
Cervical cancer is cancer of the cervix, the tube-shaped structure that connects the vagina and the uterus. The World Health Organization estimates that over one million females are living with cervical cancer around the world.1 The National Cancer Institute approximates 12,900 females were diagnosed in 2015 alone.2 According to the American Cancer Society, 4,120 females are expected to die from cervical cancer in America in 2016. The majority of cervical cancer cases are caused by long-term infection with the human papillomavirus (HPV). HPV is the most common sexually transmitted infection (STI), and is often spread through vaginal or anal sex. Generally, the HPV infection will go away on its own and thus does not cause any serious medical harm. However, cancer can arise when the viral infection persists for several years or even decades.3
Cervical cancer is a disease of the cells lining the cervix, which include squamous cells and glandular cells. Before cancer develops, the cells first exhibit pre-cancerous changes, which are detectable by a Papanicolaou test (Pap test). A Pap test or a Pap smear is a cervical screening used to detect pre-cancerous or cancerous cells. The two main types of pre-cancerous and cancerous cervical cells are squamous cell carcinomas and adenocarcinomas.4 Nine out of ten cervical cancers are squamous cell carcinomas.Squamous cell carcinomas are cancer of the flat, skin-like cells that line the outer layer of the cervix. Adenocarcinomas are cancer of the gland cells that produce mucus. Not every female who has the pre-cancerous cells will develop cancer; frequently, the pre-cancerous cells go away without treatment. If treatment begins early on, pre-cancerous cells almost always go away. There are usually very few signs and symptoms if cancer does develop. If cancer does develop, there are usually very few signs and symptoms. However, advanced cancers may cause unusual bleeding or discharge from the vagina, alerting the female of a potential health issue.
Causes and Prevention
Cervical cancer is caused by abnormal changes in the cells lining the cervix. These abnormal changes are often associated with HPV infection. The human papillomavirus is spread through penile/vaginal, anal, or oral sex with an infected individual. Since HPV infections are not always symptomatic, many people are unaware that they are infected. As a result, everyone who is sexually active is at risk for contracting the virus. There are 150 types of human papillomaviruses. Not all types of the virus have the potential to cause cancer, as some HPV types cause genital warts. However, it is difficult to tell with which type of HPV one is infected. Additionally, not all females who become infected with carcinogenic (or cancer causing) HPV will develop full stage cancer.
HPV infection causes about 70% of all cervical cancer cases. Since HPV is a sexually transmitted virus, using barrier contraceptives can help prevent females from developing cervical cancer. Barrier contraceptives can help eliminate skin-to-skin contact of infected areas, such as genitalia, therefore eliminating the means by which a sexually transmitted virus can spread.
Additional causes of cervical cancer can occur at the molecular level, often without an external cause. Cervical cancer, much like most cancers throughout the body, can be caused by damage and mutation of DNA, the genetic material inside all of our cells. For example, there are genes within our genome (i.e., the complete set of genetic material within an individual, that promotes cell division) called oncogenes, and genes that slow cell division, called tumor suppressor genes. Tumors are characterized as a mass of rapidly and uncontrolled cell divisions. Gene mutations can cause oncogenes to be expressed at a higher rate than desired, and thus can promote excessive cell division, which can quickly become cancerous. Similarly, gene mutations in tumor suppressor genes can prevent the slowing of cell division and, therefore, lead to tumor formation. Many researchers and physicians around the world are studying these DNA mutations and looking for ways to treat and prevent these cancer-causing damages.5
There are several risk factors that are associated with the development of cervical cancer. The following have been identified as such:

- Smoking: Females who smoke are at higher risk of developing cervical cancer. This risk increases with number of cigarettes smoked per day, age at diagnosis of cancer, and number of years of active smoking. Females who have successfully quit smoking are at lower risk than current smokers. Additionally, smoking is linked with an increased risk of contracting HPV. Smokers generally keep their HPV infections longer, and therefore have a higher incidence rate of developing cancer from an HPV infection.6 The mechanisms behind smoking and its role in increasing the risks of contracting cervical cancer are not fully understood, however, researchers currently believe that smoking suppresses the body’s immune system from fighting the viral infection and that the carcinogens from smoking amplify the HPV infection.7
- Prolonged Use of Oral Contraceptives: Long-term (five or more years) use of birth control pills is linked to heightened risk of cervical cancer. Researchers at the National Cancer Institute believe that the hormones in the pills cause cervical cells to be more vulnerable to HPV infections.8
- Weakened Immune System: Females who are infected with the human immunodeficiency virus (HIV) are at increased risk for cervical cancer because they are more susceptible to all infections, including HPV infection. HIV infections cause a weakened immune system, which prevents the body from successfully fighting off cancer cells. Additionally, females who are taking any drugs that suppress their immune systems, such as those used to treat autoimmune diseases, will experience similar risks.
