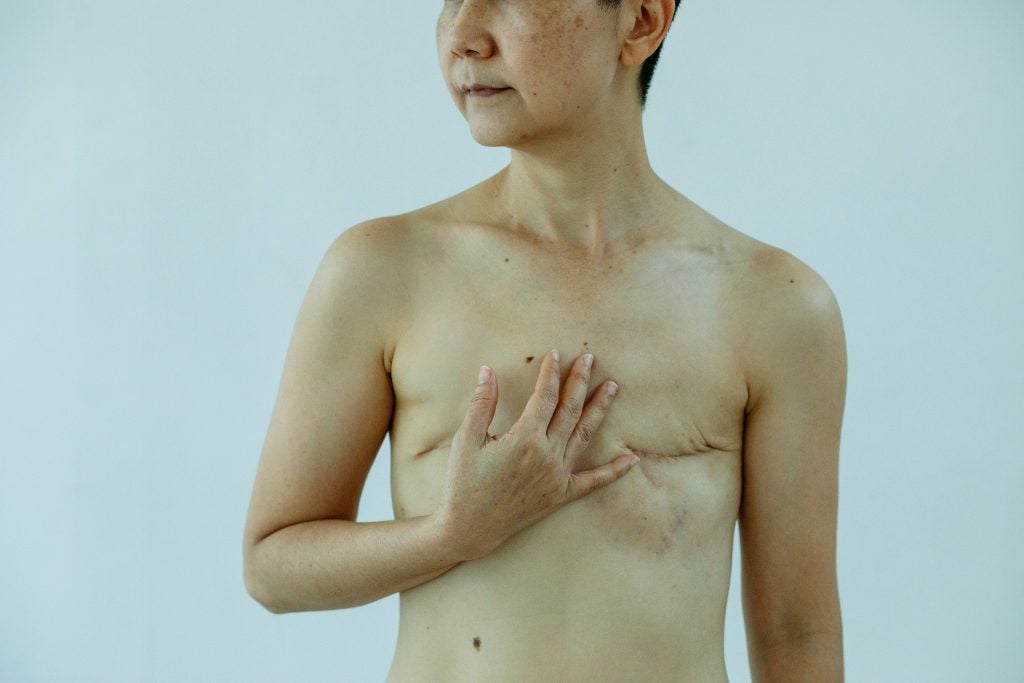
Mastectomy is the surgical removal of all or some of a patient’s breast tissue, usually performed in order to treat or prevent breast cancer. Mastectomy is not to be confused with lumpectomy, which is the removal of only the cancerous mass from the breast along with a minimal amount of surrounding healthy tissue.1 Mastectomy is most commonly performed on people with vulvas because there is a much higher incidence of breast cancer in people with vulvas than in people with penises2. However, when people with penises develop breast cancer, they can be treated with a mastectomy.3
Table of Contents
Types of Mastectomy Procedures
The details of mastectomy procedures vary between patients depending on the severity of their breast cancer, but there are five general types of mastectomy procedures.1
Simple Mastectomy:
Simple mastectomy, also called “total mastectomy,” involves the removal of the entire breast without the removal of the underlying lymph nodes or muscle. This procedure is usually recommended for patients who have multiple cancerous masses in the breast or patients who elect to have a prophylactic (preventative) mastectomy1 (for example, if they are genetically predisposed to get breast cancer).
Modified Radical Mastectomy:
The whole breast and the lower lymph nodes are removed, but none of the chest muscle is removed1. Patients with cancer that is at risk of spreading from the breast to other parts of the body are most likely to have this type of mastectomy. After the lymph nodes are removed, a doctor can examine them to determine if the cancer is likely to have spread to different parts of the body1.
Radical Mastectomy:
In a radical mastectomy, the whole breast is removed along with some of the underlying muscle and most of the lymph nodes in the chest.1 A surgeon will only recommend this procedure if the patient’s cancer has spread to the muscle tissue under the breast. Although this type of mastectomy was once quite common, the procedure occurs with decreased frequency since modified radical mastectomy can be just as effective when there is no cancer in the muscle1.
Partial Mastectomy:
A partial mastectomy is similar to a lumpectomy in that it is focused on removing just the cancerous part of the breast. In a partial mastectomy, slightly more healthy tissue is removed from the breast and the remainder of the breast tissue is left intact1.
Nipple Sparing Mastectomy (NSM):
In a nipple-sparing mastectomy, all the internal breast tissue is removed, but the areola, nipple, and breast skin are kept intact.4 Candidates for this type of procedure include people with a smaller concentrated area of cancerous tissue in the breast (not near the nipple/areola) that is surrounded by healthy tissue. If the surgeon finds cancerous tissue directly underneath or on the areola or nipple during the procedure, the nipple and areola will be removed. In the case where the skin is kept intact but the nipple is removed, the procedure can be called a skin-sparing mastectomy4. NSM is a newer procedure that some doctors are hesitant to perform out of concern that the cancer will come back; however, studies have shown that as long as the patient is a proper candidate, rates of recurrence are low5.
