
The breast is a secondary sex organ located on top of the pectoral muscle of the torso. The breasts, also called mammaries, produce milk (lactate) so that a mother can feed her infant child. Each breast is composed of both fatty tissue and mammary glands. Mammary glands are connected to the nipple via milk ducts, tubes that carry breast milk from the lobules to the nipple. Both biological males and females can be diagnosed with breast cancer, and every year roughly 252,710 females in the United States are diagnosed with invasive breast cancer. Breast cancer takes the life of 40,610 American females each year.1 Cancer is defined as the uncontrolled growth of abnormal cells in the body.2 Breast cancer is a form of cancer that commonly originates in the inner lining of the milk ducts or the lobes in the mammary gland that produce milk. During the later stages, breast cancer may also spread to the lymph nodes (bean shaped masses that filter the blood) in the neck and armpit. Currently, about 1 in 8 U.S females, and 1 in 1000 males in the U.S. will develop breast cancer over the course of their lifetime.3 Despite the high rate of diagnosis, 93% of those who are diagnosed with stage 0 cancer, also referred to as carcinoma in situ survive for five or more years.4 Stage 0 breast cancer often does not require treatment, and when Stage 0 does require treatment that treatment is usually successful.4
Table of Contents
Types of Breast Lumps
Four types of breast lumps exist: cysts, fibroadenomas, pseudolumps, and malignant tumors. Cysts are harmless fluid filled sacs of tissue, that can grow within the breast.5 Cysts are typically indicated by a tender, round, moveable lump.5 Like cysts, breast fibroadenomas are also benign, and they are composed of fibrous and glandular tissues.5 Pseudolumps are benign as well and may be composed of scar tissue, hardened silicone from breast implants, or dead fat cells.6 Malignant tumors, unlike the other types of breast lumps, are cancerous and not benign. A malignant tumor is an irregularly shaped hard mass of cells that accounts for roughly 20% of all breast lumps.7
Stages of Breast Cancer
There are four stages of breast cancer. The stages of the cancer is determined based on its size and location. Each stage has a different survival rate. The following are the stages of breast cancer:
- Stage 0: The breast cancer is non-invasive and the abnormal cells are confined to the breast duct or lobules. This stage of breast cancer is sometimes referred to as ductal carcinoma in situ (DCIS), or lobular carcinoma in situ (LCIS).8
- Stage I: This stage of breast cancer is defined by the tumor being 2 cm or smaller, and having not spread outside the breast.8 The small cancer cell clusters are typically found in the lymph nodes.8
- Stage IIA: Stage IIA breast cancer can take two forms. Either a tumor larger than 2 cm has grown in 1 to 3 lymph nodes and the tumor in the breast is absent or smaller than 2 cm, or the tumor is 2 to 5 cm and has yet to spread to the lymph nodes from the breast.9
- Stage IIB: Stage IIB cancer means that either the tumor is between 2 to 5 cm with additional small clusters of cells up to 2 mm being found in the lymph nodes, the cancer is between 2 to 5 cm and has spread to 1 to 3 lymph nodes, or the cancer is larger than 5 cm and has yet to spread to any lymph nodes.9
- Stage IIIA: At this stage, the breast tumor may absent or of any size. Tumors are also found either in 4 to 9 lymph nodes or are larger than 5 cm and found in small clusters of the axillary lymph nodes or lymph nodes near the breastbone.10
- Stage IIIB: The tumor in the breast at this stage can be of be any size, and the cancer has spread to the chest wall or skin. At this stage there may be some skin ulceration, the cancer might have spread to up to 9 axillary lymph nodes or to the lymph nodes near the breastbone.10
- Stage IIIC: At this stage, there is either no tumor in the breast or the tumor may be any size, having spread to the chest wall or skin, much like in Stage IIIB. However, in stage IIIC the cancer may have spread to 10 or more axillary lymph nodes or to the nodes near the breastbone or collarbone.10
- Stage IV: In this stage of breast cancer the cancer has spread to other organs throughout the body, most often including the lungs, liver, or brain, but also including the bones and other organs.11
Both stage 0 and stage I’s survival rates are now near 100%, and stage II’s survival rates are around 93%.12 The five-year survival rate for stage III breast cancer’s is 72%, but many people with stage III breast cancer are successfully treated.12 Stage IV’s five-year survival rate is 22%, though there are many treatments that are available.12 As the numbers show, early detection is one of the best ways to help ensure the safety and survivability of a patient with breast cancer. Knowing the risk factors associated with breast cancer also helps ensure early detection and increases survival rates.
