An important part of becoming sexually active is learning how to take care of your sexual health. Any unprotected sexual act including vaginal, anal, or oral sex can potentially result in the transmission of a sexually transmitted infection (STI) if one or both sexual partners are infected. Additionally, a pregnant individual can also pass on an STI to their fetus during delivery.1 While some STIs are symptomatic, most are asymptomatic, meaning that they do not present any visible physical changes or signs of infection, and some can still be transmitted if they are asymptomatic.2 Other STIs may exhibit symptoms several weeks or months after the initial infection, which can lead to health complications and transmission to others if the carrier (infected individual) is engaging in unprotected sex.2 Being aware of your body, as well as attending regular doctor’s appointments, is vital to ensuring good physical health.3 Noticing possible symptoms, such as unusual changes in penile or vaginal discharge, the onset of rashes or growths, and genital itchiness or discomfort, can aid in the early detection of several STIs. Diagnosing STIs as soon as possible can reduce the risk of physical complications that may arise from postponing treatment, such as male or female sterilization.
Table of Contents
Common Symptoms of Sexually Transmitted Infections
While some sexually transmitted infections have symptoms, many are asymptomatic and can go unnoticed for months or possibly years.2 Symptoms can vary between individuals with penises and those with vaginas and can also depend on whether the infection was transmitted to the genital, oral, or anal region.3
STIs in the Genital Area:
Symptoms can also vary between different types of STIs, but are generally outlined as below:
- Excessive itching of the genital area.3
- A burning sensation while urinating.1,3
- Discharge or odor from the penis or vagina.1,3
- Sores, bumps, ulcers, or blisters on the penis or vagina.1,3
- Pain in the pelvic region.3
- Needing to go to the bathroom more often.3
- Pain or lumps in the scrotum or testicles.1
- Unusual bleeding from the vagina.3
- Experiencing painful sex for individuals with vaginas.3
If you find yourself experiencing any of the above symptoms it is best to visit a medical professional as soon as you can to get a proper diagnosis.
STIs in the Oral or Anal Regions:
While most STIs present in the genital region, some can be transmitted to the oral or anal regions via oral or anal sex. STIs that can be transmitted to the genital, as well as the oral and anal regions, include the following examples:
| STI | Transmittable to Oral/Anal Areas | Common Symptoms |
| Chlamydia | Throat and rectum.4 | Sore throat and rectal discharge.4 |
| Gonorrhea | Throat and rectum.4 | Sore throat and rectal discharge.4 |
| Syphilis | Mouth, lips, throat, anus, and rectum.4 | A single sore on the mouth, throat, or anus that becomes a rash.4 |
| Herpes Simplex Virus (Types 1 and 2): | Mouth, lips, throat, anus, rectum, and buttocks.4 | Blisters or sores on the mouth, lips, throat, anus, or buttocks.4 |
| Human papillomavirus (HPV): | Mouth, throat, anus, and rectum.4 | Small bumps in the anus, rectum, mouth, or throat.4 |
| Human Immunodeficiency Virus (HIV): | Mouth, anus, and rectum.4 | Usually asymptomatic but can present as flu-like symptoms around six weeks after infection.4 |
STIs That are Typically Asymptomatic:
Some STIs can be asymptomatic a majority of the time and some of them can still be transmitted even if there are no symptoms. This makes regular STI testing even more important because testing can help to avoid unwanted transmission. Some STIs that are typically asymptomatic include:
- Chlamydia.5
- Genital Herpes.5
- Gonorrhea.5
- Trichomoniasis.5
- Hepatitis types A, B, and C.5
- Human Immunodeficiency Virus (HIV).5
STIs that can be transmitted even if they are asymptomatic:
Regular testing is important to protect your sexual health, especially because some STIs can be asymptomatic and are still transmittable.
I Am Noticing Symptoms, Does This Mean I Have an STI?
Some of the previously mentioned symptoms of STIs are also symptoms shared by non-STIs. If you are experiencing certain symptoms, such as painful urination, yellow discharge, unpleasant genital odor, pelvic pain, or genital growths, these may be symptoms of non-STIs (e.g., urinary tract infections6, yeast infections7, bacterial vaginosis7, pearly penile papules8, and Fordyce spots9). If you find yourself experiencing any of these symptoms, you should still visit a medical professional, so they can diagnose you and prescribe you appropriate treatment.
STIs are generally divided into three categories that are dependent on the pathological nature of the disease: parasitic infections, bacterial infections, and viral infections. If you present any of these symptoms, visit your medical practitioner immediately for an official medical diagnosis.