These five types of mastectomies can be performed on one or both of the breasts. When performed on both breasts, the procedure is referred to as a “double mastectomy.” Each procedure can be changed slightly by the surgeon to fit the needs of the patient’s specific case of cancer.
Choosing Mastectomy
A patient may choose to have a mastectomy for practical or personal reasons. If the cancer is too widespread for a lumpectomy, the patient will most likely need a mastectomy to remove the cancerous tissue.6 Some people also choose to undergo a mastectomy instead of a lumpectomy when they have breast cancer because they prefer the appearance of having no breasts or because they do not want to undergo radiation therapy at all or want a less extensive form of such therapy6
Some people choose to have a prophylactic, or preventative, mastectomy. A prophylactic mastectomy is performed on patients who either have not been diagnosed with breast cancer but want to take steps to lower their risk or people who have breast cancer and choose to remove an unaffected breast as well.7 The decision to have a preventative mastectomy can come from assessing a patient’s age, family breast cancer history, history of cancer in other parts of the body, and level of emotional attachment to the breasts. Because this is a serious procedure with possible side effects, one should only consider a preventative mastectomy if they have an extremely increased risk of breast cancer.7
If you are considering having a mastectomy procedure, be sure to thoroughly discuss your options with your doctor. Battling cancer can be an emotional journey, and some patients often feel hopeless or confused. It is important that you understand what is happening to your body so you can make decisions that are best for your life. Keep in mind that you have a right to assert your opinion about what your body goes through during cancer treatment6. Ask your doctor about the possible alternatives to mastectomy that may be right for you, such as lumpectomy or non-surgical treatments, and don’t be afraid to ask for a second opinion if you are unsatisfied. Friends, family, and sexual partners can be a great support system, but ultimately the decision of whether to have a mastectomy is a personal one.6
After you have made the choice to have a mastectomy, it is important to talk to your doctor about what to expect. Ask as many questions as you feel necessary, such as what the details of the procedure are, how you should prepare, what you should expect during recovery, what the emotional effects of this type of procedure are, and whether there is potential for complications. No question is a bad question, and chances are that the more information you have, the more at ease you will feel about having the procedure.
Cost
In the United States, mastectomy procedures are usually covered by health insurance.8 However, there may be certain criteria that need to be met. Some companies will only cover certain types of mastectomies. Prophylactic mastectomies and reconstructive surgeries are not always covered. Look at the details of your health insurance plan and talk to your doctor about any issue that may arise with the cost of the surgery. They may be able to make subtle changes that will be more affordable for you. Try not to let the cost of the surgery be the biggest factor in your decision to have the procedure. It is likely that if you discuss your financial concerns with your doctor, you may be able to find a treatment that is affordable and satisfies your needs and expectations. If you are comfortable reaching out to loved ones or friends for financial support, this may be another way to make a mastectomy more affordable for you.
Mastectomy Procedure Details
Mastectomy procedures are performed while the patient is under general anesthesia. The average mastectomy takes about two to three hours to complete, but the procedure may last longer if the patient chooses to have breast reconstruction done at the same time9. The type of incision made on the breast is dependent on the type of mastectomy and the patient’s desired aesthetic outcome of the surgery. Sometimes, after surgery, fluid can collect in the spaces of the breast where tissue was removed. For this reason, drainage tubes are often inserted during surgery to collect this fluid and can be taken out by the surgeon at a later date9. When the procedure is complete the surgeon wraps the breast area in several bandages that are to be left on during the recovery period.

Recovery
After surgery, a mastectomy patient usually stays in the hospital for one to two nights9. This stay may be longer if reconstructive surgery was involved. Pain medication is prescribed to make the patient more comfortable during recovery. During the stay at the hospital, patients are given instructions on how to care for bandages, stitches, and drainage tubes9. Patients are also taught how to do daily exercises that help to prevent stiffness of the arm or chest and the development of severe scar tissue.9 A doctor will most likely schedule an appointment for a recovery check-up about one to two weeks after the procedure, where the doctor will make sure the patient is healing well and possibly remove drainage tubes, staples, and bandages.9
After being released from the hospital, there are still several precautions a mastectomy patient should take to ensure a healthy recovery from the procedure. Certain exercises and strenuous activities should be avoided for several weeks after the procedure, as should wearing a bra or tight clothing until permitted by a doctor. Plenty of rest is required for proper recovery.9 Patients are advised to seek assistance from family and friends to ease the stress of daily activity as they recover. The recovery instructions from a doctor should be followed very carefully to reduce the risk of infection or other complications.9
Risks and Complications
As with any other surgery, there is a risk of complications such as infection and scarring1. A trained surgeon will take the necessary precautions to avoid these side effects, but if they occur, they can often be effectively treated if caught early enough. A seroma (buildup of clear fluid) or hematoma (buildup of blood) could develop at the surgery site but can most likely be resolved by medical intervention1. Extreme sensitivity or numbness of the affected breast can occur as a result of nerve damage inflicted during the surgery1. Any uncomfortable or worrisome symptoms should be reported to a doctor as soon as possible so that dangerous complications such as infection can be tended to in a timely manner.