- Chlamydia Infection: Studies have shown that females who are or have once been infected with chlamydia are at greater risk of cervical cancer.9
- Multiple Pregnancies: Females who have had three or more full-term pregnancies are at increased risk of developing cervical cancer.
- Many Sexual Partners: Females are at higher risk for cervical cancer if they have had many sexual partners, as they are more likely to contract HPV.
By avoiding these risk factors, a female can reduce her chances of developing cervical cancer. The best measure a female can take to prevent cervical cancer is to avoid contracting HPV. In addition to limiting the possibility of having unprotected sexual intercourse with an HPV infected individual, there is a vaccine administered that offers immunity to HPV. The HPV vaccine protects against four major types of HPV, including types 16 and 18. These two HPV strains account for 70% of all cervical cancer cases. The National Cancer Institute expects the protection provided by the vaccines is long lasting and highly effective. Vaccination is recommended for pre-teen girls, as it is important for females to be vaccinated before their first sexual encounter.
Pap Test
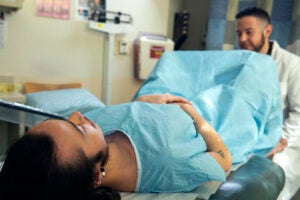
As with any cancer, or even infection, early detection allows for the most effective treatment. In regards to cervical cancer, doctors can detect pre-cancerous cells, and treatments can begin immediately to significantly decrease the chances of developing cancer. Cervical cancer screenings include cytology-based screenings, more commonly known as Pap tests and Pap smears, and HPV tests.10 Pap tests can detect “abnormal,” or pre-cancerous and cancerous, cells. HPV testing detects the presence of the HPV virus and specifically looks for the oncogenic, or cancer-causing, types by detecting the presence of DNA or RNA (the genetic material of the cell) specific to carcinogenic HPV types.
Pap tests are performed in a medical office, a clinic, or a community health center. During the test, the female lies on her back while the physician inserts a speculum, a hollow cylinder-shaped medical instrument, into her vagina in order to widen it. The widening of the vagina allows the upper portion of the vagina and the cervix to become visible. The physician will then take a sample of the cervical cells using a wooden or plastic scraper. The cells are then mounted onto slides and sent to laboratories for testing and analysis.
In the United States, physicians recommend that females begin having regular Pap tests every three years, beginning at the age of 21. Regardless of the country of residency, females are encouraged to have regular pelvic exams and Pap tests. Any female who has one or more of the risk factors for cervical cancer should consider having more frequent pelvic examinations by her doctor.
Pap tests will either come back as “normal,” “unclear,” or “abnormal.” If the results are normal, this means that no cell abnormalities were found in the cervix and no further tests will likely be performed. However, it is still important to continue to get Pap tested every few years as changes in the cells can occur later on. If the results were unclear, meaning that the Pap test showed possible cell abnormalities, the physician may follow up with an HPV test to determine whether or not the detected abnormalities are connected to HPV. After the results of the HPV test come back, further testing or treatment will be determined as seen fit by the physician. Lastly, if the Pap test results come back abnormal, this means that cell changes were detected in the cervix. These cell abnormalities do not necessarily mean cancer. The changes can be minor (low-grade) or serious (high-grade). If they are low-grade changes, the cells may go back to normal on their own. If the chances are high-grade, they are considered pre-cancerous and it is likely that the physician will follow-up with additional tests and will begin treatment as soon as possible.
Diagnosis
Pap tests are the first step towards diagnosing cervical cancer. If a Pap test comes back “abnormal,” then further tests will be ordered. The first follow up test is usually a physical examination. The physician will take a medical history, if one is not already on file. The physician will likely ask about possible risk factors specific to cervical cancer (see above).