Parasitic Infections
The most common parasitic infections are pubic lice (also known as “crabs”) and scabies. They can be transmitted through non-sexual contact (e.g., sharing towels, sharing clothing, sleeping in infested beds, or close physical contact) but are usually transmitted via sexual activity. Pubic lice and nits are generally smaller than head lice but are still visible on genital skin.
Pubic Lice
Pubic lice infestation is usually discovered by itching of the infected region. Other symptoms include:
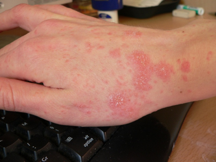
- Inflammation of the affected area.10
- Underwear showing a black powder.10
- Small spots of blood on the lower stomach.10
Scabies
Scabies are microscopic burrowing mites that are not visible with the naked eye:

- Small red bumps on the skin, including the buttocks, armpits, and elbows.10
- Excessive itchiness, particularly at night.10
- Secondary infections can arise from excessive scratching.10
Both parasitic infections are treated with topical creams or oral medications. Further actions, such as washing infested bedsheets and clothing are also required.
Bacterial Infections
Bacterial infections are some of the most common STIs in the United States, and they include chlamydia, gonorrhea, and syphilis.10
Chlamydia
Chlamydia is very common and also typically asymptomatic; only 30% of females and 50% of males experience symptoms.10 Symptoms associated with chlamydia include:
- Painful urination.10
- Lower abdominal pain.10
- Unusual white discharge.10
- Painful sex.11
Gonorrhea
Gonorrhea has similar symptoms to chlamydia, but 90% of males exhibit symptoms while only 50% of females do.10 These symptoms include:
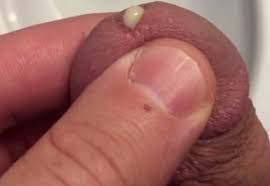
- Green or yellow discharge.10
- Painful urination.10
- Anal itching.11
- Heavy menstrual bleeding between periods.11
Syphilis
Syphilis has four stages: primary, secondary, latent, and tertiary:
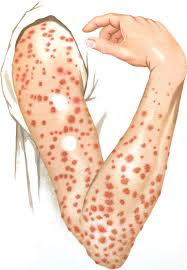
- Primary: chancre (red bump) at the site of infection.11
- Secondary: transitions into a painless rash that can be accompanied by fever, swollen lymph nodes, sore throat, and muscle pain.11
- Latent: no apparent symptoms.11
- Tertiary: large ulcers may appear on the skin or internal organs, potentially causing organ damage.11
All three of these STIs can be treated with oral or subcutaneous (under the skin) antibiotics.1
Viral Infections
Human papillomavirus (HPV), Herpes, and Human Immunodeficiency Virus (HIV) are the three most common viral STIs, and unfortunately, none are completely curable.1
Human papillomavirus (HPV)
HPV has approximately 200 different types and around 40 of those strains cause certain STIs on the genitals.12 Strains 6 and 11 are responsible for 90% of genital warts, which are soft pink bumps or cauliflower-like growths that can appear on the genitals or anus and are considered low risk since they typically cannot lead to cancer.12 However, some types of HPV can lead to anal cancer in both genders and cervical cancer in women. Preventative measures may be taken to reduce the likelihood of becoming infected with certain strains of HPV, which dramatically decreases the likelihood of developing cervical cancer in females. The vaccine, marketed as Gardasil® or Silgard®, is designed to prevent the acquisition of strains 6, 11, 16, and 18 of HPV and can be administered in a series of shots. Preferably, females should receive the vaccination before they become sexually active.12
Herpes
Herpes can be found on both the mouth and genitals of those infected, manifesting itself as blisters that may or may not be painful; simultaneous fever and swelling of the lymph nodes may occur. There are two types: Herpes Simplex Virus Type 1 (HSV-1) and Herpes Simplex Virus Type 2 (HSV-2). HSV-1 is typically spread through non-sexual contact, but if spread through oral sex it will present itself on the individual’s lips. HSV-2 spreads through bodily fluid, often during intercourse, and presents as blisters that may not be seen.3
Herpes is a lifelong condition and its outbreaks vary in terms of frequency, severity, and duration.12 Medications are available to mitigate symptoms, but even with their usage, the infected individual is contagious and must take extra precautions, such as refraining from sex during outbreaks or using barrier methods, even when there are no visible symptoms.3
Human Immunodeficiency Virus (HIV)
HIV can be acquired through sexual contact, the sharing of infected needles, and childbirth (from mother to child).3 During the initial stages of HIV, there are no clear indications of infection other than flu-like symptoms two to six weeks after infection, and these symptoms are easily mistaken for a different viral infection.12 Once the virus progresses to AIDS, the immune system is severely compromised and allows infection by opportunistic diseases, which are then usually the final cause of death in the victim.12 Fortunately, there are now regimens of antiretroviral drugs available that, if taken correctly, greatly improve the chances of survival and quality of life. Commonly known as ART (antiretroviral therapy), these drugs have raised the life expectancy after diagnosis.13
I Think I Have an STI. What Should I do?