After Mastectomy

A mastectomy procedure is not always the end of a patient’s battle with breast cancer. The first thing to consider is whether the patient needs further cancer treatment such as radiation or chemotherapy. This may be necessary if the mastectomy was not able to remove all the cancerous tissue, which could be the case if the breast tumor was very large, if the cancer was in several parts of the breast, or if the patient’s cancer had spread to the lymph nodes and other parts of the body. It may also be necessary to consider the physical and emotional effects of a mastectomy that could interfere with a patient’s return to daily life.
Physical Effects
The removal of breast tissue and sometimes muscle tissue can leave a patient with physical differences in their bodies that may affect the way they live their lives, the clothes they wear, and how they view themselves. There are several options for adjusting physically after a mastectomy to make the patient feel as comfortable and confident as possible.
Breast Reconstruction
The first option for physical modification after mastectomy is breast reconstruction. Breast reconstruction is a surgical procedure meant to match the cancer-affected breast to the size and shape of the other breast after a mastectomy10. The nipple and areola can also be reconstructed to match the healthy breast. Breast reconstruction can also involve reshaping both breasts to look a certain way, even if one of them was not affected by cancer. Most often the breast or breasts are reconstructed using silicone implants or fatty tissues from other parts of the patient’s body.10 Patients often have the choice to have breast reconstruction surgery immediately following a mastectomy, but some decide to have the reconstructive surgery several months or years later.
The advantage of having breast reconstruction immediately following a mastectomy is that the mastectomy and the first stage of the reconstructive surgery can often be done at the same time10. This allows the patient to reduce the number of surgeries they must undergo. The patient can also avoid the potential emotional effects of experiencing the loss of one or both breasts by having the procedures done simultaneously. The disadvantages of having reconstruction done immediately following a mastectomy are that the recovery period is often longer and if the patient requires further radiation treatment, there is a possibility of damage to the reconstructed breast. In fact, many doctors do not recommend immediate reconstruction for patients that require radiation therapy.10
Many patients decide to wait to have reconstructive surgery because they do not want to subject their bodies to more surgery at one time than necessary. Patients may also choose to wait because planning a reconstruction is too much to think about while dealing with the other important decisions surrounding their cancer treatment.10
The decision to have reconstructive surgery is usually dependent on whether a patient is healthy enough to undergo the extra procedure, the cost and insurance coverage, and the desire to have one or both breasts reconstructed11. Some doctors prefer that a patient decide if they may want to do reconstructive surgery, even if they plan to delay the procedure, before they make plans for a mastectomy. This way, every option can be planned out beforehand, and fully informed decisions about procedure details can be made according to what is best for the patient’s desired outcome. The decision to have reconstruction should not come directly from the opinions of other people. Friends, family, and sexual partners can be amazing forms of support, but they should not increase the pressure for the patient to do something that they would not otherwise want to do.
As with all cosmetic surgery, it is important to have realistic expectations for the outcome. If you are considering reconstructive surgery, be sure to communicate effectively with your doctor and make sure that they are understanding of your goals. Keep in mind that after reconstruction, although the breasts may look the same as before, the reconstructed breast(s) may feel different to the touch or have less sensitivity than they did before the mastectomy.11
Prosthetic Breasts
Although breast reconstruction is right for some patients, there are alternatives for those who do not want to undergo surgery but would still like the appearance of having breasts. Prosthetic breasts are one of these options. Prostheses can be worn in bras or swimsuits and come in several sizes and shapes according to the patient’s preferences. Some prostheses can even adhere to the chest so that they may be worn without a bra under clothing or during sex12. A prosthesis can be made in materials that are suitable for wearing in chlorinated pools or salt water. High-quality prostheses are usually priced between $100 and $500 USD12. Some people may be able to get a prescription from their doctor and have the cost of the prosthesis covered by insurance.12
Wearing Your Scars

Some mastectomy patients decide not to have reconstructive surgery or use prosthetic breasts at all. Many people express that their mastectomy scars and physical differences after surgery make them feel proud and empowered because they represent perseverance through a tough time in their lives. There is no functional reason to recreate the appearance of breasts after a mastectomy, so the decision to do so is purely based on the individual preferences of the patient who has undergone the mastectomy.