The physical exam will help assess the overall physical health of the patient. The lymph nodes, small organs in the immune system, will be assessed to determine the possible presence of metastasis (a tumor that has spread to another part of the body).
Diagnostic tests to further determine the presence of cancer include a colposcopy (with biopsy) and an endocervical scraping. During a colposcopy test, the female will lie on the exam table, while a speculum is placed inside the vagina so that the cervix becomes visible. A physician uses a colposcope, a magnifying lens instrument, to examine the cervix. A weak solution of acetic acid is used to make any abnormal cells easier to visualize. If a physician locates the presence of abnormal cells, then a biopsy will be performed. During a biopsy, a small piece of tissue is removed and sent to the laboratory to be looked at under a microscope. The biopsy will determine whether the abnormalities are pre-cancerous, cancerous, or benign (harmless). Endocervical scraping is performed if the colposcope is not successful at visualizing the cervical cells. A curette, or a narrow instrument, is used to scrape the endocervix, or the opening of the uterus, to remove tissue. This tissue is then sent to the laboratories.
If the biopsies detect the presence of pre-cancerous cells, the results are read as cervical intraepithelial neoplasia (CIN). CIN is a rating on a scale of one to three, depending on the severity of the abnormalities. CIN 1 means the changes are less serious, while CIN 3 means the changes are the most serious. If the biopsy detects the presence of cancer, and not simply pre-cancerous cells, the results will read squamous cell carcinoma or adenocarcinoma.
If cervical cancer is detected (meaning the abnormalities are cancerous, opposed to pre-cancerous, changes), additional tests will be ordered.11 These additional tests may include the following:
- A Cystoscopy or Proctoscopy Examination Under Anesthesia: This test is done for females only if there is a large tumor and the cancer was not detected early. The cystoscopy is used to better visualize the tumor. A proctoscopy is also used to examine the rectum to determine whether or not the cancer has spread.
- Chest X-Ray: Chest x-rays are used to determine if the cancer has spread to the lungs. Cervical cancer usually only spreads to the lungs in the most advanced cases, however, because of the seriousness of lung cancer, physicians often choose to check the lungs.
- Computed Tomography (CT): A CT is an x-ray examination that images a cross-section of the body. This image depicts a “slice” of the body, much like a slice of bread. CT images can help determine if the cancer has spread to other parts of the body, including the liver, lymph nodes, pelvis, lungs, or elsewhere.
- Magnetic Resonance Imaging (MRI):MRIs use radio waves and large magnets to image the body. The energy emitted from the radio waves is absorbed and released in unique patterns by different types of tissue in the body. A computer analyzes those emitted patterns and generates an image of the examined body part. MRI images are useful in examining the pelvic area and are used to determine whether or not the cancer has spread to the brain or spinal cord.
- Intravenous Urography: Intravenous urography is an x-ray of the urinary system, which uses a specific dye that is injected into a vein. The dye passes through the kidney into the bladder. This test helps determine whether or not the cancer has spread to the pelvic area. Intravenous urography is not used if a CT or MRI image has already been obtained.
- Positron Emission Tomography (PET): PET scans use radiolabel glucose (simple form of sugar). Glucose is absorbed in large amounts by cancerous cells because cancer cells need a lot of energy to quickly divide and grow. PET scans are specifically useful in detecting the spread of cancer in the lymph nodes or determining the location of the metastasis.
If a female receives a formal diagnosis of cervical cancer from her physician, she may choose to get a second or third opinion by contacting additional doctors. Receiving second opinions can ensure that the female undergoes the most appropriate treatment. Going to additional doctors’ offices should take no longer than a week or two and will likely increase the chances of successful treatment. The diagnosing physician may be able to offer referrals for the additional opinions, or a female can contact The Cancer Information Service, at 1-800-4-CANCER, for additional referrals.12
Asking a doctor questions about planned treatment will help a female learn about the treatment opinions. Taking an active role in these important decisions may help a female feel more comfortable and more trusting of the treatment process. The following are some of the possible questions one might want to ask:
- What is the stage (extent) of my disease?
- What are my treatment options? Which do you recommend for me? Why?
- What are the risks and possible side effects of each treatment?
- How long will treatments last?
- How will various treatments affect my normal activities?
- What is each treatment likely to cost?
