Table of Contents
Overview
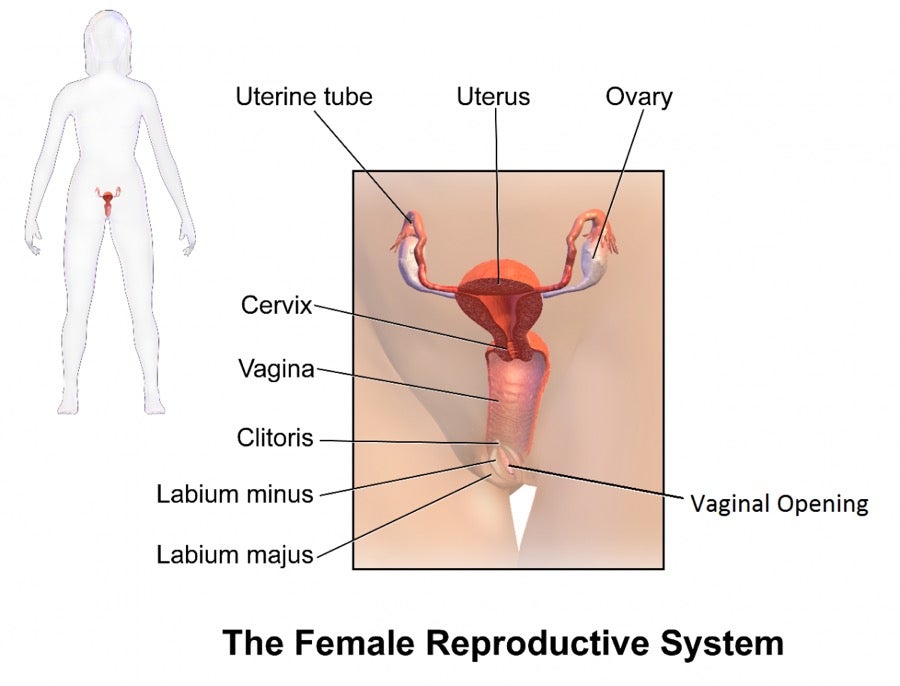
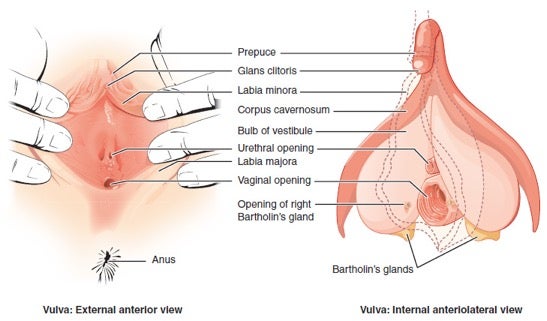
The vagina is a stretchable muscular cavity lined with mucous membranes in the female reproductive system that extends from the uterus (womb) to the vaginal opening. The cervix of the uterus forms the interior end of the vagina, while the vulva–or the external parts of the female genitalia–and labia (singular: labium) form the exterior end. The vaginal opening may be slightly covered or surrounded by the hymen.1 Externally, the vaginal opening is located between the urethral opening and the anus.
The vagina has several functions. Once a female begins her menstrual cycle, menstrual blood will flow out of the uterus and exit the body through the vagina. During sexual intercourse, the penis penetrates the vagina, and in the course of childbirth, the vagina also serves as a birth canal for the baby. The vagina experiences several transformations during pregnancy and childbirth. The vagina also experiences different changes as a result of age, diet, and activity. Each vagina may vary significantly from person to person. Doctors have described differences in vaginal color as varying from light pink to a deep brownish red-pink hue.2

Generally, the vagina is collapsed and about 3 to 5 inches long in an unaroused female. When the female experiences sexual arousal, the vagina elongates, expands, and becomes lubricated. Sometimes additional lubrication may be needed to increase comfort during sexual activities.
Normally, the vagina is inhabited by large quantities of “friendly” or “healthy” bacteria that convert sugars into lactic acid. This naturally-occurring bacteria makes the vaginal surface mildly acidic in order to prevent the growth of harmful bacteria.3
Functions
The vagina functions in different ways throughout the menstrual cycle, sexual intercourse, and childbirth.
Secretions and the Menstrual Cycle
Once a female begins puberty, the vagina plays a prominent role in creating a healthy, fertile environment for potential sperm. A healthy, fertile environment is essential for conception because sperm need to survive their passage through the vagina in order to fertilize the ovum (or egg) and cause pregnancy. Due to changes associated with puberty, just before the onset of the female’s first period, the vagina begins continuously producing a discharge (called leukorrhea) that acts primarily as a germ- and pollutant-removing mechanism. Leukorrhea is the byproduct of vaginal cleaning. This discharge varies slightly in texture and color between individuals. Vaginal discharge may appear thicker or stickier depending on the timing of one’s menstrual cycle but usually has a smooth, slightly sticky texture and is a clear or white color.4 Due to this process, the vagina is considered a self-cleaning cavity because it ensures that no bacteria or other harmful substances enter it.
