation. As a result of impacted ovulation, the endometrium continues to build up, making subsequent periods more painful. Essentially, the uterus often cramps more intensely in an effort to rid itself of the excess lining. The flow of these abnormal periods is also likely to be heavier than normal periods. If the endometrium continues to build up without subsequent shedding, the individual is at a higher risk of developing endometrial cancer.10
PCOS During Pregnancy
PCOS is the most common cause of infertility in people with uteruses because it disrupts the natural cycle of ovulation. There are a multitude of ways to help stimulate the development of follicles to jumpstart ovulation in patients with polycystic ovaries. There are many fertility medications available that can help hopeful parents become pregnant and carry the baby to term. These include Clomiphene (oral), Femara (oral), Metformin (oral), Gonadotropins (injection), and in-vitro fertilization (invasive), to name a few. Each treatment has varying success rates and may not work for everyone. Individuals should consult with their doctors to determine which treatment best suits their needs.11

Once a person with PCOS becomes pregnant, they often face a much higher risk of the following complications:
- Miscarriage
- Gestational diabetes
- Premature delivery
- Preeclampsia (pregnancy-induced high blood pressure)
A person with PCOS may not ever experience these complications, and for those who do find themselves facing these challenges, there are a number of effective resources and treatments available to help create a smooth pregnancy.
Effects of PCOS at Menopause
A few of the symptoms caused by PCOS, such as irregular or infrequent periods, are no longer a concern once a person reaches menopause. However, PCOS affects many systems in the body, so oftentimes its symptoms will persist despite menopausal changes altering ovarian function and hormone levels. Following menopause, excess hair growth often continues and male-pattern baldness (or thinning hair) tends to worsen. Further, the risk of other health complications such as strokes, diabetes, and heart attacks increases.2
Other Complications
Patients with PCOS have a higher risk of developing other serious health conditions.2 These include the following:
- Hypertension (high blood pressure)
- High cholesterol
- Heart attacks
- Diabetes
- Sleep apnea (when a person stops breathing periodically during sleep)
- Breast cancer
- Endometrial cancer
- Anxiety or depression
- Eating disorders 12

The effects of anxiety and depression on individuals with PCOS are often overlooked. Fluctuating hormones can have a profound impact on the emotional states of people with this condition.9 It is also possible that the degree of anxiousness or depressive symptoms some people feel may increase as they deal with the full impact that the symptoms of PCOS may have on their life, such as infertility, unpredictable menstruation, and fluctuating body image. It can be very helpful for those afflicted with PCOS to communicate with family and friends and to consult professional physicians when dealing with these challenges.
Diagnosis
There is not a singular test that is administered in order to diagnose PCOS. To identify this condition, a doctor will look for at least two of the following.2
Irregular Periods
Most people who menstruate experience a period every 28 to 32 days. If an individual has PCOS, their menstrual cycles tend to last over 35 days.13 Doctors also look for fewer than eight menstrual cycles in a year, with absent menstruation spanning at least 4 months. These periods can either be extremely light or heavy. This is the most common symptom, and it can manifest in two different ways.
Oligoovulation
This condition causes irregular menstruation in people with uteruses, resulting in fewer periods taking place each year than is considered healthy. Due to the infrequent nature of an inflicted individual’s menstruation, the chances of infertility rise significantly.13
Anovulation
This condition occurs when the egg (or more formally, ovum) is not released from the ovary during menstruation, resulting in irregular periods. Due to the egg’s key role in fertilization, its absence makes it considerably more difficult to get pregnant. A person with anovulation may experience irregular uterine bleeding, but these instances are not classified as menstruation, for ovulation has not taken place. Approximately 70% of anovulation cases are associated with PCOS.14
Hyperandrogenism
A doctor identifies hyperandrogenism by testing for high levels of androgens in the body. The excess androgens most commonly manifest in the form of testosterone. Additional indicators of excess androgen include hirsutism (excess hair growth on the body and face), severe acne, and male-pattern baldness. The majority of hyperandrogenism patients will be diagnosed with PCOS at some point in their life.15
Polycystic Ovaries
An ultrasound can detect the presence of polycystic ovaries, which become enlarged due to fluid-filled follicles surrounding the eggs. These cysts are often harmless and remain small, but there are cases of ovarian cysts growing several centimeters and causing discomfort to the individual with PCOS.16
In order to detect these symptoms, a doctor may also want to ask about the following information or administer the following tests in order to fully confirm the presence of this syndrome:2
Medical History
A doctor may ask about the frequency of a patient’s menstrual cycle, potential weight gain, difficulty achieving pregnancy (if they are attempting to conceive) as well as other symptoms such as hirsutism, pelvic pain, or acne outbreaks. Diet, frequency of exercise, and lifestyle may also be a topic of discussion, as eating disorders and obesity are known to exacerbate the symptoms of PCOS.12
Blood Tests
A doctor may screen for increased androgen levels (which often manifest in the form of excess testosterone in people with vulvas), as well as decreased glucose levels, which may be a sign that the body is producing excess insulin (which is often an indicator of type 2 diabetes). The physician may request a full hormone profile in which the reproductive hormones are assessed throughout different days of one’s cycle to determine whether hormone imbalance or dysregulation is present.16
Physical Exam
A doctor may check a patient’s BMI (body mass index), BP (blood pressure), and waist size. They will also look for potential physical indicators such as excess hair growth (letting hair grow naturally prior to exam often aids this identification), skin tags, severe acne, signs of male-pattern baldness, or dark patches on the neck, arms, breasts, and thighs.