- What is likely to happen without treatment?
- How often will I need to have checkups?
Stages of Cervical Cancer
There are four stages of cervical cancer depending on various characteristics of the cancer.13
Stage 0: Cervical cancer in stage 0, or the earliest stage, is referred to as a carcinoma in situ. A carcinoma in situ is when abnormal cells are found on the innermost lining of the cervix. These abnormalities can develop into a tumor with the possibility of metastasizing (the tumor spreading and growing on another part of the body).
Stage I: Stage I cervical cancer is when the cancer is localized to the cervix. This stage is divided into two additional stages, stages IA and IB.
- Stage IA: The cancer is minimal and can only be seen with a microscope. Stage IA is divided into two more stages, stages IA1 and IA2, based on tumor size.
- Stage IA1: The cancer is smaller than three millimeters deep and smaller than seven millimeters wide.
- Stage IA2: The cancer is between three millimeters and five millimeters deep and smaller than seven millimeters wide.
- Stage IB: The cancer is larger than a Stage IA tumor. Stage IB is divided into two more stages, stages IB1 and IB2, based on tumor size.
- Stage IB1: The cancer is more than five millimeters deep and more than seven millimeters wide, or the cancer can be seen without a microscope, but is not more than four centimeters wide.
- Stage IB2: The cancer is visible without a microscope and is larger than four centimeters.
Stage II: In stage II, the cancer has metastasized (spread) from the cervix, but has not reached the pelvic walls or the lower third of the vagina. Stage II is divided into two stages, Stage IIA and Stage IIB, depending on how far the tumor has spread.
- Stage IIA: The cancer has spread to the upper two thirds of the vagina. Stage II cancer is divided in two additional stages, stages IIA1 and IIA2, based on the size of the tumor.
- Stage IIA1: The tumor is not visible without a microscope and is smaller than four centimeters.
- Stage IIA2: The tumor can be seen without a microscope and is larger than four centimeters.
- Stage IIB: The cancer has spread to the tissues around the uterus (but not to the pelvic wall).
Stage III: In Stage III, the cancer has spread to the lower third of the vagina and/or onto the pelvic wall. During Stage III cervical cancer, kidney problems can evolve. Stage III is divided into two additional stages, stages IIIA and IIIB, depending on how far the cancer has spread.
- Stage IIIA: The cancer has spread to the lower third of the vagina, but not to the pelvic wall.
- Stage IIIB: The cancer has spread to the pelvic wall, or the tumor is large enough to block one or both ureters (the tubes connecting the kidney with the bladder), causing one or both kidneys to have problems.
Stage IV: In Stage IV, the cancer has spread beyond the pelvis. The cancer may have gone to the bladder or rectum, or other parts of the body. Stage IV is divided into two stages, stages IVA and IVB, depending on where the cancer has spread.
- Stage IVA: The cancer has spread to the nearby organs, including the bladder or rectum.
- Stage IVB: The cancer has spread to other parts of the body, beyond the pelvic area. Additional metastases may include, but are not limited to, liver, lungs, bones, or distant lymph nodes.
Discussing Treatments With Your Physician
Treatment for cervical cancer depends on many factors including the stage of the cancer, the size of the tumor, the depth of invasion (how deep into the cervix the tumor has grown) and whether or not it has spread to other parts of the body.
When choosing treatment options, it is important for the patient to get involved in the decision making process. There are a multitude of factors that go into choosing the treatment option that is right for each individual. The characteristics and severity of the cancer itself are important, but other significant factors include financial status, social support, overall health, age, individual preferences, and other personal circumstances. It is imperative for the individual to consider all such concerns before settling on a treatment option. The patient should discuss all the possible options with a doctor before settling on a decision. A female may want to be aware of the treatment’s goals, possible side effects, costs, and lengths. The following are some questions a patient may want to ask while discussing treatment options with a physician:
- What are my treatment options?
- Which treatment do you recommend and why?
- What are the risks and side effects of the different treatments?
- Which treatments will allow me the option to have children in the future?
- Is it possible that my cancer will come back after I undergo treatment?
- Will I need to alter my life style in any way during treatment (diet, exercise, etc.)?
- What are the popular treatments for other patients?