There are multiple types of discharge. When a female becomes sexually aroused, a clear and slippery discharge is produced. In the lubricating process known as vaginal transudation, this moist, slippery discharge seeps through the vaginal walls to serve as a natural lubricant.5
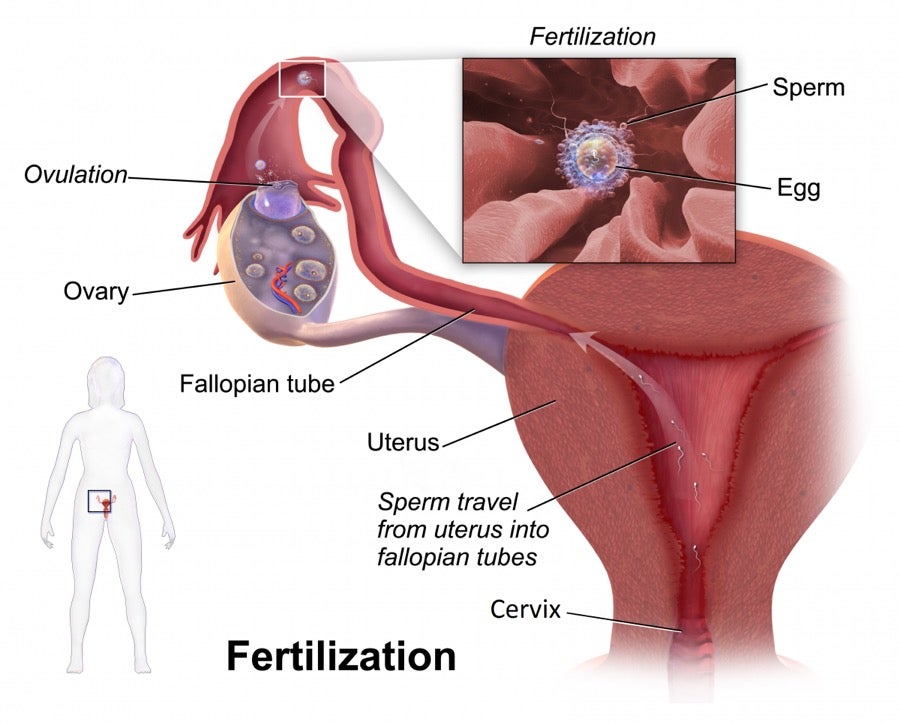
Before and during ovulation, the cervix naturally produces mucus as the result of hormonal changes during the menstrual cycle. The quantity and quality of this vaginal discharge fluctuates in accordance with the individual’s fertile days.6 When the body is not approaching or undergoing ovulation, cervical mucus functions as a barrier which prevents sperm from entering the uterus, since pregnancy cannot occur without ovulation.7 As one approaches ovulation, increased estrogen levels cause the cervix to produce additional cervical mucus which makes it easier for sperm to reach the egg.6 On the most fertile days, cervical mucus is typically very stretchy and clear. This increased cervical mucus secreted on fertile days protects and helps sperm travel to the ovum.7 Cervical mucus can be monitored as a natural method of contraception or for an increased likelihood of conception. The cervical mucus method of fertility awareness involves charting any changes in cervical mucus over a 28-day cycle. Although fertility cycles may vary from person to person, a typical fertility cycle tends to occur in the following pattern:
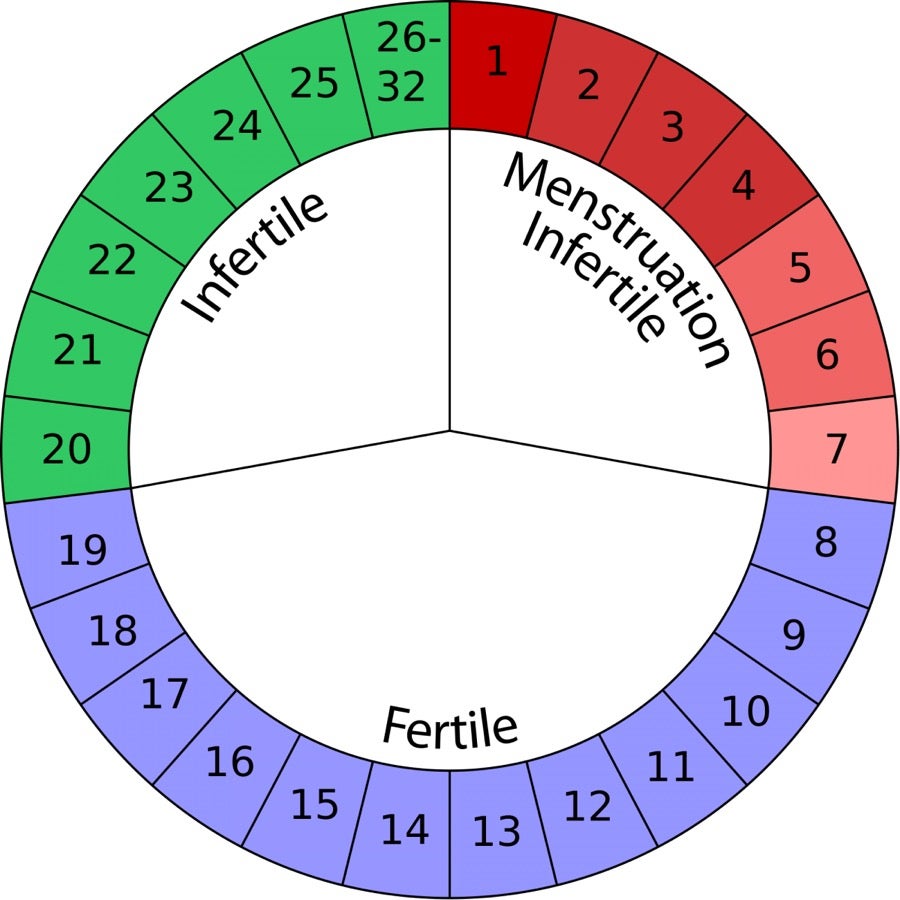
- Days 1-5: Menstrual blood exits the body as menstruation occurs
- Days 6-9: Vagina remains dry; cervix produces little to no mucus
- Days 10-12: Cervical mucus appears sticky and thick; mucus gradually becomes thinner and whiter
- Days 13-15: Cervical mucus appears thin, slippery, and clear or off-white; highest potential for fertility occurs during Days 13-15
- Days 16-21: Cervical mucus returns to sticky, thick state
- Days 22-28: Vagina becomes dry7
For more information regarding the cervical mucus method, read this article about fertility awareness!
Secretions during Pregnancy
Many pregnant females will experience a “pregnancy discharge” or an increased appearance of vaginal discharge while pregnant. Increased vaginal discharge occurs naturally in pregnant females, but should be monitored and reported to a doctor if any unusual smells or appearances develop and/or if one begins to experience pain, itching, or soreness in the vaginal area.
