Table of Contents
What Is an STI?

A sexually transmitted infection, or STI, is a condition passed from one person to another through sexual contact. An infection occurs when a bacteria, virus, or parasite enters and grows in or on a person’s body, and STIs are infections that are transmitted sexually. STIs are also sometimes referred to as sexually transmitted diseases, or STDs. While the terms “STI” and “STD” are occasionally used interchangeably, “STI” is more comprehensive. STIs affect nearly 68 million people every year, and these cases consist of both previously established infections and newly acquired transmissions through sexual behavior.1 While STIs can be an uncomfortable topic to discuss with a sexual partner, it is important to have the conversation and to be armed with knowledge on the topic. Additionally, many STIs present asymptomatically, meaning that they do not cause obvious signs or symptoms. Because of this, it can be difficult to know with certainty whether or not a partner is STI-free since they might feel and appear healthy, so we highly recommend getting tested regularly.
Types of STIs
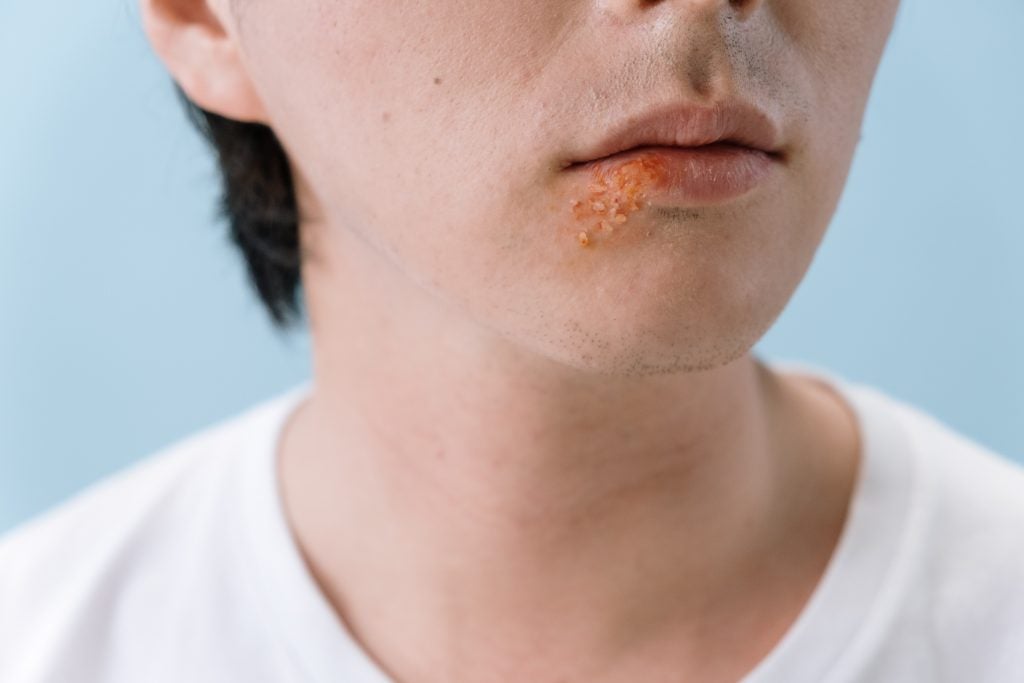
There are eight STIs that are considered to be the most common. Four of these infections are bacterial, and they are therefore curable. These bacterial infections are chlamydia, gonorrhea, syphilis, and trichomoniasis.1 The other four infections are viral, and they are currently considered incurable. These common viral infections include hepatitis B, herpes, HIV (Human Immunodeficiency Virus), and HPV (Human Papillomavirus).1 Chlamydia, trichomoniasis, genital herpes, and HPV currently account for 98% of all existing STIs and 93% of all new STIs.1 STIs are predominantly spread through different types of sexual contact, including penetrative vaginal, anal, and oral sex; however, some STIs can be spread via non-sexual routes, such as through a transmission of blood.
Who Is Affected?
The CDC estimates that, while anyone can contract an STI, certain groups such as young people or gay and bisexual males are at the greatest risk.2 Young people between the ages of 15-24 account for about half of all new STIs in the United States, and their care accounts for 26% of US healthcare system costs related to STIs.1 Young females are at a particular risk because of the serious long-term health consequences that an STI can create.3 For example, chlamydia left untreated in females can result in pelvic inflammatory disease (PID), which can sometimes lead to infertility (the inability to bear a child.) There are also many direct correlations that have been drawn between STIs and other illnesses, such as tumor-causing HPV, which is associated with nearly all cases of cervical cancer.4 While females may deal with more severe long-term effects of STIs, both males and females are at risk. Having an untreated case of herpes or syphilis can increase chances of contracting HIV by nearly three times, and this statistic is applicable to both males and females.2

Other factors that increase the risk of contracting an STI include having sex with multiple partners and engaging in unprotected sex (sex without a barrier method of birth control, such as condoms). The risk of acquiring an infection increases with the number of partners that a person interacts with, especially if one is not using proper protection with those partners. This is because there is a risk of being exposed to both the current partner’s possible infections and all their previous partners’ infections as well.