Ultrasound
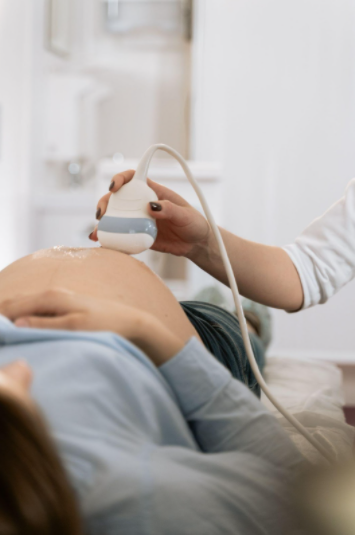
A doctor may administer an ultrasound, in order to detect and measure ovarian cysts. This test is also the easiest way to measure the thickness of the endometrial lining. The provider may request a transvaginal ultrasound in which the ultrasound transducer is inserted into the vagina to help effectively see the internal structures of the reproductive system; this technology allows each individual follicle to be counted and measured, making it the most precise method of diagnosing PCOS. If a patient prefers not to undergo an invasive exam, the provider may recommend a transabdominal ultrasound. This procedure requires the patient to have a full bladder to allow the ovaries to be more easily seen. The ultrasound transducer is subsequently pressed along the outside of the abdomen to produce images of the pelvic organs.17
While there is no single test to determine the presence of PCOS, each of these diagnostic methods help narrow down the symptoms and determine whether or not a person is being affected by this condition.
Treatment
Unfortunately, PCOS has no cure, but its symptoms can and should be managed in order to avoid future complications. Treatments vary and depend on a number of factors, including how severe the symptoms are, whether or not a person is trying to get pregnant, and how high their chances are of contracting heart disease or diabetes. Many patients will need to pursue more than one of these treatments in order to fully manage their symptoms:
- Healthy diet and exercise: A clean diet and regular exercise is recommended to all with PCOS, especially because weight gain often exacerbates this condition. This may also help normalize the menstrual cycle of overweight individuals as well as regulate blood glucose levels. In fact, just a 10% decrease in body weight can restore a regular period.2
- Birth control: Those who do not wish to become pregnant are often prescribed birth control, which often effectively helps clear acne, reduce male hormones, and normalize the menstrual cycle.2 There are multiple forms available to alleviate PCOS symptoms, such as the combination pill, progestin-only pill, skin patch, and vaginal ring.18
- Therapy: PCOS can affect a person’s body image and fertility to the point that it takes a toll on their mental health. Clinical behavioral and cognitive interventions can help a patient work through these changes in their life and develop healthy habits. Therapy for PCOS patients can center on goal-setting, adherence to diet and exercise regiment, self-love, and problem-solving.12
- Fertility medication: For people who wish to become pregnant, the lack of ovulation caused by PCOS can make becoming pregnant very difficult. Other factors influencing infertility (in either partner) should be ruled out before any of these treatments is administered. The following are several treatment options that may be considered:5
- Clomiphene – Stimulates ovulation; usually the first choice for patients.
- Clomiphene & Metformin – Respectively stimulates ovulation and helps control blood sugar levels for people with type 2 diabetes; this combination is tried if clomiphene alone fails.
- Gonadotropins – Stimulates ovulation (administered as shots); may increase risk of multiple births (twins or triplets).
- Diabetes medication: This method is especially helpful to overweight or obese PCOS patients. This medication regulates blood sugar levels the same way normal insulin levels would, in addition to lowering testosterone levels. The following treatment may be considered:1
- Metformin – Helps control blood sugar levels; may also aid in the slowing of unwanted hair growth and regulating ovulation.
- Anti-androgen medication: These medications reduce the number of androgens that individuals with PCOS produce. They are used to reduce unwanted hair growth on the face and body and clear up severe acne. The following are several treatments (including medications and alternative options) that may aid in the removal of acne or excess hair:
- Spironolactone (Aldactone) – Prescription pill originally used to treat high blood pressure, also shown to reduce the impact of male hormones in PCOS patients’ hair growth; should not be taken while pregnant or breastfeeding
- Finasteride (Propecia) – Prescription pill originally used by people with testes to treat hair loss, also shown to reduce the impact of male hormones in PCOS patients’ hair growth; should not be taken while pregnant or breastfeeding.