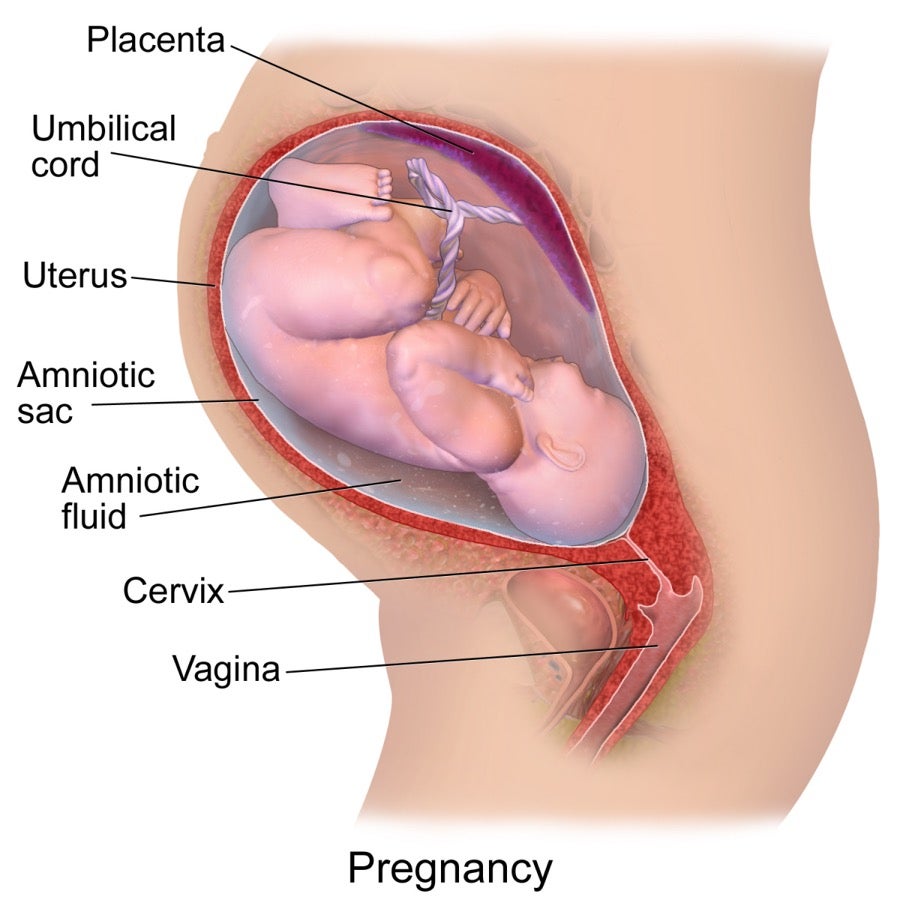
During pregnancy, the cervix produces increased vaginal discharge as a method of protecting the womb from infections that could potentially enter through the vagina. As a pregnant female approaches delivery, the positioning of the baby’s head often adds increased pressure onto the cervix, which can cause increased discharge and the frequent sensation or urge to urinate. In the final week of pregnancy, vaginal discharge may also contain some thick mucus and traces of blood due to a gradual breakdown of the cervical mucus plug, which is an accumulation of thick mucus that blocks off the cervix during pregnancy. This breakdown is a natural sign that the body is preparing to give birth soon. Although a small quantity of blood during pregnancy is usually of little cause for concern, it is imperative to contact a doctor or midwife if any pregnant female experiences bleeding from the vagina, as this may be an indication of a more serious issue.8
Secretions after Childbirth
Immediately after childbirth, the new mother will encounter some vaginal bleeding as her body works to shed the complete uterine lining created by the pregnancy. For approximately six weeks after childbirth, new mothers will experience a postpartum vaginal discharge known as lochia, which contains mucus, blood, and uterine tissue. This process of bleeding for about six weeks is known as a “postpartum period.” Lochia discharge often resembles a clear to creamy white color.9

Typically, most females will not begin menstruating until approximately six to eight weeks after childbirth, or the length of the postpartum period. This time range varies greatly depending on each mother’s schedule for breastfeeding. Females who breastfeed after giving birth tend to experience a lack of periods due to changes in the body’s hormones. As the hormone prolactin functions to produce breast milk in new mothers, it can also prevent menstruation and ovulation by suppressing the body’s reproductive hormones. While most non-breastfeeding females’ periods will return within six to eight weeks, some females may not experience a menstrual period the entire length of time spent breastfeeding. However, some females may have their periods return after a few months following childbirth, regardless of breastfeeding practices.9
The first period after childbirth differs significantly from periods encountered before the pregnancy occurred. Some of the differences in menstruation that females may experience after giving birth include the following:
- Experiencing cramps that are either stronger or lighter in intensity than normal
- Observing the presence of small blood clots
- Undergoing a heavier flow than in previous menstrual cycles
- Noticing an irregular menstrual flow that appears to start and stop unusually
As one’s menstrual cycle continues, the occurrence of these differences will likely decline.9
Sexual Activity
During sexual intercourse, the vagina functions as a passageway for the penis and plays a significant role in sperm transportation. Upon sexual arousal in the female, the vaginal walls prepare for entrance of the penis by secreting lubrication, lengthening, and expanding. The amount of time spent on foreplay changes both the lubrication level and the shape of female’s vagina. If a female is not properly and completely aroused, the female will not have a lot of natural lubrication, which will make their partner feel more friction that could end up causing them both to feel pain. Most of the time, the vagina lies flat, but when a female is aroused, the vagina lengthens and the inner two-thirds expand in a process called “tenting.” The biological function of this action is to create a receptacle for semen. When a female is properly aroused, the factors mentioned above may combine to make it feel as if their vagina is “looser,” but it should not be a concern as this is their body’s natural reaction to ensure that the sex is pleasurable and comfortable for them. Also, if a female has not had sex in a while, the muscles in their vagina will become used to being closed, causing their vagina to feel a little tighter than normal during the first occurrence of sex after a break.
Lubrication can make coitus easier and more pleasurable for both partners; it also has a near-neutral pH which creates a more fertile environment for sperm than does the naturally acidic state of the vagina. As a result of vasocongestion during sexual arousal, the color of the vagina usually shifts from a pink hue to a color closer to purple. The vagina can both expand and tightly contract around the penis to increase stimulation and achieve sexual satisfaction.3
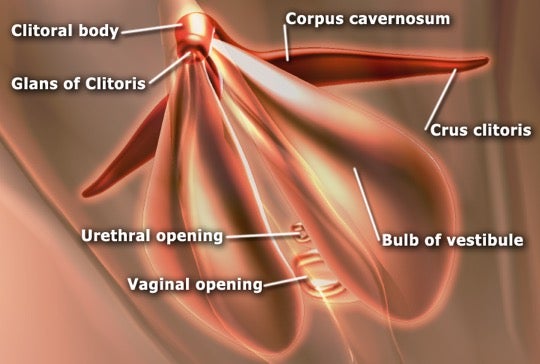
In terms of sexual pleasure and sensitivity, the vagina contains significantly fewer nerve endings than the clitoris because the vagina is more biologically functional for reproduction than erotic pleasure. Therefore, a female’s ability to receive an orgasm purely from vaginal penetration is often hindered.10 Penile-vaginal intercourse alone can feel extremely pleasurable, but incorporating clitoral stimulation and foreplay can help increase sexual satisfaction for both the female and the male. For additional information regarding solutions for female orgasmic difficulties, check out this article!
