Herpes is a viral disease also known as HSV (Herpes Simplex Virus). There are more than 70 different strains of the herpes virus, although humans are susceptible to only four of them. There are two types of HSV. Herpes Type I is most commonly found above the waist — in the mouth, nose, and eyes — though it can be spread to the genitals via oral sex. Herpes Type II is most commonly located below the waist — on the genitals, thighs, and buttocks — but can be spread to the mouth via oral sex. There is currently no cure to completely eliminate either HSV-1 or HSV-2, but certain treatments are used to alleviate symptoms.
Table of Contents
- Symptoms
- Transmission
- Parent-to-Child Transmission
- Triggers for New Outbreaks
- Emotional Impact
- Treatment
- The Difference between Canker Sores and Herpes Cold Sores
- Other Herpes
- Sex and Herpes
- Concluding Remarks
Table of Contents
Symptoms

Most people who have herpes do not know it.10 Symptoms are often very mild and can be mistaken as an ingrown hair or pimple, or they can go unnoticed completely. Symptoms of HSV infection include fever, lymph-node enlargement, painful lesions, and a sluggish, lethargic feeling.1 The area can become red in color, and then tiny fluid-filled blisters may form. These sores can be quite painful. It is common for the first breakout to be very intense and to include multiple sores. Flu-like symptoms are common during the first outbreak.7 Eventually, after an outbreak, lesions crust over as the body heals itself. For people with vulvas, the main sites of the sores include the cervix, vagina, vulva, mouth, and lips.10 For people with penises, the main sites of the sores include the tip (glans) of the penis, the shaft of the penis, the mouth, and the lips.10 People with penises may also develop urethritis from HSV. The intensity of the breakouts typically decreases with each subsequent breakout, and after a year of infection the breakouts usually become quite manageable.
Transmission
The virus typically enters the body through a break in the skin (through the genitals, lips, or skin around or inside the mouth). Herpes can be spread from one part of the body to another part of the body through a process called autoinoculation. Spreading a sore to another site on one’s own body is uncommon; still, washing hands after touching any sore is a recommended preventative measure. One should be especially careful not to spread the virus to the eyes, as in some cases it can cause blindness.7 Although HSV-1 is primarily found in the mouth, it can easily be transferred to the genitals through sexual behavior, such as oral sex. Likewise, HSV-2 can be spread to the mouth, eyes, etc. When an open cold sore lesion is present, there is a large chance of spreading the infection to other people, so the infected person should avoid direct or indirect contact with others, such as kissing and sharing drinks. Touching an active sore with the fingers allows transmittance of the virus via the fingertips. Therefore, if an individual has a sore, it is important for them to thoroughly wash their hands with soap and water after touching the infected area.
Fortunately, many people experience early symptoms — itching, tingling, and/or burning sensations — before the onset of an outbreak. People with herpes can learn to pay attention to tingling sensations or warmth in the infected area before a sore appears. They should then refrain from participating in any sexual behavior with their partner(s) that might spread HSV. A person can also use their prodromal symptoms to their benefit by applying preventative ointments to the tingling areas. It is possible to transmit herpes even when sores are not present due to a process called viral shedding; during this process, viruses are released from the body even when no sores are present. Asymptomatic shedding from the site where sores previously appeared may occur randomly up to three to six days or more each year. Thus, people with oral HSV who are sexually active should use condoms during every sexual encounter.7

It is also possible for a person infected with herpes to be asymptomatic (never show any symptoms). Asymptomatic individuals may be unaware that they are a carrier, but can still transmit the infection to others.
Parent-to-Child Transmission

If a pregnant person with a vagina has genital herpes, it is of utmost importance that they go to prenatal care visits. It is necessary for people to tell their doctor if they have ever had symptoms of, been exposed to, or been diagnosed with genital herpes. In some cases, genital herpes infection can lead to miscarriage. Genital herpes also increases the chance that a baby will be delivered prematurely. Herpes infection can be passed from a person with a vulva to an unborn child and cause a potentially deadly infection in the child, called neonatal herpes. It is especially important to use protection during sexual activity to avoid contracting herpes during pregnancy.
Pregnant people with vulvas may be offered herpes medicine toward the end of pregnancy to reduce the risk of having any symptoms during the time of childbirth and passing the infection to the baby. At the time of delivery, a physician should carefully examine the pregnant person for symptoms. If any herpes symptoms are identified before delivery, a Cesarean delivery, or “c-section” is usually performed.5
Triggers for New Outbreaks

Most of the time, people with HSV are asymptomatic and do not have any sores. The following triggers reactivate viral particles and can cause new outbreaks:
- Emotional changes or stress.