Risk Factors Associated with Breast Cancer

Breast cancer forms when breast cancer forms when a healthy cell experiences a mutation in its DNA. In many cases, these mutations are harmless or lead to death of the cell. In other cases, the mutation causes the cell to reproduce rapidly, consuming many resources. If the body’s immune system is unable to eliminate the cell, it will continue to divide, which creates a mass of cells called a tumor. A tumor can be benign (harmless) or malignant (cancerous).13 The following are risk factors that can affect the probability of being diagnosed with breast cancer:
- Biological Sex: Above all, being a female is the primary risk factor for breast cancer. Males can develop breast cancer, although it is over 100 times more common in females than males. This lowered risk for male breast cancer is due to lower levels of circulating estrogen in the body.15
- Genetic Factors: BRCA1, and BRCA2 are tumor receptor genes that work to prevent cancerous tumors from forming.13 In certain families, these tumor receptor genes may be mutated, resulting in an 80% chance of developing a cancerous tumor. Roughly 5 to 10% of all breast cancers can be traced to genetic factors.13
- Heredity: Having a parent, child, sibling, or other relative who has been diagnosed with breast cancer before the age of fifty increases the odds of also being diagnosed with breast cancer.13
- Race and Ethnicity: Breast cancer is more common in white and African females than females of other ethnicities.1
- Early Menstrual Periods: Females who begin menstruating before the age of 12 are at a slightly increased risk for breast cancer. This risk may be due to higher overall exposure to the sex hormones estrogen and progesterone.14
- Late Menopause: Females who undergo menopause after the age of 55 are at a slightly increased risk. This risk is due to the increased exposure to the hormones estrogen and progesterone.14
- Childbirth: Having children leads to a reduction in the amount of estrogen and other hormones in a female’s body, which also leads to a reduction in the risk of breast cancer.17 However, there is also a slight short-term increase in risk in the for females who have recently experienced childbirth.17 While the reason for this brief increase is unknown, it is believed to be due to either the increase in hormones or the growth of breast tissue that are experienced during pregnancy.17
- Synthetic Hormones: It is possible that use of birth control pills, or hormone therapies (i.e. post-menopausal hormone therapy and hormone replacement therapy) can lead to an increased risk.16
- Lifestyle Choices: Other risk factors include not breast-feeding after having a baby, daily alcohol consumption, obesity, and lack of exercise.16 All of these factors lead to an increase in hormones like estrogen in the body, and with estrogen’s link to breast cancer these lifestyle choices become risk factors.
These are all factors that lead to an increase in the risk of an individual developing breast cancer. However, possessing any of these traits does not guarantee that one will get breast cancer. In the same way, one can develop breast cancer in spite of not having any of the above risk factors. When it comes to reducing your risk of breast cancer living a healthy lifestyle is the best method.