Although research regarding the orgasmic power of the Gräfenberg spot (or G-spot) remains debatable, stimulation of the G-spot on the anterior (or front) wall of the vagina may lead to an orgasm in some females. The G-spot is an area of heightened sensitivity that is typically located about one to two inches away from the vaginal opening.3 However, the existence of an exact anatomical location of the G-spot remains controversial among researchers.11 When unstimulated, the G-spot is generally small and flaccid, approximately the size of a bean. When a female is aroused, however, this area becomes more pronounced: it swells and may more feel more like a ridge than does the surrounding tissue in the vagina. Stimulation of the G-spot does not result in orgasm for all females and may actually trigger the urge to urinate. If stimulation continues after the sensation to urinate is triggered, one may experience an orgasm which can be categorized as a different quality than an orgasm produced through clitoral stimulation alone.3
Childbirth
The vagina also functions as a pathway for newborn babies to exit the womb. The vagina experiences several major changes around and after childbirth. Although every delivery varies, common changes in pregnant females who are about to give birth include pre-labor contractions, ruptured membranes (or one’s water breaking), and “pregnancy discharge” due to the repositioning of the fetus. Although pre-labor contractions usually include some pain, some females do not actually feel their pre-labor contractions because they are completely painless.12 As pregnant females approach delivery, pre-labor contractions naturally occur at regular intervals to push the baby out of the womb and through the vagina. These contractions gradually increase in duration, frequency, and intensity as the soon-to-be-mother gets closer to childbirth.3 True labor is typically associated with an hour-long period of contractions that each last for one minute in duration and occur every five minutes.13 For more information about “false labor” or Braxton-Hicks contractions, read this article about childbirth!
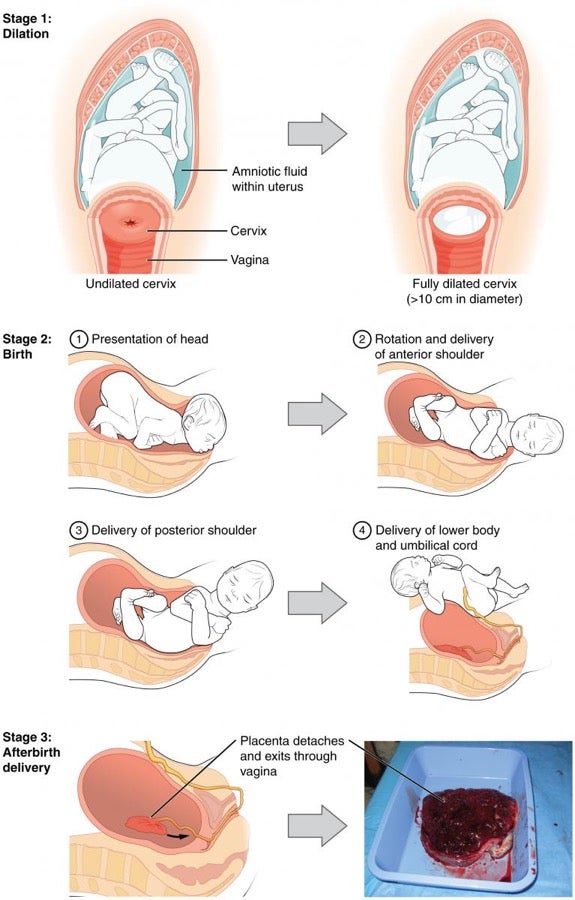
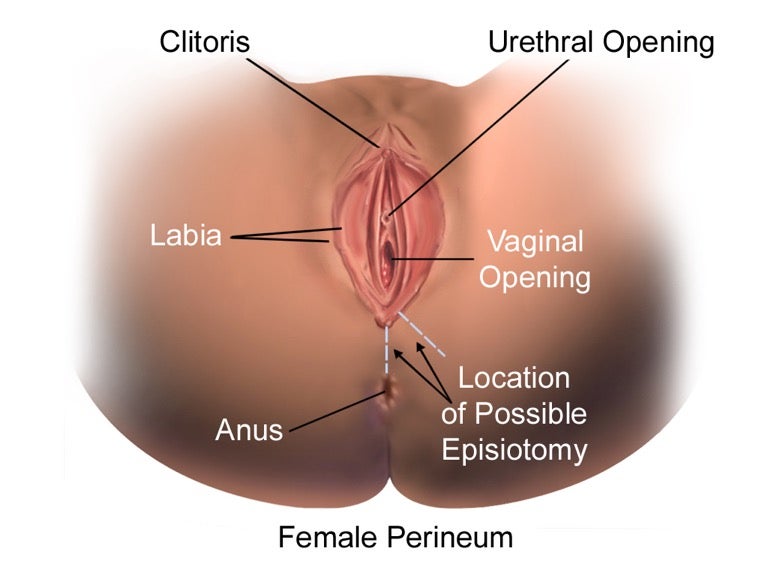
When the uterine contractions begin, the cervical canal starts to open until the cervix expands to 10 centimeters in diameter.13 Therefore, the fetus can no longer be supported by the cervix and it begins to move from the uterus to the vagina. The elastic capabilities of the vagina allow it to stretch wide enough for the baby to exit the female’s body.12 However, despite the flexibility of the vagina, an excessively forceful or rapidly-occurring delivery may cause some vaginal tissues and/or the perineum to tear during childbirth. As the vaginal walls and perineum expand to the point of tearing, the mother may feel tremendous pressure and a burning sensation around the skin being stretched by the baby’s head.13 In some cases, the perineum may be cut by a doctor in a procedure known as an episiotomy in order to provide a wider opening for vaginal delivery and to avoid potential tearing.8 Most new mothers recover from these tears and incisions without complications, although the use of stitches may cause discomfort and some difficulty during urination.13
It is common for females to undergo several natural changes to the vagina after giving birth. Although changes vary from person to person, many females experience feeling a wider or looser vagina after childbirth. Typically, the shape of the vagina will remain wider after childbirth than it was before having a child. Consequently, many females undergo urinary incontinence, or the inability to control urine leakage, after giving birth. Additionally, the vagina may also appear bruised or swollen for a few days following the birth. If an episiotomy was needed, the new mother may also experience soreness and pain around the vaginal area immediately after childbirth as a result of stitches in the perineum. Due to hormones associated with breastfeeding, the vagina often feels drier than it did before childbirth, increasing the likelihood that the female will experience pain during sex. Although lubrication may be necessary to improve sexual comfort in these situations, the dryness usually subsides after breastfeeding has ended and menstrual periods have returned.14
Improving Vaginal Muscles
Kegel Exercises
A great method females can use to increase the strength of their vaginal muscles (and in turn, the tightness of their vagina) is engaging in Kegel exercises. Kegel exercises help to increase sexual response and satisfaction by strengthening the pubococcygeus (PC) muscle, which forms the pelvic floor and supports the pelvic organs. New mothers can perform Kegel exercises to tighten the vagina and to decrease urinary incontinence. Just like normal exercise, doing this often will strengthen a female’s PC muscle. Anyone can practice Kegel exercises discretely almost anytime and anywhere (e.g., in their car, in their living room, etc.). Strengthening this muscle will add to the overall tightness of the vagina and will also give one stronger contractions during orgasm, which will make orgasms feel more powerful. For more information on how to locate and exercise the PC muscle, read this article!