- Physical stress, fatigue, or exhaustion.
- Illnesses like a cold, the flu, or an upper respiratory infection.
- Menstruation or pregnancy. For many people with vulvas, cold sores are more frequent around the time of their monthly periods.
- Immune system weakness or deficiency.
- Injury or physical trauma to the lips or surrounding skin, such as a bite, scrape, cut or dermabrasion (for cases of oral herpes).
- Exposure of the lips to sunlight, sunburn, or an ultraviolet light source (for cases of oral herpes).
- Exposure to extreme dryness, wind, or cold.
- Dental treatment (for individuals with oral herpes). This includes dental injections, periodontal procedures (gum work), tooth extractions, and any other non-dental surgical procedures performed in the orofacial area.3
Getting adequate rest, exercising regularly, and eating well are all great ways to reduce stress and strengthen your immune system.6
Emotional Impact
Viral shedding makes herpes one of the more difficult STIs to cope with on an emotional level, as there is currently no available cure. Oral herpes can be especially difficult as it is often visible and generally lasts for two weeks at a time. However, although herpes cannot be cured, it can be managed, and herpes outbreaks become less and less frequent and severe as time passes. Due to the stigma that many people associate with sexually transmitted infections (STIs), many people feel anxious or hesitant to talk to their partner about having herpes. It is necessary for people infected with herpes to tell their sexual partner(s) and inform them of the risk involved. Using condoms may help lower the risk of transmitting herpes to a partner, but it will not eliminate the risk completely. Additionally, Valtrex, an antiviral drug used to control herpes, can be used in combination with a condom to further decrease the chance of transmission. Being aware of these methods to decrease transmission often comforts people with herpes who worry about transmitting the virus to their partner(s).
The herpes diagnosis may also become easier to accept once a person realizes how common herpes is. Almost 50% of children entering kindergarten and 90% of adults have been infected with either oral or genital HSV, although a much smaller percentage have experienced symptoms.7 Although most people have been exposed to HSV and are carriers of the virus (meaning they can transmit it to others), only about 1 in 3 people will have visible symptoms or outbreaks in their lifetime.3 In regards to genital herpes in the United States, about one out of every six people aged 14 to 49 years are infected.5 I kind of hate this sentence. Alternative: Overall, experiencing emotional stress due to herpes is normal and may be alleviated by talking to a therapist.
Treatment
Although there is no cure for herpes, there are some treatments available that can decrease the frequency, length, and intensity of each outbreak. Some antiviral medications can be used when experiencing early symptoms in order to preemptively lessen the severity of the oncoming outbreak. They can also relieve pain during the outbreak or soften HSV scabs on the skin. Other medications can be taken daily for more serious cases.1 Currently available treatments include the following:
- Denavir (penciclovir cream), a topical antiviral cream recently approved by the FDA that may decrease the period of lesion pain and quicken healing.
- Acyclovir (Zovirax) or valacyclovir (Valtrex), taken orally, may decrease symptoms if started within 24-48 hours after the onset of symptoms.
- A moistened styptic pencil may relieve symptoms if used several times a day.
- Zinc oxide ointment is meant to be used after crusts have formed.
- A drying agent (like a Blistex ointment or 70% rubbing alcohol) that is best if used when sores first appear.
It is not recommended to use steroid ointments, dye-light therapy, smallpox vaccination or vitamin therapy (unless otherwise directed by a physician). These methods are ineffective and oftentimes make the sores worse.7 Please contact a physician if you think you might have herpes to discuss possible treatment options.
