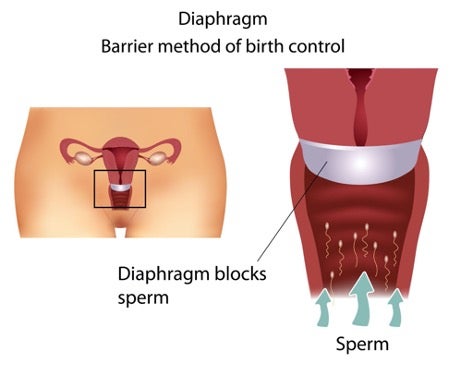
The diaphragm, a shallow silicone cap, is a barrier method of birth control for people with vulvas. Inserted deep within the vagina, the diaphragm creates a seal against the cervix to prevent sperm from entering the uterus.1 Spermicidal foam, cream, or jelly is applied onto the diaphragm before insertion to immobilize and kill sperm before they enter the uterus.1 Once professionally fitted by a healthcare provider, the diaphragm may be used repeatedly.1 The diaphragm should be checked annually during a gynecological exam and replaced every two years or when there are any signs of damage.1
The diaphragm is about 94% effective with perfect use and 88% effective with typical use.2 The diaphragm does not offer protection against the transmission of sexually transmitted infections (STIs).1 It should be used with another barrier method, like an internal or external condom, for STI protection.

Table of Contents
History of the Diaphragm
The diaphragm was first introduced as a contraceptive method in the late 1800s in Germany.3 Birth control activist Margaret Sanger introduced the diaphragm to the United States in the early 1900s, despite its production and distribution being illegal due to a law prohibiting “obscene goods.”3 Contraceptive diaphragms began to be manufactured and distributed in many countries and became the main method recommended by birth control clinics and doctors by around 1940.4 However, its popularity decreased as more high-tech and reliable birth control methods, such as the pill and the IUD, became available in the 1960s and 70s.4
The FDA approved a diaphragm for the first time in 2002, but this brand was later discontinued due to design flaws.3 A new brand of diaphragm, Caya, became popularized after this and is still one of the most popular diaphragm brands on the market.3 Its main appeal to many people is that a person with a vulva can be in control of pregnancy prevention. However, the diaphragm continues to decrease in popularity as a birth control method. According to the CDC’s reports in 2010, less than 0.01% of women in the U.S. rely on the diaphragm for contraception.4
Types of Diaphragms
Diaphragms come in different shapes and materials to fit the needs of each individual. These are the main four types of diaphragms:5
- The arching spring diaphragm: most common, has a firm rim, and is easiest to insert.5 It is usually made of latex.
- The coil spring diaphragm: softer, more flexible rim, requires stronger vaginal muscle tone.5 It is usually made of latex.
- The flat spring diaphragm: thinnest rim and most flexible, may need a tool to be inserted, suitable for people with very strong vaginal muscle tone.5 It is usually made of latex.
- The wide seal rim diaphragm: the main silicone option suitable for people with latex allergies. Can come in different styles, including the ones described above.5

Diaphragm Fitting
If you are interested in getting a diaphragm, you must obtain a prescription from a medical doctor or nurse. A fitting for the proper size and style of the diaphragm is necessary to receive a prescription.6 At the initial fitting, the clinician will have you practice inserting and removing the diaphragm yourself. Therefore, people with vulvas who choose this birth control method should feel comfortable inserting fingers into their vagina and should be able to locate their cervix. The fit and condition of the diaphragm must be rechecked once a year at a gynecological exam.6 You may need to schedule another diaphragm fitting with your healthcare provider if you:
- experience pain or discomfort
- have difficulty urinating or experience frequent urinary tract infections (UTIs)5
- have a pregnancy, miscarriage, or abortion5
- have pelvic surgery5
- gain or lose more than 10 pounds5