Vaginoplasty
Vaginoplasty is a surgical procedure meant to tighten the female pelvic floor muscles surrounding the vagina. The goal of the procedure is to give a female better strength or control of these muscles, which can lead to greater satisfaction for both the female and her partner during sexual intercourse. The procedure was originally intended to fix genetic vaginal deformations or repair vaginal stretches and tears that are often the result of childbirth. Now, many females are also choosing to have the surgery for aesthetic reasons. For more information about the pros and cons of getting a vaginoplasty, read through this article!
Genital Self-Exam
Performing regular genital exams can help you better understand your body and learn what is normal for it. These exams can show you the physical changes that occur throughout the menstrual cycle. Regular self-exams are important because they increase the likelihood of discovering physical changes and abnormalities. This is important so that any changes can be discussed with a physician in a timely manner. Remember, the earlier a problem is detected and treated, the more likely it can be successfully controlled or cured. Female genital self-exams are key to early detection. However, self-exams should not replace annual pelvic exams performed by your gynecologist. These annual exams include Pap smears and other diagnostic tests designed to detect microscopic changes that cannot be found through self-examination. For a step-by-step guide on examining the vagina, check out this article!
Douching

Douching is the act of forcing water or some solution into the vagina with the purpose of cleaning it. It is usually done with plain water or some combination of water and vinegar, baking soda, or iodine. Douching may involve either rinsing or forcing the liquid at a high pressure into the vagina using a douche device. However, the vulva is naturally self-cleaning, so douching and using feminine deodorants is completely unnecessary. In fact, douching on a regular basis can upset the natural balance of bacteria found in the vagina and can lead to an increased risk of vaginitis. To keep your vulva healthy, simply eat healthy, exercise on a regular basis, wash it consistently with gentle soap and water, and wipe from front to back after going to the bathroom. If you wipe from back to front, you may accidentally infect the vagina with bacteria from the anus. For more information regarding cleaning the vagina, read this article on douching!
Contraception
Female Condoms

The female condom, like the male condom, is a barrier method of contraception. When worn during sex, the female condom lines the entire interior of the vagina, preventing semen from entering the uterus and fertilizing an egg. By shielding the walls of the vagina or anus from semen and other bodily fluids, the female condom also helps to prevent sexually transmitted infections (STIs). According to the United States National Library of Medicine, the female condom is about 75-82% effective in preventing pregnancy with typical use. Female condoms are a safe, convenient, and effective alternative to other methods of birth control. For more information regarding use of female condoms, read this article!
Vaginal Rings

The vaginal ring, most commonly known as the NuvaRing®, is a soft, flexible ring inserted into the vagina once a month for three weeks. The ring is a reversible form of birth control that steadily releases both estrogen and progestin hormones, similar to the combination pill. The vaginal ring prevents pregnancy but does not protect against STIs, so it should be used with a latex or female condom. The vaginal ring has very low failure rate. In studies, it has proven to be 99% effective, which is about the same as the birth control pill. The vaginal ring is convenient since it only requires insertion and removal every month. The vaginal ring contains fewer hormones than the average hormonal pill. For more information about the advantages and disadvantages of vaginal rings, check out this article!
Intrauterine Device (IUD)
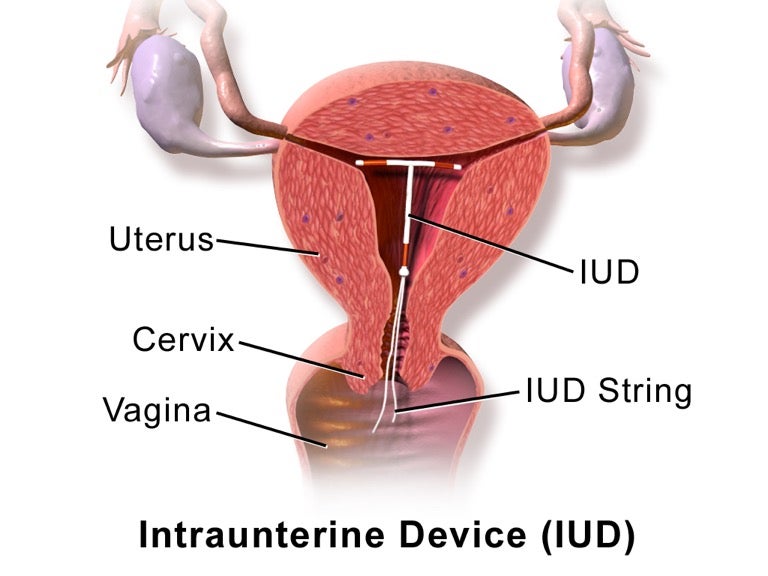
Intrauterine devices (IUDs) are plastic T-shaped objects that are inserted through the vagina and placed in the uterus to prevent pregnancy. IUDs are used for long-term, reversible contraception. There are two major types of IUDs: the copper IUD (marketed as Paragard) and the hormone-releasing IUD (marketed as Skyla, Mirena and Liletta in the United States). The copper IUD has a typical-use effectiveness of 99.2% (8 out of 1000 females will become pregnant in a given year). The hormonal IUD has a typical-use effectiveness of 99.9% (only 1 out of 1000 females will become pregnant in a given year), making it even more effective at preventing pregnancies than female sterilization (99.5% effective). The copper IUD can also be used as a form of emergency contraception if inserted within 5 days of unprotected sex. Since it does not protect against sexually transmitted infections (STIs), the IUD should be used with a male or female condom. For more information on the advantages and disadvantages of IUDs, read this article!