STIs can also be transmitted in a non-sexual manner, and it is important to consider this when engaging in higher risk behaviors. Certain STIs can be spread through intravenous drug use, so activities such as sharing needles may put an individual at risk for an STI.5 Additionally, depending on the identity of the infection, STIs can be passed from a mother to a child during both fetal development and birth.5
Prevention Methods
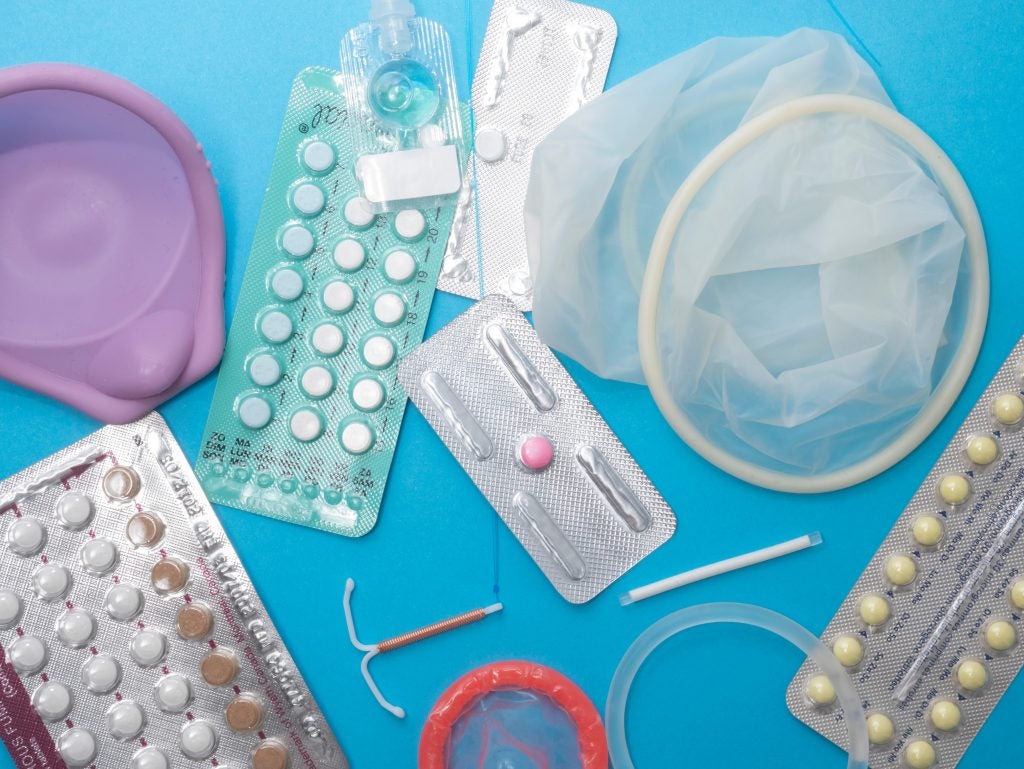
There are a multitude of ways to avoid sexual transmission of STIs. The three most effective methods are 1) abstinence, 2) a long term, mutually monogamous relationship with someone who does not have an STI, and 3) correct and consistent usage of barrier methods of birth control, such as male and female condoms.6 If a person chooses to be sexually active, both they and their partner(s) should undergo STI testing beforehand and should educate themselves on the different forms of protection. It is important to note that most forms of birth control do NOT protect against STIs, even if they do prevent pregnancy.
Hormonal birth control methods (e.g., the Pill, Depo-Provera, NuvaRing, Implanon, and Nexplanon) and other forms of pregnancy prevention like spermicide do not protect against STIs. Male latex condoms are one of the most effective methods of preventing STI transmission because they serve as a barrier to STIs passed through genital secretions. Condoms are also relatively inexpensive and accessible. Other barrier methods include dental dams, which protect from STIs during oral sex, and female condoms, which may give females a sense of shared responsibility and added peace of mind during sexual activity.6 The best way to be safe during sexual interactions is to communicate with a partner prior to any sexual activity and to discuss the importance of getting tested, using protection, and practicing safe sex. Approaching this subject beforehand can ensure all partners’ comfort and safety in the situation. Remember, “safe sex is great sex,” so taking the necessary precautions to protect each sexually-active partner can result in a better, more pleasurable experience.
Concluding Remarks
While talking and thinking about STIs may be difficult at first, being well-informed on the types of STIs, who they affect, and how to prevent them will make one better suited for navigating conversations about STIs with a sexual partner. STI prevention starts with communication, especially about sexual history/STI testing and methods of protection that partners are comfortable using. STIs are preventable, and with the proper practices one can keep themselves and their partner(s) safe.
References
- Sexually Transmitted Infections Prevalence, Incidence, and Cost Estimates in the United States. (2021, Jan 25). CDC. Retrieved Feb 16, 2021 from https://www.cdc.gov/std/statistics/prevalence-2020-at-a-glance.htm
- Sexually transmitted infections. (n.d.). Office on Women’s Health | Womenshealth.gov. Retrieved Oct 11, 2016 from https://www.womenshealth.gov/a-z-topics/sexually-transmitted-infections
- Sexually transmitted infections (STIs). (n.d.). World Health Organization. Retrieved Oct 11, 2016 from https://www.who.int/news-room/fact-sheets/detail/sexually-transmitted-infections-(stis)
- HPV-Associated Cancers and Precancers. (2015, June 4). CDC. Retrieved Feb 16, 2021 from https://www.cdc.gov/std/tg2015/hpv-cancer.htm
- Attia. (2020, April 29). Can you get an STD if you and your partner are both virgins? Planned Parenthood. https://www.plannedparenthood.org/learn/teens/ask-experts/can-you-get-an-std-if-you-and-your-partner-are-both-virgins
- ReCAPP: Statistics: Sexually Transmitted Infections (STIs). (n.d.). Resource Center for Adolescent Pregnancy Prevention. Retrieved Oct 11, 2016 from http://recapp.etr.org/recapp/index.cfm?fuseaction=pages.StatisticsDetail&PageID=558#:~:text=CDC%20estimates%20that%20nearly%2020,every%20year%20in%20this%20country.&text=Young%20people%20(ages%2015%2D24,of%20the%20sexually%20experienced%20population
Last Updated: 16 February 2021.