It may be useful to talk to a few different specialists before choosing a treatment plan in order to understand all the different options that are available. Specialists who can provide the most useful information about treating cervical cancer include: a gynecologist (a physician who works with the health of the female reproductive system), a gynecologic oncologist (a gynecologist who specializes in cancer of the female reproductive system), a radiation oncologist (a physician who treats cancer using radiation), and a medical oncologist (a physician who treats cancer using chemotherapy). Lastly, it may be beneficial to get a second opinion from another physician of the same specialty before undergoing treatment. Second opinions can help patients feel more confident in their chosen treatment as well as provide a source of additional information.
Treatment
There are three main treatment options for patients diagnosed with cervical cancer: surgery, radiation, and chemotherapy.14 The use of angiogenesis inhibitors (drugs that prevent angiogenesis, or the formation of new blood vessels, which is often associated with the growth of a tumor) is also a treatment option. Additionally, researchers are studying the use of various targeted treatments, which include drugs that specifically target cancer cells.15
Surgery
If cervical cancer is in Stage 0, there are two surgical options available.16 The first, cryosurgery, uses a metal probe lined with liquid nitrogen that is placed onto the cervix. The probe kills abnormal cells by freezing them. Cryosurgery can be done in a doctor’s office or in a clinic. In the following week post-surgery, the female may notice watery, brown discharge as a result of this procedure. This discharge is normal and does not need to be met with worry or concern. The second option is laser surgery in which a laser beam is directed through her vagina onto the cervix. The laser burns off abnormal cells. Laser surgery can be performed in the doctor’s office or a clinic under local anesthesia.
If the cervical cancer is in Stage IA1, the cancer can be treated using either a Conization procedure, or a hysterectomy. During a Conization treatment, a surgeon uses a surgical knife, a laser knife, or a heated wire to remove a cone-shaped piece of tissue from the cervix. The tissue is examined under microscope to determine if additional treatments are needed. A hysterectomy is the surgical removal of the uterus, including the cervix. There are three forms of a hysterectomy, including an abdominal hysterectomy, a vaginal hysterectomy, and a laparoscopic hysterectomy. An abdominal hysterectomy involves the removal of the uterus through an incision in the front of the abdomen. During a vaginal hysterectomy, a surgeon removes the uterus through the vagina.
A laparoscopic hysterectomy is a minimally invasive surgery that involves the removal of the uterus through a small naval incision. A laparoscope (a tubed surgical instrument with a camera at the end) allows for the small incision because it provides the surgeon visualization of the patient’s insides without having to open the body up wider. A female is under general anesthesia (a controlled, unconscious, mental state the patient enters after receiving medications) during hysterectomies. The hospital stay for vaginal and laparoscopic hysterectomies is one to two days, followed by a two to three week recovery period. The hospital stay for an abdominal hysterectomy is three to five days, followed by a four to six week recovery period. The abdominal hysterectomy has a longer recovery time because it is a more invasive surgery than the other two. Due to the fact that these procedures involve the total removal of a reproductive sex organ, the patient is sterile after a hysterectomy.
For cancer in Stages IA2 and II, the patient may undergo a radical hysterectomy or a radical trachelectomy. A radical hysterectomy involves the removal of the uterus and additional surrounding tissue, including the upper part of the vagina. This procedure is performed via an incision in the abdomen. There is a laparoscopic-assisted form of radical hysterectomy, called laparoscopic-assisted radical vaginal hysterectomy, which allows for a smaller surgical incision. The hospital stay for a radical hysterectomy is five to seven days. A radical trachelectomy is a less common form of treatment than a radical hysterectomy, however, it does not make the patient sterile, and thus gives the female the option of having children in the future. During a trachelectomy, the cervix and the upper part of the vagina are removed while leaving the uterus in place. This operation is done through the vagina or abdomen.
If cancer is reoccurring, the patient may choose to undergo pelvic exenteration, in which the uterus, cervix, vagina, pelvic lymph nodes, bladder, rectum, and parts of the colon may be removed. Clearly, this is a much more extensive surgery and may result in drastic life style changes. Some adaptations that patients may have to undergo after receiving this surgery can include using a new method to store and eliminate urine due to the removal of the bladder, or a new system to remove solid waste due to the removal of the rectum. Due to the highly invasive nature of this procedure, the recovery time is between six and twenty-four months.