Symptoms of Breast Cancer
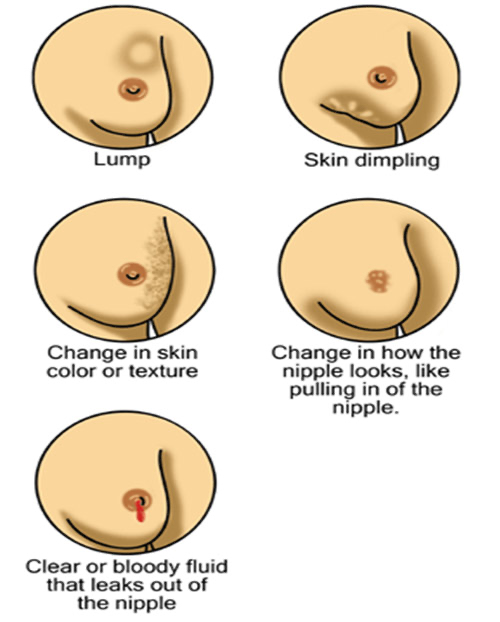
The early stages of breast cancer can be asymptomatic meaning they are not accompanied by any noticeable symptoms.18 As such, routine breast examinations are extremely important even when no symptoms are present. However, a person with early stage breast cancer can exhibit symptoms. These symptoms may include an irregularly shaped lump in the breast or armpit, changes in the shape, feel, or size of the breast or nipple, skin dimpling or tethering, changes in skin color or alterations in the appearance of the nipple, or a bloody fluid coming from the nipple.18 More serious symptoms of breast cancer include increasing tenderness of the breast and eventual bone pain, skin ulcers, swelling of the armpit, weight loss, inflammation of the surrounding tissues, and insomnia.19
Screening for Breast Cancer
Physical examinations are highly recommended as a measure of early identification of breast cancer. Physical examinations include clinical breast examinations, which are performed by a medical professional, and self-examinations, conducted regularly by the individual. The American Cancer Society references three methods of imaging testing to identify if an individual has breast cancer: mammograms, breast ultrasounds, and breast MRI scans.20 Early detection of breast cancer is the most effective way to improve chances of survival. By identifying the cancer in the earlier stages, it is often possible to begin treatment before the cancer progresses to the later stages that are more frequently fatal.
Females aged 40 to 49 should open a dialogue with their doctors about when to begin getting mammograms and other breast cancer screenings, being sure to discuss their medical history and any risk factors that might be present.23
Breast self-exams
Breast self-exams (BSEs) are a simple and relatively effective way to screen for changes in breast tissue at home without a medical professional. Females should conduct a BSE once a month, approximately three to five days after menstruation. Males should also schedule a day once a moth to conduct a BSE. This is important because breasts may change slightly over the course of the month, and examining the breasts at the same time each month helps reduce these differences.21
To conduct the exam, visually inspect the breasts in front of a mirror with arms at your sides (1 on the diagram), above your head (2), and on your waist (3) for any noticeable changes in appearance or coloration.21 For most people, breasts are not identical, so do not be alarmed if they are not exactly the same size or shape. Raise one arm and inspect the upper areas of the breast and the armpit for any lumps (4), rashing, or dimpling. Do the same for each breast.21 Then, lay down on your back with your right hand above your head (6). Using the middle fingers of your left hand, move in small coin-sized circles over the right breast. Repeat this procedure using the right hand for the left breast. Visually check your nipples for any discharge (5).21 Continue to examine the entire breast using a spiral pattern that extends from the collarbone to the bra line, and from the armpit to the breastbone.21
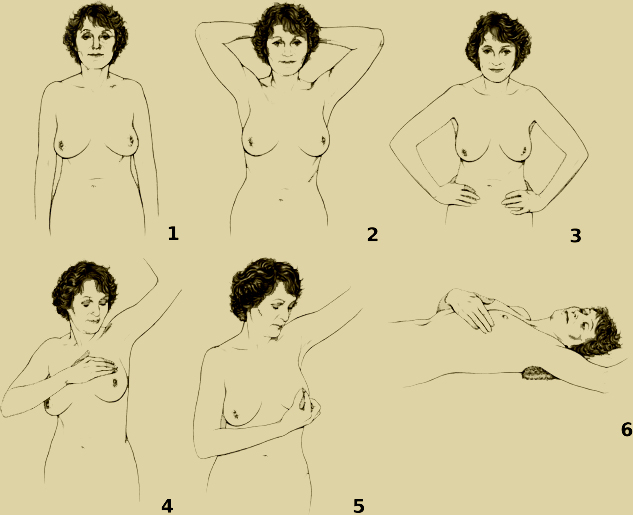
By the end of a BSE, you should know how your breasts look and feel normally, and any significant or unusual changes should be promptly reported to a doctor for further examination. Breast self-examinations are recommended for people of any age or biological sex and can be an important part of early detection for males and females.