The Difference between Canker Sores and Herpes Cold Sores
Canker Sores
Canker sores and cold sores are commonly mistaken for one another but have very different implications. A canker sore is a painful ulcer, or open sore, that can usually be found on the movable parts of the mouth, such as the tongue or the inside linings of the lips and cheeks. Individuals can have more than one canker sore at any given time, and sores can recur throughout one’s life. Canker sores begin as small oval or round reddish swellings, which usually burst within a day. The ruptured sores are covered by a thin white or yellow membrane and are edged by a red halo. They typically heal within two weeks. The main cause of canker sores is viral infection, which can be brought on by injury to the mouth due to dental work, aggressive teeth cleaning, or biting the tongue or cheek.4
Unlike cold sores, canker sores are not contagious, and are not caused by the herpes virus. They occur in females more often than males and can occur at any age, but initial cases generally occur between the ages of 10 and 20. In most cases, canker sores will heal without any medication, but depending on the severity of infection they may need to be treated with an antibiotic or an anti-viral medicine.8
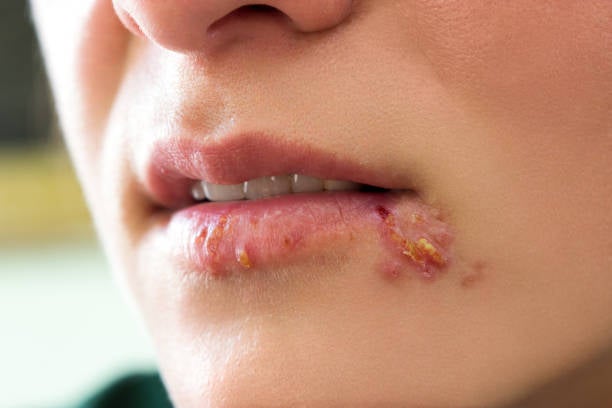
Cold Sores
Cold sores, however, are contagious and usually occur outside of the mouth. They tend to appear on the lips, chin, or cheeks; in the corner of the mouth; in the nostrils; or, rarely, in the eye.4 Cold sores, also known as fever blisters, are clusters of blisters that appear clear at first and then become cloudy. Ninety-five percent of recurring cold sore outbreaks are caused by HSV-1, as opposed to HSV-2.7 The sores usually run their course within 8 to 12 days, during which they undergo five stages that are detailed below.4
Stages of a Cold Sore
Herpes cold sores progress in a series of stages: tingling, blistering, weeping, crusting, and healing. In total, these stages generally take 8 to 12 days.
Stage 1: Tingling (Days 1-2)
When a cold sore is beginning to form, the individual may notice a new sensation — such as burning, stinging, itching, soreness, tautness, or swelling — in the area where the lesion will later appear.
Visible Signs: The area may become red and slightly raised or elevated.
Why This Happens: These initial symptoms are signs of the body’s reaction to the herpes virus and the subsequent inflammation and tissue damage the virus is beginning to cause.
Stage 2: Blistering (Days 2-3)
The first definite sign of cold sore formation is the appearance of multiple fluid-filled blisters.
In about one in four cases, the infection is brought under control (either just by the immune system or with the help of a medication) before any blisters can form and progress to the next stages. Since no blisters form, these are referred to as “failed” or “aborted” lesions.
Visible signs: The blisters are usually smaller than a dime and form a cluster that is no larger than a nickel. Sometimes, multiple blisters may merge to form a single large blister.
Why This Happens: This is the stage where the total number of herpes virions, or HSV virus particles, is the greatest. The relative size of the forming lesion is generally related to the number of virions. Therefore, blisters form as a result of increased herpes virions.
Stage 3: Weeping (Day 4)
The blisters generally rupture soon after they have appeared. As they burst, they discharge a clear fluid packed with herpes virions. After they have ruptured, the sores become ulcers. During this phase sores are the most contagious and the most painful.
Visible Signs: Immediately after rupture, the lesion starts as a shallow red ulcer, looking moist and raw, and then becomes gray.
Why This Happens: By this time, the replication rate of the virus has passed its peak. Additionally, the inflammatory response activated by the virions and the skin-cell damage that the virions cause are well under way. This inflammation reaction is responsible for the redness, swelling, and tenderness linked to cold sores as they progress through their stages.
Stage 4: Crusting (Days 5-8)
If the ulcer is in a location that is not kept moist from the mouth, it will scab over. The scabbing process is accompanied by an itching or burning sensation. Moisturizing the scab can aid in the healing process.
Visible Signs: The scabbing looks like a yellow, dark red, or brown crust. It often cracks, which can cause bleeding. When a scab comes off, the remaining ulceration and the freshly formed pink surrounding tissue become visible. The tissue is still contagious, but less so than the previous stage.