We strongly encourage regular STI screenings every three months, which involves being tested for STIs without having any physical symptoms, especially for those who are at risk of contracting an STI. At-risk populations include those who are sexually active, those who are involved in sexual relations with people who have been diagnosed with incurable STIs, habitual intravenous drug users, and those who engage in riskier sexual behaviors (e.g., unprotected sex with multiple partners, sexual contact with sex workers, and anal sex).3 We recommend talking to your physician about your sexual history so that they can devise an STI screening schedule that is best for your sexual practices.
The ideal testing scenario involves both people getting tested before engaging in any type of sexual activity, whether it is protected or unprotected, because barrier methods (e.g., condoms) may break or slip off. If you have recently engaged in unprotected sex and are worried about the possibility of having contracted an STI, most medical facilities advise waiting a certain amount of time before getting tested in order to avoid false negatives. There are no screening tests for herpes as tests are generally only conducted when visible outbreaks are present. The general waiting periods are as follows:
- 2 weeks for gonorrhea and chlamydia.10
- 1 week to 3 months for syphilis.10
- 6 weeks to 3 months for HIV, and hepatitis C and B7.10
An official medical diagnosis is required for the treatment of any STI; diagnostic exams include pelvic exams, genital swabs, urine analysis, and blood analysis and are the only definite way to know if a person is infected.3 Rapid at-home HIV tests are now available for over-the-counter purchase, but confirmation of one’s HIV status by a physician is recommended, as drug therapy options for alleviating HIV symptoms still require an official medical diagnosis.14
If You Are Pregnant

Being pregnant can sometimes complicate the treatment for an STI. Some STIs such as chlamydia, gonorrhea, syphilis, trichomoniasis, and bacterial vaginosis can be cured during an individual’s pregnancy. Other STIs such as those caused by viruses cannot be cured during the pregnancy. However, there are some medications that can be used to reduce the risk of passing on the infection to the baby.15 Discuss your options with a medical professional who can determine the best treatment for your circumstances.
Concluding Remarks
Sexually transmitted infections come with negative stigmas, which can sometimes cause an individual to avoid getting tested for fear of learning that they have an STI. However, sexually active individuals should get tested approximately every three months to ensure their sexual health. If you feel that you may have symptoms, it is always best to visit a medical professional to receive a diagnosis and the appropriate treatment. For pregnant individuals, treatment can be more complicated, so staying up to date with all appointments can help to ensure both your health and the baby’s health. As always, your health and well-being should be the top priority in any sexual relationship you develop.
References
- Department of Health & Human Services. “Sexually Transmitted Infections (STIs).” Better Health Channel, Department of Health & Human Services, 27 May 2018.
- Parenthood, Planned. “How Can You Tell If You Have an STD?” Planned Parenthood.
- “What Are Sexually Transmitted Infections (STIs) or Diseases (STDs)?” Sexually Transmitted Infections: Symptoms, Diagnosis & Treatment – Urology Care Foundation.
- “Oral Sex and STIs.” American Sexual Health Association: Your Source For Sexual Health Information.
- How Do I Know If I Have an STI?, www.familyplanning.org.
- “Urinary Tract Infections: Causes, Symptoms & Treatment.” Cleveland Clinic.
- Parenthood, Planned. “Vaginitis & Yeast Infections: Symptoms, Signs and Causes.” Planned Parenthood.
- “Pearly penile papules.” U.S. National Library of Medicine. Oct 2009.
- “Fordyce spots.” DermNet New Zealand. DermNet New Zealand. N.p., n.d. Web. 18 Apr. 2017.
- NHS Choices, NHS, www.nhs.uk/common-health-questions/sexual-health.
- “Common STD Symptoms.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 13 Mar. 2018.
- Parenthood, Planned. “What Is HPV & How Do You Get It?” Planned Parenthood.
- “HIV Treatment Overview.” HIV.gov, 11 Jan. 2020.
- “Testing.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 3 Dec. 2019.
- “STD Facts – STDs & Pregnancy.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 28 Mar. 2016.
Last Updated: 5 May 2020.