Clinical Breast Examination
Clinical breast examinations (CBEs) are similar to self-examinations, but performed by a medical professional and are often given in conjunction with periodic mammograms. Combining the two result in the most effective screening method for breast cancer. During a clinical breast exam, a health professional will ask the patient questions about any current problems they may be experiencing, as well as questions about medical history and any potential risk factors. The examiner will then ask the patient to remove their clothes from the waist up and lie on the examination table.22 An examiner will inspect each breast, underarm, and collarbone for changes or abnormalities in size or skin, and for signs of injury or infection like bruising or redness, as well as lumps in the breast or discharge from the nipples. After this visual inspection, the doctor or nurse will feel each breast for any painful areas, starting from a region one inch below the breast up to the collarbone. They will also check the armpit (axillary area) and around the neck (lymph nodes).22 Following this examination, the doctor may instruct the patient on how to examine themselves using the breast self-exam method.
Mammograms
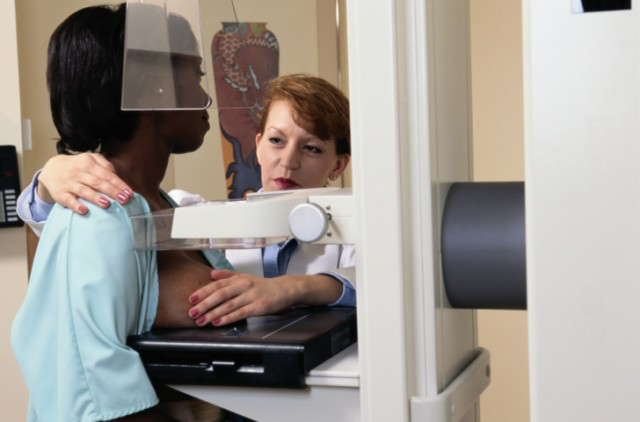
Mammography is the most effective method of screening for breast cancer.23 This technique involves taking an X-ray picture of the breast in order to detect the presence of dense lumps of tissue.24 During the procedure, a radiology technologist will place the individual’s breasts, one at a time, onto a plate that contains an X-ray film while another plate will push the breast down against the film to secure the breast and obtain a clear image.24 It is important to have both breasts checked as even individuals who have had breast cancer in one breast are still at risk for breast cancer in the other breast.24 Annual mammograms should be routine for females over the age of 45, and at the age of 55 the choice to schedule mammograms every other year can be made.25 For females under the age of 45 may be have a mammogram or other screening if there is suspicion of a tumor do to an abnormal CBE or if there is a family history that indicates that they are at a very high risk for breast cancer.25
Breast Ultrasounds
Breast ultrasounds are a noninvasive screening procedure that use sound waves to produce images of the breast.26 Breast ultrasounds can have various applications. For example, they can be used to further examine abnormalities that were found during a mammogram. They may also be used to investigate any abnormalities that were felt in a CBE or BSE, but were not found with the mammogram. Breast ultrasounds can also help with the accuracy of a biopsy.26 Biopsies involve the removal and analysis of small pieces of tissue to search for cancer or other diseases.26 Breast ultrasounds also help in get clearer images of denser breast tissue, which might cause the X-rays of mammograms to be difficult to read. In addition, breast ultrasounds can easily and painlessly identify the difference between solid masses and less harmful, noncancerous cysts.26 Breast ultrasounds are painless, noninvasive, and widely available.