Emotional Effects of Mastectomy
Mastectomy and its aftermath can have a large effect on the mental and emotional wellbeing of the patients who undergo this procedure. Some people experience grief about the loss of one or both of their breasts or about the entire breast cancer experience.13 Mastectomy may lead to issues with body image and overall confidence. Sometimes the results of the surgery can have negative effects on a person’s sex life if they are experiencing a loss of self-esteem. The loss of sensation in the breasts can also make arousal more difficult to achieve for some people13. Many female-identifying or feminine-presenting people feel less feminine than before their mastectomy. It can even be harder to connect with sexual partners in the same way emotionally because of these sexual difficulties.
Breasts (or the lack thereof) do not determine femininity. Female-identifying people who have had their breasts removed are in no way less feminine than they were before the procedure. Similarly, male-identifying or masculine-presenting people should not feel that their experience with breast cancer and mastectomy has a negative effect on their masculinity. Femininity and masculinity are the products of personal expression and cannot be determined solely by physical features. The decision to go through with a mastectomy procedure is one that requires a great deal of strength. Having a mastectomy is something that should make those that must undergo the procedure proud, as the procedure is a symbol of perseverance after a traumatic breast cancer diagnosis. For some patients, it may take time to restore self-esteem and reestablish their sexuality. The right partner will understand this and be able to show love and respect regardless. Couples who have been affected by mastectomy can restore and improve their sexual and emotional connection by implementing effective communication and general positivity.
If you or someone you know is suffering emotionally from the effects of a mastectomy procedure, it may help to know that there are other people who are most likely experiencing the same difficulties, and there are plenty of resources to help you. Sometimes a patient’s best support system can come from close friends and family. Ask your doctor about groups that are designed to help recovering mastectomy patients cope with their emotional burdens and provide them with useful answers to questions and concerns. There are often programs led by cancer survivors who can provide guidance to patients throughout their diagnoses, treatments, and recoveries. The American Cancer Society (ACS) offers programs like this. More information about the resources provided by ACS can be found here. Many mastectomy patients feel helpless or scared. Know that this is a normal reaction to a traumatic experience and that there is help and hope for those who seek it.
Concluding Remarks
Mastectomy is a surgery that involves much more than just the procedure itself. There are many important decisions to be made before and after surgery that can have a significant effect on a person’s life. Those considering having a mastectomy are encouraged to look to trusted family, friends, or partners for much-needed support. Keep in mind that the effects of mastectomy do not have to be negative. There are many options for adjusting physically and emotionally to life after the procedure. With positivity, perseverance, and support, patients can ultimately recover from their mastectomy with feelings of pride and strength.
References
- The American Cancer Society medical and editorial content team. “Mastectomy.” American Cancer Society. Cancer.org: October 27, 2021.
- The American Cancer Society medical and editorial content team. “Key Statistics for Breast Cancer in Men.” American Cancer Society. Cancer.org: January 12, 2022.
- The American Cancer Society medical and editorial content team. “Surgery for Breast Cancer in Men.” American Cancer Society. Cancer.org: April 27, 2018.
- “Nipple-Sparing Mastectomy.” Breastcancer.org. Breastcancer.org: February 2, 2018.
- “In Appropriate Women, Nipple-Sparing Mastectomy Doesn’t Lead to Higher Breast Cancer Recurrence Rates.” Breastcancer.org. Breastcancer.org: September 4, 2019.
- “Mastectomy vs. Lumpectomy.” Breastcancer.org. Breastcancer.org: March 9, 2019.
- The American Cancer Society medical and editorial content team. “Preventive Surgery to Reduce Breast Cancer Risk.” American Cancer Society. Cancer.org: December 16, 2021.
- The American Cancer Society medical and editorial content team. “Women’s Health and Cancer Rights Act.” American Cancer Society. Cancer.org: May 13, 2019.
- “Mastectomy: What to Expect.” Breastcancer.org. Breastcancer.org: November 4, 2021.
- The American Cancer Society medical and editorial content team. “Breast Reconstruction Options.” American Cancer Society. Cancer.org: October 20, 2021.
- “Breast Reconstruction After Mastectomy.” National Cancer Institute. Cancer.gov: February 24, 2017.
- “Prosthetics: An Alternative to Reconstruction.” Breastcancer.org. Breastcancer.org: March 7, 2019.
- Tarkowska, Magdalena et al. “Sexual functioning and self-esteem in women after mastectomy – a single-centre, non-randomised, cross-sectional study” Contemporary Oncology. 24 (2), 106–111. National Center for Biotechnology Informnation: June 18, 2020.
Last Updated: 3 March 2022