Medical Conditions
There are numerous medical conditions associated with the vagina. Several of the possible conditions that can affect the vagina are listed below.
- Chlamydia: Chlamydia is a sexually transmitted infection (STI) caused by Chlamydia trachomatis, a bacterium that infects and lives within human cells. Chlamydia is one of the most common STIs in the world, infecting approximately 4 to 8 million new individuals each year. Although chlamydia is spread primarily through sexual contact, it can also be spread from the genitals to the eyes by finger contact. Chlamydia infecting the eye, known as chlamydia conjunctivitis or trachoma, is one of the most common causes of blindness in the world. Symptoms of chlamydia in females may include spotting; abnormal or smelly vaginal discharge; and pain, itching, or burning around the vagina, especially during urination or sexual intercourse. However, many females infected with chlamydia do not experience noticeable symptoms.1 Chlamydia is easily and effectively cured by antibiotics; however, if left untreated chlamydia infections can result in serious reproductive damage as well as a number of other health problems including short and long-term consequences. Some consequences of untreated chlamydia in females include Pelvic Inflammatory Disease (PID), infertility, ectopic pregnancies, and premature births.1 Therefore, if you are sexually active, the only way to truly know if you have contracted any STIs is to contact your healthcare provider and get tested!
- Genital Warts: Genital warts are caused by an STI known as the human papillomavirus (HPV). Genital warts are transmitted easily by sexual contact, including oral, penile-vaginal (coital), and anal sex. HPV infection is the most common STI in North America and may cause cervical, penile, and anal cancer. The Centers for Disease Control and Prevention (CDC) estimates that at least 50% of sexually active individuals will contract a genital HPV infection at some time in their lives. Genital warts can appear in females on the vulva, vagina, cervix, and anus several weeks to months after a sexual encounter with an infected partner. Many females infected by genital HPV may experience no symptoms, as the genital warts may or may not be visible. Although the HPV virus is untreatable, the infection typically disappears from the body by itself.1
- Gonorrhea: Gonorrhea, sometimes referred to as “the clap,” is an STI that can be spread to both males and females. It is a bacterial infection caused by the bacterium Neisseria gonorrhoeae, or simply gonococcus. It is transmitted through any kind of unprotected penile-vaginal, oral-genital, oral-anal, and genital-anal contact with an infected individual. Therefore, any sexually active person is at risk for contracting gonorrhea. The bacteria can be spread even without penetration or ejaculation. Infants can contract gonorrhea from an infected mother during childbirth. Gonorrhea is a very common infection: The CDC estimates that in the United States about 820,000 people contract gonorrhea infections each year, though less than half of these new infections are detected. Females are usually asymptomatic; about 80% of females who are infected do not notice any symptoms. When symptoms do appear, infected individuals usually experience itching, dysuria (burning during urination), increased vaginal discharge (especially yellow or green in color), and/or vaginal bleeding. While these symptoms are irritating and concerning, they are often mistaken for signs of other health problems such as bladder or vaginal infections. Sometimes, females with gonorrhea may also have trichomoniasis, which can mask the presence of gonorrhea, making it difficult to detect. If left untreated, gonorrhea can lead to Pelvic Inflammatory Disease (PID) in females or, less commonly, to disseminated gonococcal infection (DGI) in both sexes.
- Herpes Simplex Virus (HSV): The herpes simplex virus is a viral infection that can affect the vulva, vagina, cervix, and anal area in females. There are two types of HSV. Herpes Type I is most commonly found above the waist, in the mouth, nose, and eyes, though it can be spread to the genitals via oral sex. Herpes Type II is most commonly located below the waist-on the genitals, thighs, and buttocks- but can be spread to the mouth via oral sex. Although genital herpes are commonly caused by HSV Type II, recent evidence shows that HSV Type I is also increasingly causing genital herpes. While it is common to experience no noticeable symptoms, possible symptoms of HSV may include tiny blisters, painful lesions, and fever. Persons infected with HSV are at an increased risk of acquiring HIV.1 There is currently no cure to completely eliminate both HSV-1 and HSV-2, but there are treatments used to alleviate symptoms.