Breast MRI
Breast MRIs generate detailed images of breasts through the use of magnets and radiowaves. Females should undergo a breast MRI if they are at high risk for breast cancer23 or if they have been previously diagnosed with breast cancer in order to check for developing tumors in both breasts.27 Breast MRI scans are typically used in coordination with mammograms, rather than used independently, as the breast MRI does not always identify some cancers more easily identified by a mammogram.27 Breast MRIs are used more frequently once cancer has been confirmed to get better images of the developing tumors, and not during the initial diagnosis, as the more precise nature of the MRI can lead to false positives, which can lead to unnecessary biopsies and stress for the individuals.27
Diagnosing Breast Cancer
If the screening tests have revealed a breast lump or other abnormality, the next step is often a biopsy. During a biopsy, in order to determine whether or not an abnormality is cancerous, a sample of the irregular tissue is removed and inspected using a number of tests to determine if the tissue is cancerous.20
In a needle aspiration biopsy, the doctor uses a hollow needle attached to a syringe to withdraw (or aspirate) a small piece of the tissue. Once the needle is in place, fluid or tissue is drawn out.22 Clear fluid indicates a benign cyst, while cloudy or bloody fluid indicates the possibility of cancer. When solid tissue fragments or a bloody fluid are withdrawn, they are inspected under a microscope to determine the type of lump or cyst and its severity.28
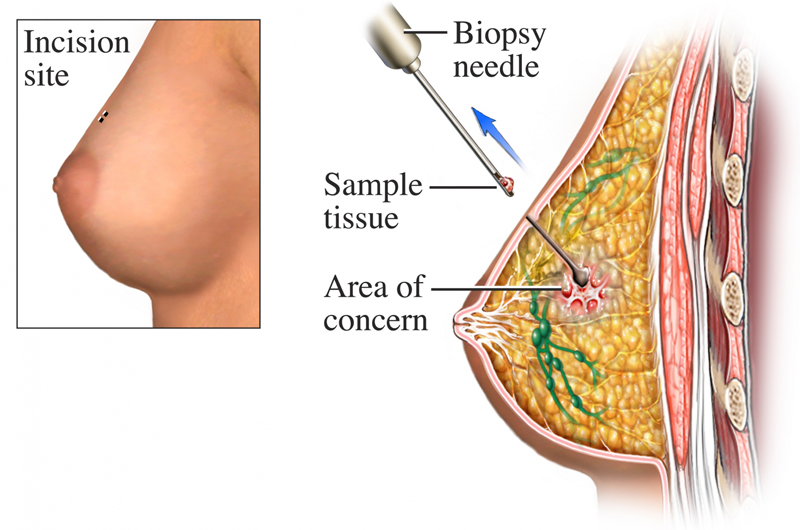
Usually, breast cancer is diagnosed using the needle aspiration biopsy technique. Occasionally, however, surgery is required to remove all or part of the lump for inspection because a needle aspiration biopsy is inconclusive. This is process is referred to as a surgical or “open” biopsy.29 There are two kinds of open biopsy. In an excisional biopsy the surgeon removes the entire cancerous mass as well as the normal-appearing perimeter of breast tissue.29 If the mass is too large to be removed easily, only part of it may be excavated in what is referred to as an incisional biopsy.29 Both kinds of surgical biopsies are more invasive than needle aspiration biopsies and often lead to stitches, scarring, and a change in shape of the breast.
Treatment
Breast cancer can be treated in several different ways. A doctor will recommend a treatment or treatments based upon the kind of breast cancer and the amount it has spread. There are several options for treatment of breast cancer, both nonsurgical and surgical.30 Doctors will discuss options with patients, including the draw backs and benefits to utilizing the different types of treatments, and what will be most effective for an individual’s cancer.
Nonsurgical Treatments
There are four types of nonsurgical treatments that can be used against breast cancer. These treatments utilize chemicals in an attempt to fight off the cancer without needing to performing surgery or remove the cancer and surrounding tissue. The following are nonsurgical treatment options:
- Hormonal therapy alters the levels of estrogen in the patient’s body. Lowering the levels of estrogen prevents cancer cells from getting the hormone levels they need to grow, thereby killing the cancerous cells or slowing their growth.30
- Immunotherapy works with the body’s immune system to fight cancer or control the side effects caused by other types of treatment.30
- Chemotherapy implements drugs or medicines that can shrink or kill the cancerous cells or alleviate symptoms caused by other cancer treatments. Chemotherapy has some side effects, including sores in the mouth, nausea, hair loss, and fatigue. These side effects tend to end after treatment.30
- Radiation therapy uses high-energy rays to kill cancer cells, but there is a lifetime limit to the amount of radiation your body can handle, and a common side effect of radiation therapy is fatigue.30
While these nonsurgical treatments aim to reduce the need for surgery they can also be used in coordination with surgical treatments to better treat patients and improve survival rates.