The following are some questions a patient may want to ask prior to surgery:
- What kind of operation will it be?
- How will I feel after the operation?
- What kinds of side effects can I expect?
- If I have pain, how can you help me?
- When can I return to my normal activities?
- How will this treatment affect my sex life?
Radiation Therapy
Radiation therapy is the use of high energy x-rays to kill cancer cells.17 There are several different types of radiation therapy used to treat cervical cancer. One radiation treatment uses external beam radiation therapy (EBRT). EBRT uses x-rays from outside the body and aims them at the cancer. This treatment is similar to receiving a regular x-ray, but the radiation dosage is much stronger. The procedure is not painful, but is often accompanied with many side effects, including tiredness, pain in the stomach, diarrhea, nausea and vomiting, and changes to the skin. Radiation passing through the skin causes changes to the skin. Changes include skin pigment changing form pink to red. This change in pigment can be harder to see for darker skin tones, but there may still be symptoms such as dry skin and soreness.21 The radiation may cause discomfort to the bladder, frequent urges to urinate, soreness to the vulva and vagina, discharge, menstrual changes, or early menopause. Radiation can also cause anemia (low red blood cell count) and leukopenia (low white blood cell count).
A brachytherapy, or internal radiation therapy, is a procedure in which a source of radiation is place in or near the cancer. A low-dose rate brachytherapy lasts several days, during which the patient remains in the hospital. With a high-dose rate brachytherapy, the treatment is performed over several weeks; over the course of this treatment, the patient comes in and has the radioactive source placed at the site of the cancer for a few minutes at a time. Side effects for internal radiation therapy include irritation to the vagina and vulva. Low-dose brachytherapy is often used in patients with earlier stages of cervical cancer versus a high-dose brachytherapy which will be used for a more advanced form of cervical cancer. Brachytherapy is oftentimes used in additional to EBRT.
The following are some questions that a patient may want to ask a doctor before starting radiotherapy treatment:
- What is the goal of this treatment?
- How will the radiation be given?
- How long will treatments last?
- How will I feel during therapy?
- What can I do to take care of myself during treatment?
- Can I continue my normal activities?
- How will this treatment affect my sex life?
Chemotherapy
Chemotherapy (chemo) is the treatment of cancer using anti-cancer drugs that are injected in the veins or taken orally.18 The drugs enter the blood stream and reach all areas of the body. The drugs target rapidly dividing cells, which are characteristic of cancer cells. However, it is possible that the chemo drugs will also target healthy cells, which is the source of many of the side effects associated with chemotherapy. These side effects include nausea and vomiting, loss of appetite, loss of hair, mouth sores, and tiredness. Additionally, if chemotherapy drugs target blood-producing cells of the bone marrow, the patient’s blood cell count might decrease and lead to a heightened risk of infection, bleeding, easy bruising, and shortness of breath. Changes in the menstrual cycle may be a side effect if the female has an intact uterus. Even if the female’s periods stop while on chemo, she still has the possibility of getting pregnant. Pregnancy during chemotherapy can cause severe birth defects. Any sexually active female should use birth control while undergoing chemotherapy. Once the patient stops receiving chemotherapy, the pregnancy is no longer at risk of contracting the birth defects associated with the chemotherapy. However, in some cases, there is a possibility of premature menopause and/or permanent infertility (not being able to become pregnant).
If cancer has metastasized (spread) throughout the body, chemotherapy is the most likely treatment that a patient will undergo. Additionally, if the cancer is reoccurring, chemo is a good choice for reintroducing treatment. Chemotherapy is often given in treatment cycles interrupted by recovery periods. Chemotherapy is often used in addition to radiation therapy because the chemo increases the effectiveness of the radiation. When chemotherapy is combined with radiation, side effects are often more severe.
The following are some questions that a patient may want to ask a doctor before chemotherapy begins:
- What is the goal of this treatment?
- What drugs will I be taking?
- Do the drugs have side effects? What can I do about them?
- How long will I need to take this treatment?