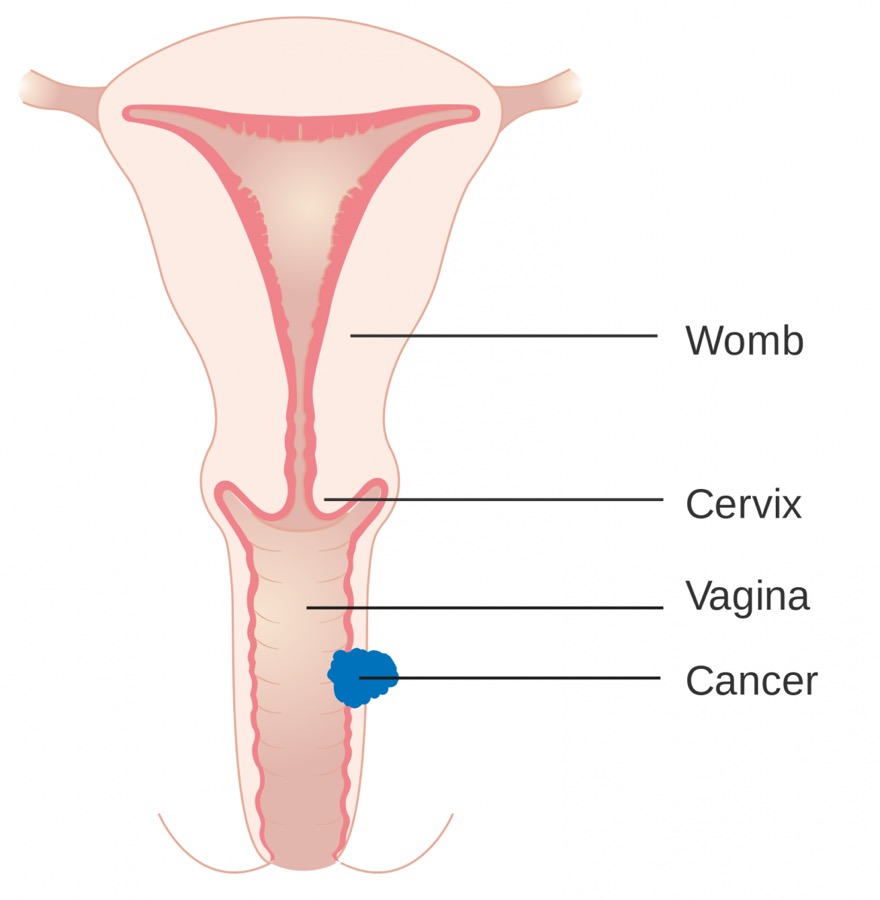
- Vaginal Cancer: Cancer is defined as the uncontrolled growth of abnormal cells in the body. Vaginal cancer is extremely uncommon. Risk factors of vaginal cancer include old age, HPV infection, history of cancer, and having a hysterectomy. Several treatment options are available for females with vaginal cancer. The most common treatment used for vaginal cancer is through surgical removal of the tutor. Vaginal cancer may be recurrent in some individuals. In these cases, the female is often given treatment typically used for cervical cancer, as treatment for recurrent vaginal cancer does not exist.1
- Vaginismus: Vaginismus is medically defined as involuntary spasms of the pubococcygeus (PC) muscles, the muscles which surround the vaginal canal. Vaginismus is a physical disorder that can stem from psychological or physiological factors. On average, one in every 500 females will experience vaginismus. However, the true number of females with vaginismus is estimated to be higher because many never report their condition or seek medical care due to fear or lack of knowledge. Females with vaginismus report an increase in vaginal tightness prior to or during penetration. This may include an instance that is sexual, such as intercourse, or even nonsexual, such as inserting a tampon or a speculum during a pelvic exam. This tightness can make penetration extremely painful, and in extreme cases, impossible. Treatment for vaginismus can include physical treatments such as Kegel exercises and vaginal dilators, and/or medical treatments such as Botox injections. It is imperative to seek medical help in order to properly treat vaginismus.
- Vaginitis: Vaginitis is the broad term for inflammation or infection of the vagina. There are many types of vaginitis; each of which is characterized by different causes and symptoms. Symptoms of vaginitis include vaginal itching and irritation, painful urination, pain during intercourse, light vaginal bleeding or spotting, and vaginal discharge that has a foul smell or strange color. These symptoms are characteristic of most vaginal infections and may vary or not occur at all depending on the type of infection present. The different types of vaginitis include the following:
- Bacterial Vaginosis: Bacterial vaginosis is an infection within the vagina due to an imbalance of healthy bacteria. Females with bacterial vaginosis typically have a decreased amount of healthy bacteria and an excessive amount of unhealthy bacteria. Douching, sex with a new partner, and sex with multiple partners can all disrupt the process of vaginal self-cleaning, leading to an imbalance of vaginal bacteria. Symptoms of bacterial vaginosis include foul-smelling vaginal discharge and discharge that appears gray or yellow. Typically, bacterial vaginosis is a mild infection that does not lead to other health problems unless the female is pregnant, has recently received a pelvic procedure, or has been exposed to an STI. Although symptoms of bacterial vaginosis usually disappear within a few days, it is best to see a doctor for a proper diagnosis and treatment.1
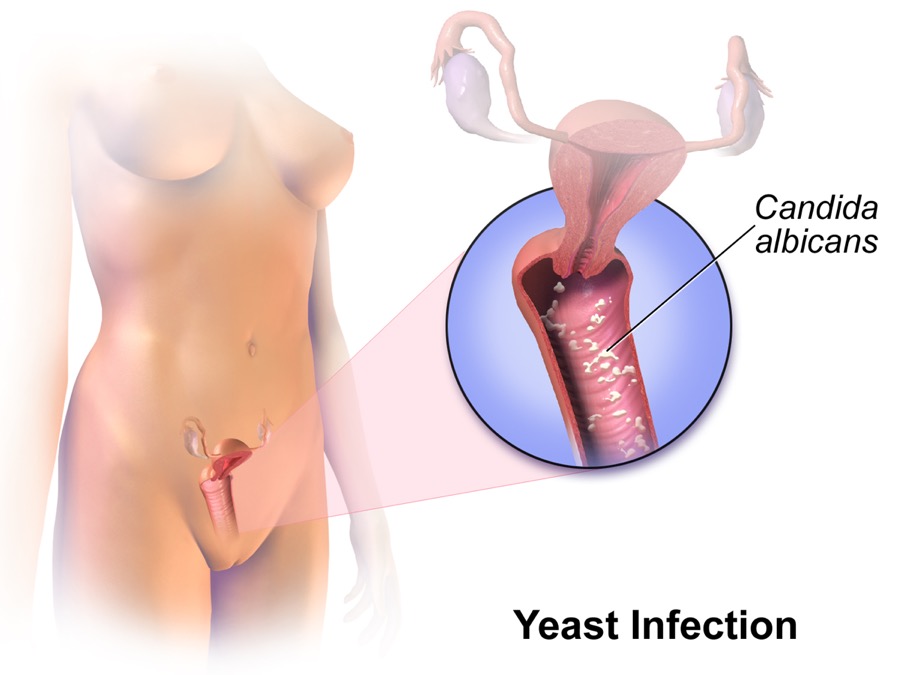
- Yeast Infections: Yeast infections are also known as genital/vulvovaginal candidiasis (VVC). The fungal yeast Candida is found in small quantities all over the body. When there is an overgrowth of Candida in the vulva, candidiasis occurs. This overgrowth can result from a hormonal imbalance or a change in the pH of the vagina. Symptoms usually include the burning, itching, or pain typical of other vaginal infections, as well as a thick, white, cottage cheese-like discharge. This type of infection is very common in both females who are sexually active and in females who are not sexually active. The Center for Disease Control and Prevention (CDC) reports that about 75% of females have had a yeast infection in their lifetime. A female is at a higher risk for contraction if she has a weak immune system. Candidiasis is common in pregnant females because of the hormonal changes that their body undergoes when carrying a child. Vaginal yeast infections are easily treatable through antifungal medications such as prescription pills or cream.15
- Trichomoniasis: Trichomoniasis is an infection of the vagina that affects roughly 5 million males and females each year. Trichomoniasis is one of the most common, curable causes of vaginal infection. Trichomoniasis is spread through sexual contact. The vulva, vagina, and urethra are the most common sites of infection in females. Trichomoniasis is often asymptomatic, meaning the disease shows no signs of being present. However, in cases where symptoms do arise, symptoms typically do not appear for several weeks after exposure to the infection. Females who eventually show symptoms may not show any for up to six months! Symptoms in females may include foul-smelling vaginal discharge that often appears green in color, dysuria (pain during urination), itching, spotting, and pain around genitals or abdomen. Trichomoniasis is easily curable. However, if left untreated, the infection can cause several complications in pregnant mothers-to-be including early delivery. Females infected with trichomoniasis have an increased risk of contracting the HIV infection.1