Surgical Treatments
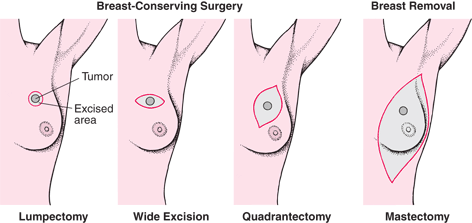
There two types of surgical options for treating breast cancer at different stages. In some circumstances a patient’s doctor may recommend a lumpectomy also known as a wide excision surgery.31 These surgeries leave most of the breast tissue intact while removing the cancerous tumor along with some of the healthy breast tissue in the surrounding area.31 If the cancer is not a good candidate for those procedures a doctor may recommend a mastectomy.31 There are five types of mastectomy which is the surgical removal of the breast and some of the surrounding tissue.32 The following are surgical options can be utilized either on their own or coupled with nonsurgical treatments:
- In a simple mastectomy, the entirety of the breast (including the nipple) is removed, but the surgeon leaves the lymph nodes and underlying muscles untouched.32
- In a modified radical mastectomy, the breast is completely removed, including the nipple and some lymph nodes while leaving the muscle and remaining lymph nodes intact.32
- A radical mastectomy, like the modified radical mastectomy removes the breast completely, along with the nipple; however, unlike the modified version, the radical mastectomy removes the lymph nodes completely, along with some of the underlying chest muscle.32
- A partial mastectomy, also known as a quadrantectomy, is used for less severe forms of stage I or II breast cancer, and only removes the cancerous cell and the bordering tissue around it.32
- In a nipple-sparing mastectomy all of the breast tissue is removed, but the nipple is, as the name suggests, spared. This means that while the breast tissue underneath the skin is removed, the skin of the breast is left intact, allowing for implants or transplants of tissue from elsewhere in the body to be used to replace the lost breast tissue.32
Both mastectomies and lumpectomies are often followed by radiation and chemotherapy to ensure the cancer has been completely removed and will not return.30
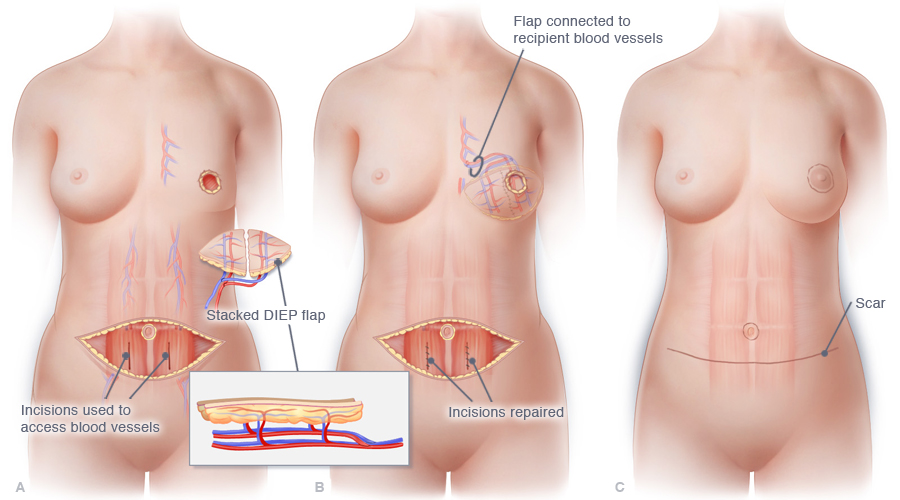
Modern breast reconstruction techniques enable physicians to rebuild the breast mound using skin grafts and fat from the abdomen. The nipple can also be replaced, usually by the skin of the reconstructed breast, and even connected to recipient blood vessels to create a symmetrical and realistic breast for.33 There are two main options for reconstruction: implant reconstruction or autologous reconstruction.34 With implant reconstruction, a patient receives implants filled with saline, silicone gel, or a combination of the two.35 Autologous flap reconstruction or “flap” reconstruction uses tissue, either fat, skin, or even sometimes muscle from another part of the body to replace the lost breast tissue.36 Nipple reconstruction surgery can also be done.37 Nipples can either be rebuilt from tissue from other parts of the body, like with the flap reconstruction surgery, or tattooed on.37 The appearance of the tattooed nipples can be personalized and chosen by the patient.37
Breast Cancer and Sex