Clinical Trials
A patient may want to ask her health care provider about possible clinical trails and whether they are appropriate for her situation. A clinical trial is a scientific study that tests the safety and effectiveness of new medical treatments. The benefit of being in a clinical trial is that a patient has the chance to be the first to receive new, possibly more effective treatment methods while helping contribute to medical science. Some patients who participate in clinical trials will be part of the control group and receive the standard treatment approach, serving as a comparison for the new approach. Other participants in the clinical trial will serve as the experimental group and recieve the new treatment approach. Currently, there are clinical trails being developed for new treatments of cervical cancer.19
Sex with Cervical Cancer
A female can still have an active, healthy sex life after being diagnosed with cervical cancer.20 Depending on what treatment she chooses to undergo, the female may have to recuperate during a predetermined amount of recovery time before engaging in sexual activities. For a patient who has a hysterectomy, sexual pleasure is not affected. The sensitive sex organs (the clitoris and the vagina) are not affected by hysterectomies. For females who receive radiation therapy, their vaginas may become dry which can cause painful intercourse. The doctor can prescribe local estrogens to aid with the dryness in order to eliminate pain during sex. A female may even experience a heightened sex life post-treatment due to the new found relief from the sexual pain and discomfort that might have occurred as a result of the previous cancer.
Concluding Remarks
Cervical cancers are one of the most common cancers in females worldwide. The cancer occurs when the cells of the cervix grow abnormally. Symptoms of cervical cancer may include abnormal bleeding from the vagina, pain in the lower pelvic area, pain during coitus, and abnormal vaginal discharge. Most cervical cancer cases are caused by infection of the sexually transmitted human papillomavirus (HPV). Since HPV is the most common sexually transmitted infection, doctors recommend females take preventative measures to avoid contracting the virus. These measures may include an HPV vaccination and/or use the of barrier contraceptives during sexual activities. Treatments for the cancer are usually successful when caught early. Early detection is made possible by frequent Pap tests. In countries like the United States, where cervical cancer screenings are routine, the incidence of cervical cancer significantly decreases. There are many different treatments available to a female with cervical cancer. Discussing the cancer with a doctor and learning more about the different treatment options can help a patient decide on the right course of action. With the medical advances available today, it is now easier for a female to be successfully treated for this cancer and go on to live a happy, healthy life.
References
- “Screening as Well as Vaccination Is Essential in the Fight against Cervical Cancer.” World Health Organization. N.p., 2016. Web. 22 May 2016.
- “Cervical Cancer.” National Cancer Institute. N.p., n.d. Web. 22 May 2016.
- “Genital HPV Infection – Fact Sheet.” Centers for Disease Control and Prevention. Centers for Disease Control and Prevention, 18 Feb. 2016. Web. 22 May 2016.
- “What Is Cervical Cancer?” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “Cancer Biology.” National Cancer Institute. N.p., n.d. Web. 22 May 2016.
- “Cervical Cancer and Smoking.” Foundation for Women’s Cancer (2012): n. pag. Web. 22 May 2016.
- “Stop Smoking and Reduce Your Cervical Cancer Risk.” EverydayHealth.com. N.p., n.d. Web. 22 May 2016.
- “Oral Contraceptives and Cancer Risk.” National Cancer Institute. N.p., n.d. Web. 22 May 2016.
- “Untreated Chlamydia Infections Linked To Cervical And Other Gynecological Cancers.” Medical Daily. N.p., 21 June 2013. Web. 22 May 2016.
- “Pap and HPV Testing.” National Cancer Institute. N.p., n.d. Web. 22 May 2016.
- “How Is Cervical Cancer Diagnosed?” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “NCI Contact Center.” National Cancer Institute. N.p., n.d. Web. 22 May 2016.
- “How Is Cervical Cancer Staged?” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “How Is Cervical Cancer Treated?” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “Targeted Therapy for Cervical Cancer.” Targeted Drug Therapy for Cervical Cancer. N.p., 01 Jan. 0001. Web. 22 May 2016.
- “Surgery for Cervical Cancer.” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “Radiation Therapy for Cervical Cancer.” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “Chemotherapy for Cervical Cancer.” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “Cervical Cancer Clinical Trials & Research.” Cervical Cancer:. N.p., n.d. Web. 22 May 2016.
- “Sexuality for the Woman With Cancer.” American Cancer Society. N.p., n.d. Web. 22 May 2016.
- “Side Effects of Radiation Therapy.” Cancer.Net. American Society of Clinical Oncology. 15 Dec. 2015. Web 14 Oct. 2016.
Last Updated 20 October 2016.