- Noninfectious Vaginitis: Inflammation of the vagina is not always a result of infection. Some females may experience burning, itching, and unusual discharge without the presence of an infection. Typically, noninfectious vaginitis occurs as an allergic reaction to douching or using vaginal sprays, scented soaps, detergents, and spermicides that can cause irritation of the vagina or vulva. Post-menopausal females or females who have had their ovaries or uterus removed sometimes experience vaginal atrophy, or the thinning of the vaginal walls that is caused by hormonal changes. Noninfectious vaginitis is treated by diagnosing and avoiding the cause of inflammation. If hormonal changes are responsible for the inflammation, estrogen pills can be prescribed by a doctor to alleviate symptoms.16
- Bacterial Vaginosis: Bacterial vaginosis is an infection within the vagina due to an imbalance of healthy bacteria. Females with bacterial vaginosis typically have a decreased amount of healthy bacteria and an excessive amount of unhealthy bacteria. Douching, sex with a new partner, and sex with multiple partners can all disrupt the process of vaginal self-cleaning, leading to an imbalance of vaginal bacteria. Symptoms of bacterial vaginosis include foul-smelling vaginal discharge and discharge that appears gray or yellow. Typically, bacterial vaginosis is a mild infection that does not lead to other health problems unless the female is pregnant, has recently received a pelvic procedure, or has been exposed to an STI. Although symptoms of bacterial vaginosis usually disappear within a few days, it is best to see a doctor for a proper diagnosis and treatment.1
Although the list above does not contain all possible infections related to the vagina, some of the most common are included. If an individual suspects that they may have a vaginal infection, it is best to consult a doctor for a proper diagnosis and treatment since self-diagnosing is highly unreliable.
Concluding Remarks
The incredible amount of information associated with the vagina can be intimidating to some, but it is very important to be familiar with this organ. Although many variations can occur from female to female, the vagina naturally experiences numerous changes throughout one’s lifetime. Performing genital self-examinations regularly not only increases one’s chances of finding irregularities, but can help one become more comfortable with their body. Overall, while the vagina is absolutely nothing to be ashamed of, it should be properly cared for with healthy eating, regular exercise, and consistent cleaning with soap and water.
References
- “The Vagina (Human Anatomy): Picture, Parts, Function, Definition, and Problems.” WebMD. WebMD, LLC, 2015. Web. 15 Apr. 2016.
- “Is My Vagina Normal?” NHS Choices. GOV.UK, 12 Jan. 2015. Web. 19 Apr. 2016.
- LeVay, Simon, Janice I. Baldwin, and John D. Baldwin. “Women’s Bodies.” Discovering Human Sexuality. 3rd ed. N.p.: Sinauer Associates, 2015. 29-32. Print.
- Peri, Camille. “What Girls Need to Know about Growing Up.” WebMD. WebMD, LLC, n.d. Web. 19 Apr. 2016.
- “The Stimulating Paradox of Female Desire.” Neuronarrative. WordPress, 02 Feb. 2009. Web. 19 Apr. 2016.
- “Cervical Mucus and Your Fertility.” American Pregnancy Association. American Pregnancy Association, 18 Jan. 2013. Web. 18 Apr. 2016.
- “Charting Fertility Cycle: Monitoring Your Fertility.” WebMD. WebMD, n.d. Web. 18 Apr. 2016.
- “Is It Normal to Have Vaginal Discharge during Pregnancy?” NHS Choices. GOV.UK, 05 Dec. 2015. Web. 18 Apr. 2016.
- Nall, Rachel. “What to Expect from Your First Period After Pregnancy.” Healthline. Health On The Net, 27 Oct. 2015. Web. 17 May 2016.
- Castleman, Michael. “So That’s How It Feels…” Psychology Today. Sussex Publishers, LLC, 01 July 2012. Web. 18 Apr. 2016.
- Kilchevsky, Amichai. “Is the Female G‐Spot Truly a Distinct Anatomic Entity?” ScienceDirect. Journal of Sexual Medicine, Mar. 2012. Web. 18 Apr. 2016.
- Leggitt, Kathryn. “How Does My Body Work During Childbirth? | Taking Charge of Your Health & Wellbeing.” Taking Charge of Your Health & Wellbeing. Regents of the University of Minnesota, n.d. Web. 18 Apr. 2016.
- “What to Expect During a Vaginal Delivery.” Healthline. Health On The Net, 31 July 2015. Web. 17 May 2016.
- “Vagina Changes after Childbirth.” NHS Choices. GOV.UK, 12 Jan. 2015. Web. 17 May 2016.
- “Vaginal Yeast Infections.” WebMD. WebMD, 17 Mar. 2014. Web. 17 May 2016.
- “Vaginal Infections.” WebMD. WebMD, 17 Sept. 2015. Web. 19 May 2016.
Last Updated: 2 June 2016.