Breast cancer and its treatment may or may not affect a person’s sexuality and sexual desire in a number of different ways. Symptoms can be both physical and mental and emotional, so there are many ways that one’s sexuality can be affected. Some females who opt for breast-conserving surgeries, such as lumpectomies, are less likely than mastectomy patients to report enduring post-cancer sexual difficulties, due to the preservation of the majority of breast tissue in those surgeries.33 Feelings of grief and fear triggered by the cancer diagnosis may temporarily reduce sexual drive while the side effects of the cancer treatment may be debilitating and painful, which can impair libido.38 Some treatments may impair libido or decrease physiological arousal due to the hormonal changes in the body.38 People who have experienced breast cancer (especially in the case of mastectomy recipients) may fear that they are no longer attractive to their partner.38
Those diagnosed with breast cancer are encouraged to discuss their feelings and concerns with both their doctors and their partners to help resolve or soothe them. Practicing healthy communication with loved ones can relieve stress and encourage a positive environment. Currently, the American Cancer Society offers counseling to females who have undergone a mastectomy to help them cope with the change. It is important to remember one does not need breasts to be beautiful, feminine, and to live a full and happy life. Most people who have had a mastectomy report no change in the key aspects of their sexuality (like frequency of sex or overall satisfaction).38
Concluding Remarks
Getting cancer will always be life-changing, but with modern medicine and early detection one can still thrive and live a full life. Today, there are survivors everywhere and there are support networks not just for cancer patients, but also for caretakers, family members, and survivors. Be sure to take advantage of the resources available before, during and after diagnosis. Know your own body and pay attention to changes, as early detection is still the best was to ensure survival. When in doubt, contact your physician.

References
- “How Common Is Breast Cancer?” American Cancer Society. American Cancer Society, 5 Jan. 2017. Web. 15 Apr. 2017.
- “Cancer.” Merriam-Webster. Merriam-Webster, n.d. Web. 15 Apr. 2017.
- “U.S. Breast Cancer Statistics.” Breastcancer.org. Breastcancer.org, 10 Mar. 2017. Web. 15 Apr. 2017.
- “Stage 0 Breast Cancer: Information & Options.” CancerCenter.com. Cancer Treatment Centers of America, Inc., n.d. Web. 15 Apr. 2017.
- “Fibrosis and Simple Cysts in the Breast.” American Cancer Society. American Cancer Society, 21 Apr. 2016. Web. 15 Apr. 2017.
- Stephan, Pam. “What Are the Causes of Benign Pseudolumps?” Verywell. About, Inc., 09 Aug. 2016. Web. 15 Apr. 2017.
- “Different Kinds of Breast Lumps.” Cancer Center. Stony Brook University Cancer Center, 20 May 2015. Web. 15 Apr. 2017.
- “Stages 0 & 1: The National Breast Cancer Foundation.” National Breast Cancer Foundation, n.d. Web. 26 May 2017.
- “Stages 2: The National Breast Cancer Foundation.” National Breast Cancer Foundation, n.d. Web. 26 May 2017.
- “Stages 3: The National Breast Cancer Foundation.” National Breast Cancer Foundation, n.d. Web. 26 May 2017.
- “Stages 4: The National Breast Cancer Foundation.” National Breast Cancer Foundation, n.d. Web. 26 May 2017.
- “Breast Cancer Survival Rates & Statistics.” American Cancer Society. American Cancer Society, 18 Aug. 2017. Web. 26 May 2017.