- Electrolysis (laser hair removal) – Laser treatment that removes unwanted hair growth on an individual’s body.
- Vaniqa – Prescription topical cream that temporarily removes facial hair chemically by interfering with the hair follicles on the treated area.19
- Surgery: A procedure known as “ovarian drilling” may increase the chance of ovulation. During this procedure, the doctor punctures the ovary with a small needle that conducts an electric current, in order to destroy a small part of the ovary. This can lower male hormone levels and regulate ovulation. However, this solution may only be effective for a few months.5
PCOS is a common condition in people with uteruses that manifests itself in many ways, so treatment must be established on an individual basis in order to address the patient’s specific needs. There are a vast number of resources available to those with PCOS, ensuring that the diagnosis does not interfere with the patient’s ability to live a long, happy, and risk-free life.

Concluding Remarks
Polycystic ovary syndrome, commonly referred to as PCOS, is the number one condition affecting fertility in people with uteruses. This condition causes the body to produce excess androgens, such as testosterone, which in turn causes a number of symptoms, including interruptions to the regular menstrual cycle, increased risks for certain cancers, increased risk of developing eating disorders, anxiety and depression, as well as a number of physical manifestations. The exact causes of PCOS are unknown, but research has found that insulin levels and genetics may play a key role. Luckily, there are a number of resources and treatments available for people with PCOS and its overall effect on a person’s life can be effectively managed with the correct treatment. While the health prospects for patients with PCOS are optimistic, dealing with this condition can be very difficult on both a physical and emotional level, so please communicate with family and friends for support, and consult with a medical professional if you are experiencing any of these symptoms or feel you may be at risk for PCOS.
For online support, visit the PCOS Awareness Association.
References
- “Adolescent Polycystic Ovary Syndrome According to the International Evidence-Based Guideline.” BMC Medicine. BioMed Central, 2020. Web.
- “Polycystic Ovary Syndrome (PCOS).” Mayo Clinic. Mayo Foundation for Medical Education and Research, 2016. Web.
- “Ovarian Cysts.” WomensHealth.gov. U.S. Department of Health and Human Services, 1 April 2019. Web.
- “Hyperandrogenic Anovulation (the polycystic ovary syndrome) – back to the ovary?” Human Reproduction Update. National Library of Medicine, 1998. Web
- “What is Polycystic Ovarian Syndrome?” PCOSupport. Polycystic Ovarian Syndrome Association, Inc., 2009. Web.
- “Inflammation.” ClevelandClinic.org. Cleveland Clinic, 28 July 2021. Web.
- “Polycystic ovary syndrome (pcos) fact sheet.” WomensHealth.gov. U.S. Department of Health and Human Services, 23 Dec 2014. Web.
- Escobar-Morreale, Hector. “Polycystic ovary syndrome: definition, aetiology, diagnosis and treatment.” Nature Reviews: Endocrinology. Vol. 14. Macmillan Publishers, 2018. Web.
- “What is Polycystic Ovarian Syndrome?” Health Line. Health Line Media, 2016. Web.
- “Abnormal Uterine Bleeding: A Guide for Patients.” ReproductiveFacts.org. American Society for Reproductive Medicine, 2012. Web.
- “PCOS Treatment for Pregnancy – Fertility Success Rates.” AdvancedFertility.com. Advanced Fertility Center of Chicago. Web.
- Teede, Helena J. et al. “Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome.” Human Reproduction. Vol. 33, No. 9. Oxford University Press, 19 July 2018. Web.
- “Helping Women Diagnose the Cause of Irregular Periods and Increase Chances of Pregnancy.” FertilitySA.com. Fertility Center of San Antonio. Web.
- “Anovulation.” ClevelandClinic.org. Cleveland Clinic, 25 August 2021. Web.
- Yildiz, Bulent O. “Diagnosis of hyperandrogenism: clinical criteria.” Best Practice and Research: Clinical Endocrinology and Metabolism. Vol. 20, Issue 2. Hacettepe University: Ankara, 2006. Web.
- “Full Cycle Hormone Profile.” ClinicalLabs.com.au. Australian Clinical Labs. Web.
- Sun, Tatym. “PCOS Diagnosis: The Role of Pelvic Ultrasound.” VolusonClub.net. Empowered Women’s Health, 5 February 2019. Web.
- Scaccia, Annamarya. “What’s the Best Birth Control for Women with PCOS?” HealthLine.com. HealthLine, 16 July 2020. Web.
- “Vaniqa.” Drugs.com. Drugs.com, 15 July 2021. Web.
Last Updated: 3 March 2022