Stage 5: Healing (Days 8-12)
Visible Signs: A series of scabs will typically form on the lesion; each scab will shed before it is replaced by a new one. The scabs will continue to decrease in size, until finally the lesion will resolve fully, and in most cases, there will not be any scarring.3
Unfortunately, once a person has an outbreak of cold sores, the herpes simplex virus remains in the body for life, and can be transmitted to others. The virus lies dormant in the nerve cells of the skin and can re-emerge as an active infection around the site of the original outbreak. The cold sores will appear only during an outbreak, which can be brought on by fever, stress, or exposure to the sun. After the outbreak passes, the virus retreats back into the nerve cells. Though cold sores cannot be cured, antiviral medications can help reduce their frequency and to limit the duration of an occurrence.4
Other Forms and Types Herpes
HSV is the most common herpes virus; however, there are three other common types that can have adverse effects on a person’s health. Cytomegalovirus (CMV) is spread through contact with an infected person’s bodily fluids, including saliva, urine, semen, and breastmilk. In the United States, nearly one in three children is infected with CMV by age 5, and more than half of adults have been infected with CMV by age 40. Symptoms of CMV include fever, swollen lymph nodes, fatigue, and sore throat. However, most people who have CMV are asymptomatic, as people with healthy immune systems are generally able to prevent the virus from causing illness. CMV can also be transferred from a pregnant individual to their fetus. Babies born with CMV can have brain, liver, spleen, lung, and growth problems, and most commonly suffer from hearing loss. In people with weakened immune systems, CMV can cause more serious symptoms affecting the eyes, lungs, liver, esophagus, stomach, and intestines.5
Varicella-zoster virus (VZV) can cause the common diseases chickenpox and shingles. People can greatly reduce their chances of contracting both diseases by getting the respective vaccinations.1 The fourth type of herpes virus is Epstein-Barr virus (EBV), which can cause infectious mononucleosis (commonly referred to as mono), hairy leukoplakia, and Burkitt’s lymphoma. Symptoms of EBV include fever, swollen lymph nodes, fatigue, and rash. EBV primarily affects children and is most often spread through saliva.
Sex and Herpes

Individuals with herpes can still have a fulfilling sex life after a herpes diagnosis, although sexual activity may require more precautions than before. If a person has a genital sore or feels one coming on, it is recommended that they avoid sexual intercourse.5 Those who have cold sores around the mouth or feel one coming on should avoid kissing and oral sex with their partner(s). Between outbreaks, it is okay to have sexual intercourse or oral sex as long as both partners are aware of the risks and give their consent. Using protection during sex such as internal condoms, external condoms, and dentals dams may help decrease the risk of spreading herpes, but these tactics will not completely erase the risk. 5 During the time of an outbreak, people can engage in alternative sexual activities. For example, if someone who has oral herpes experiences a flare up, they can engage in sexual intercourse with a condom and without any oral exposure, meaning no kissing or oral sex. If someone who has genital herpes experiences a flare up, they should not engage in penetrative or oral sex with their partner, even with a condom, since there may be infectious sores that are not covered by the condom.9 A person with genital herpes experiencing a flare up can engage safely (make sure to have clean hands) in mutual masturbation with their partner(s), an activity where partners masturbate next to each other. People experiencing a herpes outbreak can also engage in sexual interaction with their partner(s) through the use of sex toys. Sex toys should never be shared and should be properly cleaned before and after each use. With careful monitoring of outbreaks, open communication with partners, and implementation of alternative sexual activities during an outbreak, it is possible to have a fulfilling sex life with herpes.
Concluding Remarks
This article has hopefully provided information and resources pertaining to Herpes. Symptoms of HSV infection include fever, lymph-node enlargement, painful lesions, and a sluggish, lethargic feeling. Herpes is not curable, but it is treatable and controllable with a variety of topical and oral medications. Many people experience negative feelings surrounding their herpes. However, negative emotions about herpes can be alleviated. By discovering that herpes is normal and common, learning to control herpes outbreaks, and understanding how to maintain a healthy and fulfilling sex life, individuals are often able to accept their herpes.
Feel free to check out this informative video about herpes!
References
- Greenberg, J. S., Bruess, C. E., & Oswalt, S. B. Exploring the Dimensions of Human Sexuality. Jones & Bartlett Learning. 2014. Print.
- “Cytomegalovirus (CMV) Infection.” Definition. Mayo Clinic, 4 Apr. 2014. Web. 23 Apr. 2014.
- “Cold Sore (fever Blister) – Stages / Identification / Pictures / Signs & Symptoms.” Cold Sore (fever Blister) Stages – Pictures, Signs & Symptoms. N.p., n.d. Web.
- “Cold Sores & Fever Blisters.” Cold Sores/Fever Blisters-What Are They? What’s the Difference? N.p., n.d. Web.
- “Genital Herpes – CDC Fact Sheet.” Centers for Disease Control and Prevention. Centers for Disease Control and Prevention, 21 Feb. 2017. Web.
- Jocelyn. “Herpes Myths vs. Facts.” International Herpes Resource Center. N.p., n.d. Web.
- “University Health Service.” Cold and Canker Sores | University Health Service. N.p., n.d. Web.
- “What Is the Difference between a Cold Sore and a Canker Sore? Is It True That If You Have a Canker Sore, You Have Herpes? » Scienceline.” Scienceline. N.p., 05 Mar. 2010. Web.
- “My Partner has Herpes.” Response. Planned Parenthood. Jan 15 2020. Web. May 10 2022.
- “Genital Herpes.” Symptoms. Mayo Clinic, 10 May 2022. Web.
Last Updated: 24 May, 2022.