- “Breast Cancer Risk Factors: Genetics.” Breastcancer.org. Breastcancer.org, n.d. Web. 15 Apr. 2017.
- “Menstrual History.” Breastcancer.org. Breastcancer.org, n.d. Web. 15 Apr. 2017.
- “What Are the Key Statistics About Breast Cancer in Men?” American Cancer Society. American Cancer Society, 05 Jan. 2017. Web. 16 Apr. 2017.
- “Lifestyle-related Breast Cancer Risk Factors.” American Cancer Society. American Cancer Society, 18 Aug. 2016. Web. 16 Apr. 2017.
- “Reproductive History and Cancer Risk.” National Cancer Institute. National Cancer Institute, 9 Nov. 2016. Web. 19 May 2017.
- Chalasani, Pavani. “Breast Cancer.” Medscape. WebMD Health Professional Network, 13 Apr. 2017. Web. 16 Apr. 2017.
- Story, Colleen M. “The Symptoms of Stage 4 Breast Cancer.” Healthline. Healthline Media, 30 Aug. 2016. Web. 16 Apr. 2017.
- “How Is Breast Cancer Detected? | Breast Cancer Diagnosis.” American Cancer Society. American Cancer Society, n.d. Web. 16 Apr. 2017.
- “Breast Self-exam.” MedlinePlus Medical Encyclopedia. A.D.A.M., Inc., n.d. Web. 17 Apr. 2017.
- “Clinical Breast Exam: The National Breast Cancer Foundation.” National Breast Cancer Foundation. National Cancer Institute, n.d. Web. 17 Apr. 2017.
- ” What Is Breast Cancer Screening?” Centers for Disease Control and Prevention. Centers for Disease Control and Prevention, 19 Apr. 2016. Web. 16 Apr. 2017.
- “Mammograms.” American Cancer Society. American Cancer Society, 16 Aug. 2016. Web. 18 Apr. 2017.
- “Cancer Screening Guidelines | Detecting Cancer Early.” American Cancer Society. American Cancer Society, 7 July 2017. Web.
- “Breast Ultrasound.” American Cancer Society. American Cancer Society, 18 Aug. 2016. Web. 16 Apr. 2017.
- “Breast MRI Scans.” American Cancer Society. American Cancer Society, 18 Aug. 2016. Web. 16 Apr. 2017.
- “Fine Needle Aspiration Biopsy (FNAB).” Genesis Health. Genesis Health, n.d. Web. 17 Apr. 2017.
- “Breast Biopsy.” American Cancer Society. American Cancer Society, 18 Aug. 2016. Web. 17 Apr. 2017.
- “Types of Cancer Treatment.” National Cancer Institute. National Cancer Institute, 06 Apr. 2017. Web. 17 Apr. 2017.
- “Breast-conserving Surgery: Lumpectomy or Wide Local Excision.” Breast Cancer Care. Breast Cancer Care, 19 Aug. 2016. Web. 20 May 2017.
- “What Is Mastectomy?” Breastcancer.org. Breastcancer.org, 02 May 2016. Web. 18 Apr. 2017.
- Schmauss, Daniel, Hans-Günther Machens, and Yves Harder. “Breast Reconstruction after Mastectomy.” Frontiers in Surgery. Frontiers Media S.A., 19 Jan. 2016. Web. 17 Apr. 2017.
- “Types of Breast Reconstruction.” Breastcancer.org. Breastcancer.org, 20 July 2016. Web. 20 May 2017.
- “Implant Reconstruction.” Breastcancer.org. Breastcancer.org, 26 Apr. 2017. Web. 19 May 2017.
- “Autologous or “Flap” Reconstruction.” Breastcancer.org. Breastcancer.org, 14 Feb. 2017. Web. 19 May 2017.
- “Nipple Reconstruction.” Breastcancer.org. Breastcancer.org, 26 Apr. 2017. Web. 19 May 2017.
- “Keeping Your Sex Life Going despite Cancer Treatment.” American Cancer Society. American Cancer Society, 29 Aug. 2013. Web. 17 Apr. 2017.
Last updated: 28 November 2017.