How To Use a Diaphragm
A diaphragm can be inserted up to two hours before intercourse,1 but the efficacy of spermicidal foam, cream, or jelly reduces over time. If it has been more than two hours after the diaphragm was inserted or you have intercourse more than once, use an applicator to insert more spermicide deep into the vagina1. Be sure to leave the diaphragm in place as more spermicide is inserted. The diaphragm must remain in place for at least six hours after intercourse.1 Diaphragms should be removed at least once every 24 hours to avoid irritation and infection, which could both lead to toxic shock syndrome.7 Petroleum jelly or other oil-based products should not be used on the diaphragm because these products can damage it and decrease its efficacy.5
Using a diaphragm during a person’s menstrual period may increase the risk of infection due to the accumulation of blood, so diaphragm users might want to consider using a different birth control method during their period.7
Diaphragm Insertion
Before you insert a diaphragm, make sure that it is not damaged or torn. Once you are sure that the diaphragm is clean and undamaged, the following steps can be used for insertion:
- Wash your hands with soap and water.
- Hold the diaphragm with the concave cup facing upwards. Place about one tablespoon of spermicide, possibly more or less depending on the instructions on the package of the diaphragm, into the cup. Spread it around the inside of the cup and along the edges.
- Find a comfortable position for insertion. It is usually easiest to squat, lie down, or prop up one leg.5
- Pinch the rim of the diaphragm between your thumb and fingers. Be sure not to squeeze out any of the spermicide.
- With your other hand, spread the inner lips of your vulva. Carefully insert the diaphragm into the vagina with the hollow side facing up into the vaginal opening. Push the diaphragm up into the vaginal canal as far back as it will go until you reach the cervix.
- Use your finger to tuck the edge of the rim behind the pubic bone (at the front of your body behind the mons pubis), and make sure the diaphragm lays snugly against the cervix.
After insertion, you should not be able to feel the device. If the fit feels uncomfortable, remove the diaphragm, and repeat the insertion process, making sure to reapply spermicide. If it continues to be uncomfortable, contact your doctor about size adjustment and refitting.
Diaphragm Removal
With a bit of practice, removing the diagram after intercourse should become a simple process. Be sure to wait at least six hours following your last act of intercourse before removing the diaphragm.1 To remove the diaphragm, use your index finger to lift the front rim of the diaphragm away from the cervix. Pull the diaphragm down and out of the vagina.1
After removal, wash the diaphragm thoroughly with mild soap and warm water. Perfumed soaps and powders should not be used because they may weaken the rubber or cause vaginal irritation or infections.5 Allow the diaphragm to air dry. The diaphragm should be stored in its plastic container in a cool, dry place. With proper care and use, one diaphragm can last up to two years.1
Advantages of the Diaphragm
The diaphragm may appeal to people that are looking for a less expensive barrier method contraceptive. Some of the specific advantages of the diaphragm are:
- It is a relatively inexpensive form of birth control1
- It is reusable
- Little to no side effects reported by users5
- Allows immediate return to fertility
- Non-hormonal
- People who are breastfeeding can safely use the diaphragm for contraception
- Allows for some spontaneity because it may be inserted up to six hours before intercourse and left in place for up to 24 hours5
- Most people report that they and their partners cannot feel the diaphragm during sex
- Allows the person with a vulva to be in control of contraception
Disadvantages of the Diaphragm
The diaphragm is not the right birth control method for everyone, especially those who may have a hard time remembering to use birth control with every occurrence of vaginal penetration.1 In addition, the diaphragm may be difficult for some people to insert or remove.1 Some individuals find that the diaphragm becomes dislodged during sex in certain positions.1 If this occurs, stop the sexual act immediately and reposition the diaphragm. Some people experience irritation from spermicide.1 If this occurs, discontinue use, and speak with a doctor. The diaphragm also does not protect against STIs, so another barrier method must be used alongside the diaphragm for proper STI protection.1
Furthermore, the diaphragm is not a recommended form of birth control for people who:
- Are allergic to silicone, latex, or spermicidal foams, creams, or jellies
- Are at a high risk of or have HIV/AIDS1
- Are at high risk for pregnancy and intend to use the diaphragm as their only birth control method
- Have vaginal or pelvic organ abnormalities that interfere with the fit and retention of the diaphragm
- Have a vaginal or pelvic infection
- Have frequent urinary tract infections (UTIs)1
- Have a history of toxic shock syndrome (TSS)
- Have recently given birth, had a miscarriage, or had an abortion
Cost and Pricing
A diaphragm is one of the most cost-effective types of barrier methods for contraception. Prices of the diaphragm vary based on your health care coverage and location. In the United States, if you have insurance it is likely that you can acquire a diagram and fitting free of charge or at a significantly reduced cost.1 Without insurance, a diaphragm, fitting, and exam can cost up to $250.1 The cost of spermicide, about 5-15 dollars per kit, is not included in this price.1 Since the diaphragm can last up to two years, this cost is relatively low compared to other birth control methods.

Concluding Remarks
The diaphragm is a non-hormonal barrier method of birth control that has been around since the 1800s.3 A diaphragm must be fitted by a medical professional and a single diaphragm can be used for up to two years.1 Although the diaphragm is not for everyone, it is a relatively cheap and simple birth control method. Diaphragms allow the person with a vulva to be in control of their contraception and allows for some sexual spontaneity.
References
- Planned Parenthood Federation of America. “Diaphragm.” Plannedparenthood.org. 2022.
- Bartz, Deborah A. “Pericoital contraception: Diaphragm, cervical cap, spermicides, and sponge.” UpToDate. Version June 2022, last revised September 11, 2020.
- Drucker, Donna J. “Chapter 2: Contraception Before the Pill.” Contraception: A Concise History. The MIT Press: 2020.
- Planned Parenthood Federation of America. “A History of Birth Control Methods.” plannedparenthood.org. Katharine Dexter McCormick Library and the Education Division of Planned Parenthood Federation of America: New York, NY, last updated January 2012.
- Familydoctor.org editorial staff. “Birth Control: How to Use Your Diaphragm.” American Academy of Family Physicians. Last updated July 27, 2020.
- Planned Parenthood Federation of America. “How Do I Get a Diaphragm?” Plannedparenthood.org. 2022.
- Sexual Health and Family Planning Act. “Diaphragms.” shfpact.org.au. 2022.
- Eisenstein, Lea. “From Icon to Bygone: The Rise and Fall of the Diaphragm in Twentieth-Century America.” University of Pennsylvania ScholarlyCommons. 5-2019. University of Pennsylvania: 2019.
Last Updated 24 May 2022.
